Содержание
- 2. Objectives I. Pharmacokinetics Absorption Bioavailability Distribution Drug metabolism Excretion II. Combined action of drugs
- 3. Pharmacokinetics Pharmacokinetics (from Greek pharmakon - medicine, kineo - move) Pharmacokinetics is the part of pharmacology
- 4. Pharmacokinetics Based on the hypothesis that the action of a drug requires presence of a certain
- 5. Pharmacokinetics Drug Movement in the Body Absorption Distribution Metabolism Excretion ADME profile
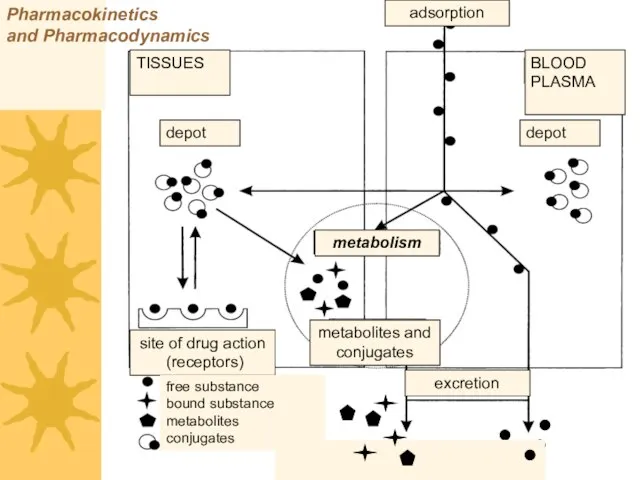
- 6. Pharmacokinetics and Pharmacodynamics TISSUES BLOOD PLASMA depot depot metabolism site of drug action (receptors) metabolites and
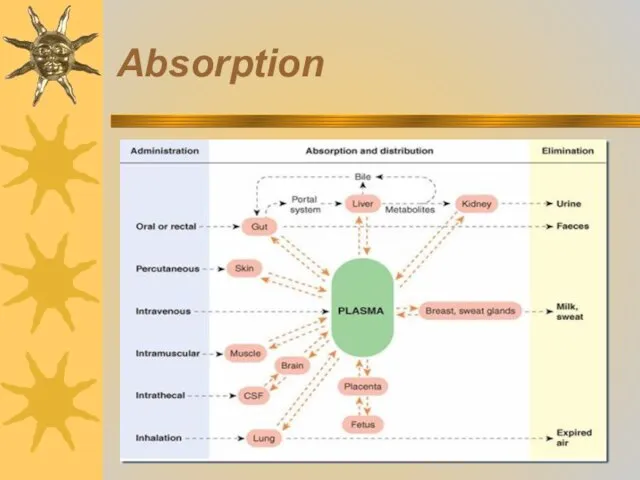
- 7. Absorption The usage of drugs starts with their administration into the organism or application onto body
- 8. Absorption
- 9. Absorption
- 10. Absorption of drugs from the gastrointestinal tract through the skin, respiratory and vascular walls is connected
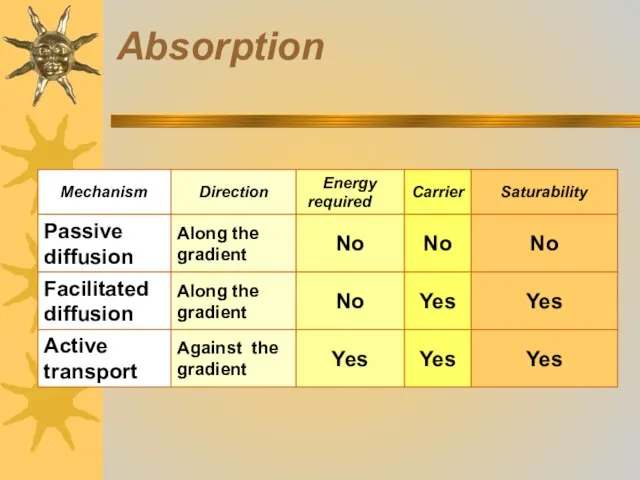
- 11. Passive diffusion: substances move from the area with high concentration to the area with low concentration
- 12. Absorption
- 13. Passive transport
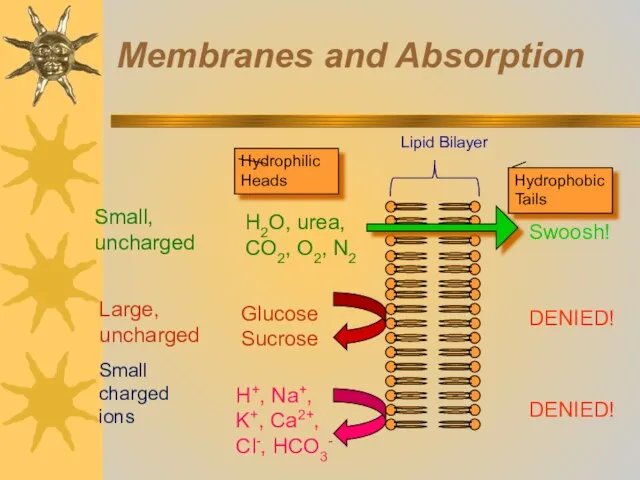
- 14. Membranes and Absorption
- 15. Facilitated transport
- 16. Active transport
- 17. Pinocytosis
- 18. Factors that influence the absorption
