Слайд 2Definition
Blood vessels inflammation and damage
Tissue ischemia
Primary vasculitis
Secondary vasculitis
(infections, viruses, tumors, collagen diseases:
RA,

Sjögren’s syndrome, SLE, SSc, Myositis)
Слайд 3VASCULITIS
CLASSIFICATION
LARGE-MEDIUM-SIZED VESSELS
Takayasu’s arteritis
Temporal arteritis
MEDIUM-SMALL-SIZED VESSELS
Polyarteritis nodosa
Kawasaki’s disease
Churg-Strauss syndrome
Wegener’s granulematosis
SMALL-SIZED VESSELS
Schonlein-Henoch syndrome
Cryoglobulinemia
Goodpasture’s
(anti-GBM) disease
Immune complex vasculitis (SLE, Serum sickness)
Microscopic polyangiitis
Слайд 4VASCULITIS
CLASSIFICATION
MISCELLANEOUS SYNDROMES
Behcet’s syndrome
Pyoderma gangrenosum

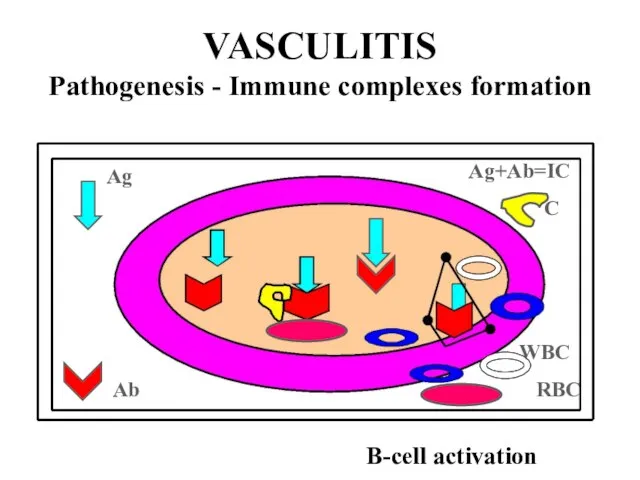
Слайд 5VASCULITIS
Pathogenesis - Immune complexes formation
Ag
Ab
WBC
Ag+Ab=IC
C
B-cell activation
RBC
Слайд 6Vasculitis with IC
Serum sickness
CTD
SLE
PAN
Virus hepatitis B in IC
Cryoglobulinemic vasculitis
Hepatitis C related IC
in cryoprecipitates
Слайд 7Vasculitis with IC
Antigen excess
IC formation
Increased permeability of blood vessels
PLT & MC: histamine,

bradykinin, leukotriens
Activation of complement
C5a – chemotaxis of PMNC
Degranulation of PMNC
Compromised blood flow
Tissue ischemia
Слайд 8Vasculitis with IC depositions
Henoch-Schonlein purpura
CVD
Serum sickness
HCV related mixed cryoglobulinemia
HBV related PAN
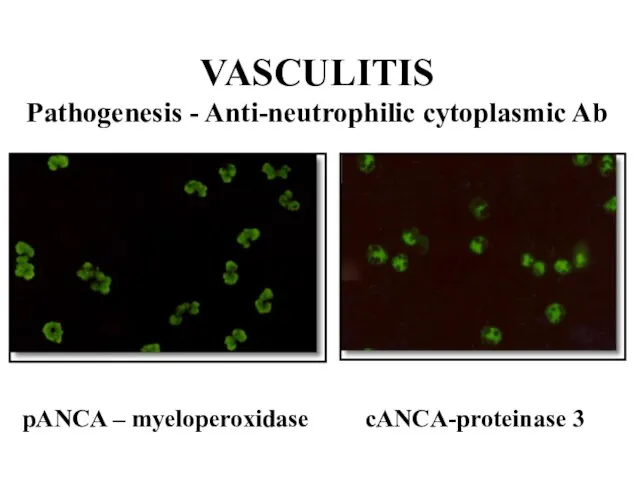
Слайд 9VASCULITIS
Pathogenesis - Anti-neutrophilic cytoplasmic Ab
pANCA – myeloperoxidase cANCA-proteinase 3
Слайд 10ANCA related
Wegener’s granulomatosis
Churg-Strauss syndrome
Microscopic polyangiitis
Necrotizing & crescentic GN
Goodpasture’s syndrome
Crohn’s disease , others

IBD
Слайд 11ANCA associated vasculitis
TNFα, IL-1 induce translocation of azurophilic granules to membrane of

monocytes and PMNC
Myeloperoxidase or proteinase 3 interact with extracellular ANCA
Monocytes and PMNC degranulate and release ROS, IL-1, IL-8
Tissue damage
No correlation between cANCA and WG activity
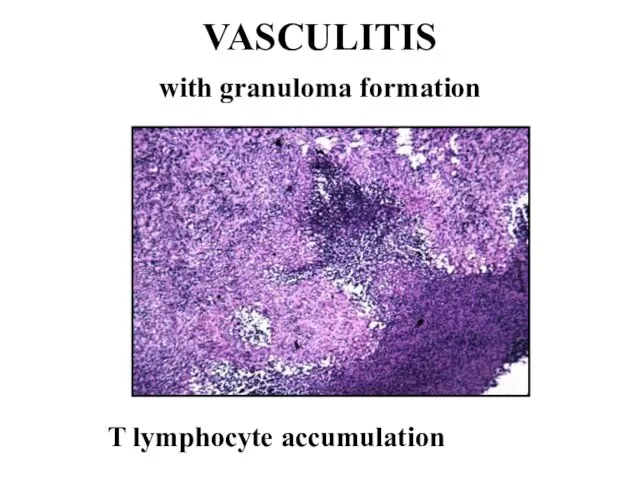
Слайд 12VASCULITIS
with granuloma formation
T lymphocyte accumulation
Слайд 13VASCULITIS
with granuloma formation
Ag or IC induce delayed hypersensitivity and cell mediated
injury
EC activation
INF, IL-1
T-ly activation
TNF
IL-1
Adhesion molecules formation
ELAM-1
VCAM-1
Слайд 14T-ly response and granuloma formation
GCA
Takayasu-s
Wegener’s granulomatosis
Churg-Strauss syndrome

Слайд 15Suspicion of vasculitis
Systemic ilness
Purpura
Pulmonary infiltrates
Microhematuria
Chronic sinusitis
Mononeuritis multiplex
Unexplaned ischemia
GN

Слайд 16DD vasculitis
Infection
Neoplasia
Lymphoma
Coagulopathy
Drugs/toxins
Others