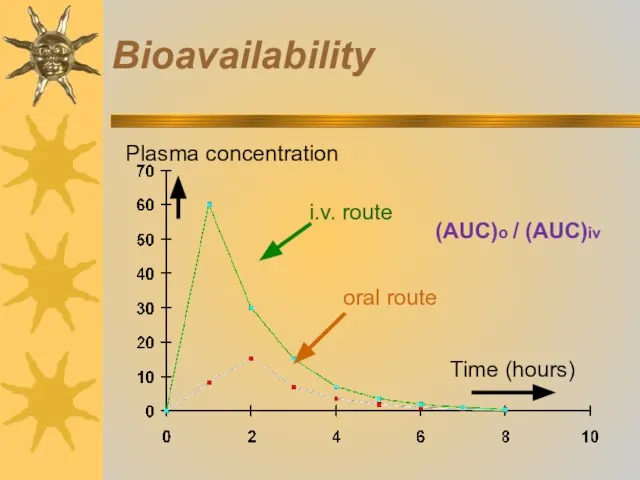
- 19. Bioavailability bioavailability is the proportion of the initial drug dosage that reaches blood plasma (systemic circulation)
- 20. Bioavailability
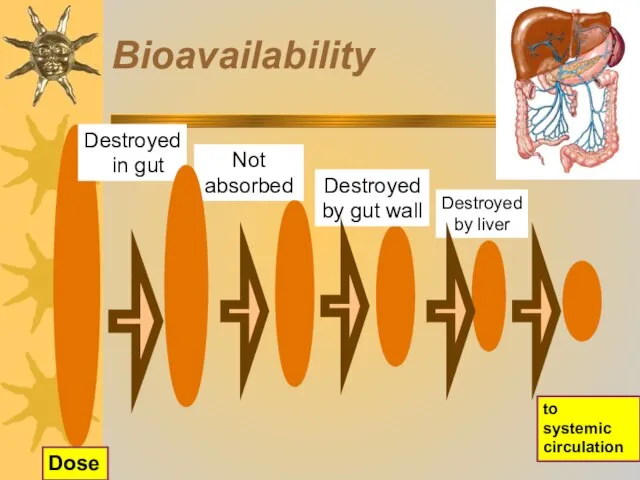
- 21. Bioavailability Not absorbed Destroyed by gut wall to systemic circulation Destroyed by liver Dose Destroyed in
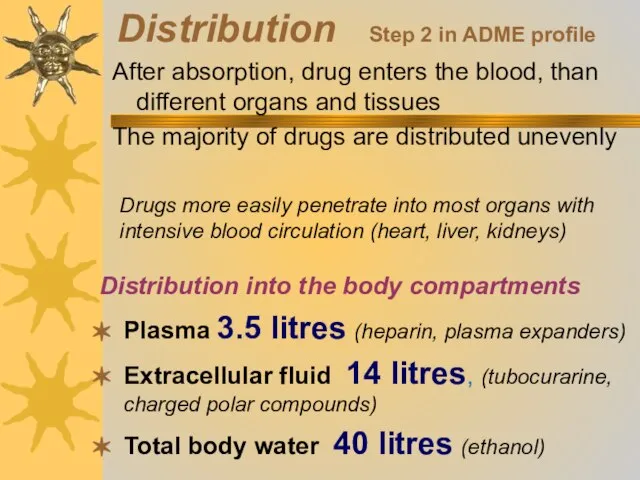
- 22. Distribution Step 2 in ADME profile After absorption, drug enters the blood, than different organs and
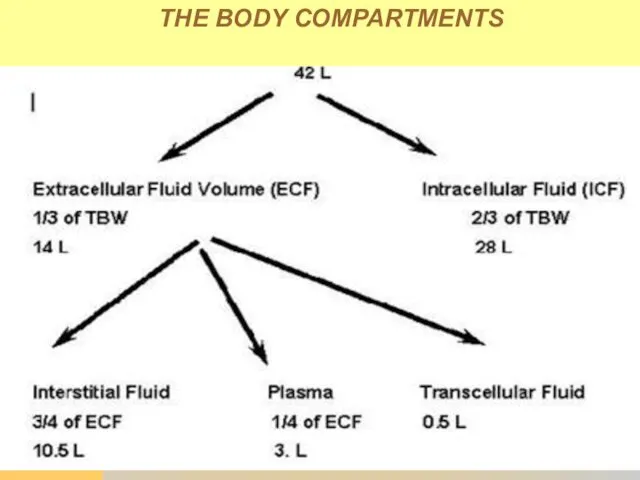
- 23. THE BODY COMPARTMENTS
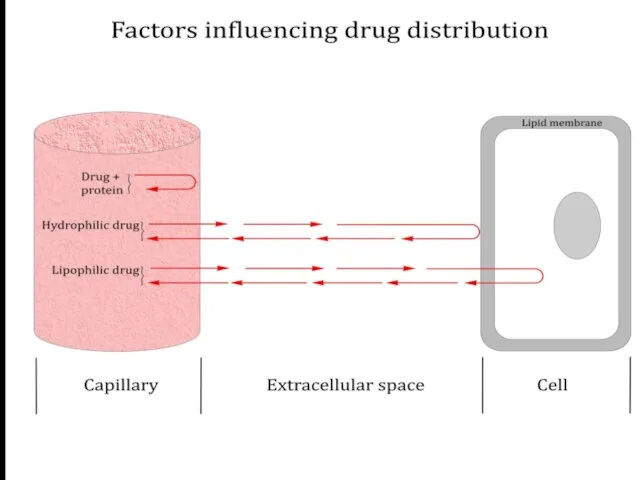
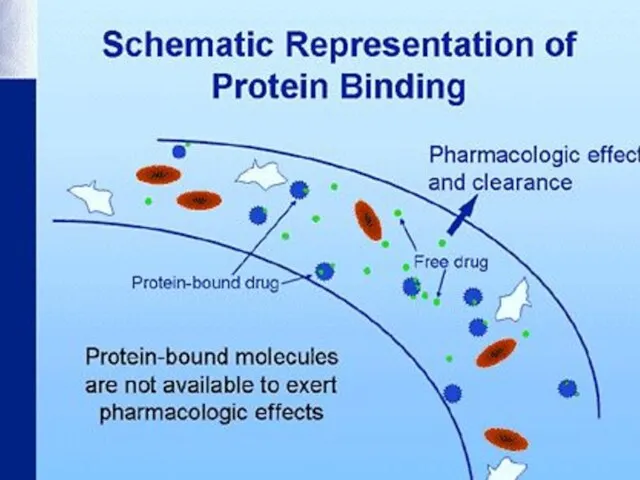
- 25. Distribution of drugs in the body In the body drugs partially bind to other molecules and
- 27. Distribution
- 28. Important for clinical pharmacology It is the presumed volume of liquid in which a drug can
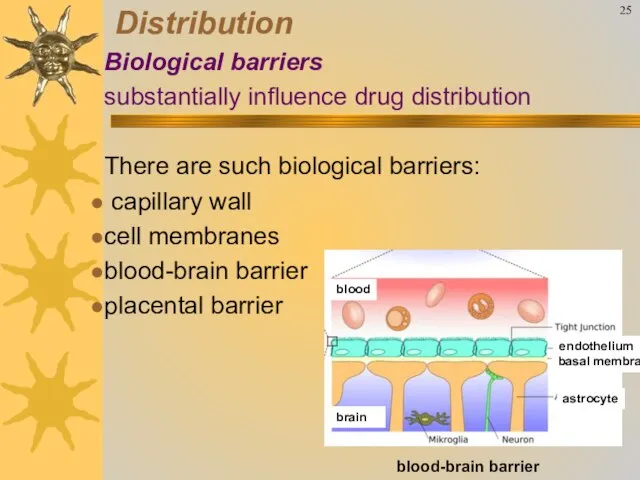
- 29. 25 Distribution Biological barriers substantially influence drug distribution There are such biological barriers: capillary wall cell
- 30. Biotransformation of drugs (drug metabolism) is the process of drugs (xenobiotics) conversion into metabolites that are
- 31. METABOLISM
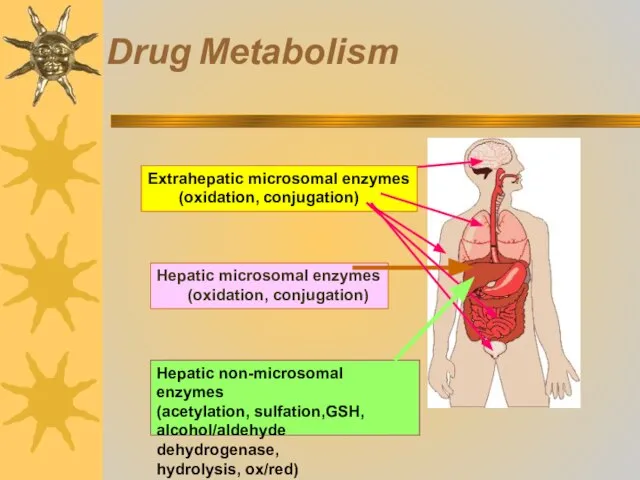
- 32. Drug Metabolism
- 33. 1. Metabolic transformation occurs through oxidation, reduction, hydrolysis In these reactions groups with active hydrogen atoms
- 34. Biotransformation of drugs (drug metabolism) METABOLISM deactivation
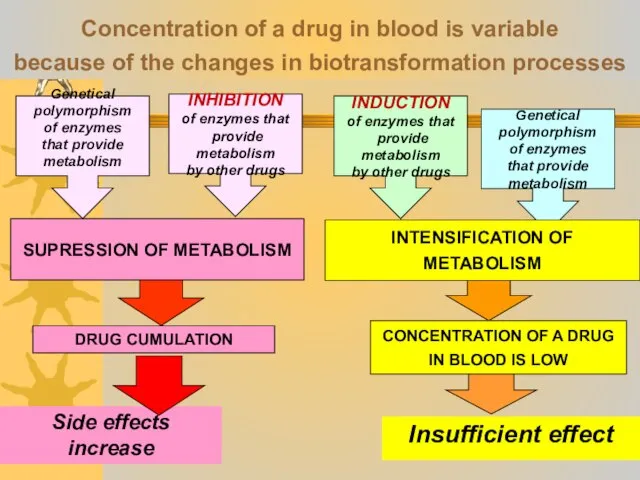
- 35. Metabolic rate depends on genetic factors. Induction and inhibition of metabolism enzymes influences the rate of
- 36. Concentration of a drug in blood is variable because of the changes in biotransformation processes SUPRESSION
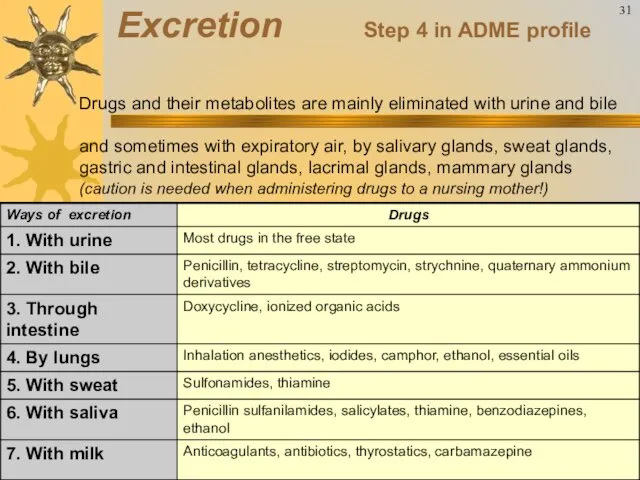
- 37. Drugs and their metabolites are mainly eliminated with urine and bile and sometimes with expiratory air,
- 38. Important for clinical pharmacology It shows the time necessary to decrease drug concentration in blood plasma
- 39. EXCRETION
- 40. Drug interactions Based on the change in drugs pharmacokinetics Based on the change in drugs pharmacodynamics
- 41. Synergism (from Greek syn – together, ergos – work) increase in effect of drugs used at
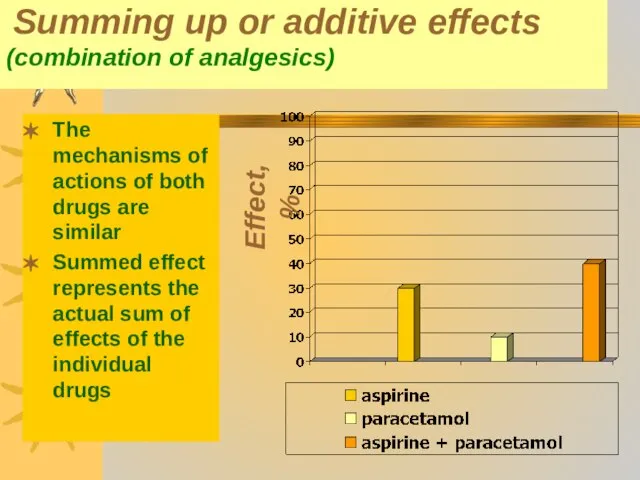
- 42. Summing up or additive effects (combination of analgesics) The mechanisms of actions of both drugs are
- 43. Potentiation (neuroleptanalgesia) The drugs differ in mechanisms of action The total effect exceeds the sum of
- 44. Antagonism (from Greek antagōnisma – struggle, conflict) the ability of drug to decrease the effect of
- 45. Antagonism Types of antagonism - two-way and one-way antagonism A blocker reliably eliminates the effects of
- 46. Drug incompatibility Incompatibility is the weakening, full loss or change in the pharmacotherapeutic effect, intensification of
- 48. Скачать презентацию



























 Веб дизайн и компьютерная графика
Веб дизайн и компьютерная графика Римское право
Римское право Парфенова Татьяна Александровна, учитель биологии школы №97 Санкт-Петербурга
Парфенова Татьяна Александровна, учитель биологии школы №97 Санкт-Петербурга Оқушының сұрағына ынтыландыра жауап беру
Оқушының сұрағына ынтыландыра жауап беру Учитель начальных классов МОУ СОШ №8 Оладько Валентина Николаевна
Учитель начальных классов МОУ СОШ №8 Оладько Валентина Николаевна Финансы и кредит
Финансы и кредит Презентация на тему Гигиена кожи одежды и обуви
Презентация на тему Гигиена кожи одежды и обуви Средства адаптивной физической культуры
Средства адаптивной физической культуры Как выяснить – на кого зарегистрирован антивирус Касперского ?
Как выяснить – на кого зарегистрирован антивирус Касперского ? Робототехника. Открытый урок
Робототехника. Открытый урок Презентация без названия
Презентация без названия Презентация на тему Петропавловск-Камчатский
Презентация на тему Петропавловск-Камчатский Интеграция учебных дисциплин
Интеграция учебных дисциплин Презентация на тему Зачем нужна гигиена (4 класс)
Презентация на тему Зачем нужна гигиена (4 класс) Инструкция по использованию Системы электронного обучения (СЭО) Академия-Медиа
Инструкция по использованию Системы электронного обучения (СЭО) Академия-Медиа Почему люди не летают?
Почему люди не летают? ЭТО МЫ!
ЭТО МЫ! ВКР: Разработка самоочищающейся шпатлевки на основе гипсоцементно-пуццоланового вяжущего с применением диоксида титана
ВКР: Разработка самоочищающейся шпатлевки на основе гипсоцементно-пуццоланового вяжущего с применением диоксида титана Зарубежная Европа. Хозяйство. Промышленность. Сельское хозяйство
Зарубежная Европа. Хозяйство. Промышленность. Сельское хозяйство Презентация на тему Сложные таблицы
Презентация на тему Сложные таблицы  Crisis del Salitre
Crisis del Salitre Система права
Система права СИНОДАЛЬНЫЙ ОТДЕЛ ПО ЦЕРКОВНОЙ БЛАГОТВОРИТЕЛЬНОСТИ И СОЦИАЛЬНОМУ СЛУЖЕНИЮ РПЦ МП НАПРАВЛЕНИЕ ПОМОЩИ БЕЗДОМНЫМ
СИНОДАЛЬНЫЙ ОТДЕЛ ПО ЦЕРКОВНОЙ БЛАГОТВОРИТЕЛЬНОСТИ И СОЦИАЛЬНОМУ СЛУЖЕНИЮ РПЦ МП НАПРАВЛЕНИЕ ПОМОЩИ БЕЗДОМНЫМ Тутанкамон
Тутанкамон От бизнес идеи до собственного бизнеса
От бизнес идеи до собственного бизнеса Презентация на тему Умножение натуральных чисел и его свойства
Презентация на тему Умножение натуральных чисел и его свойства  Бельгия
Бельгия Тема проекта
Тема проекта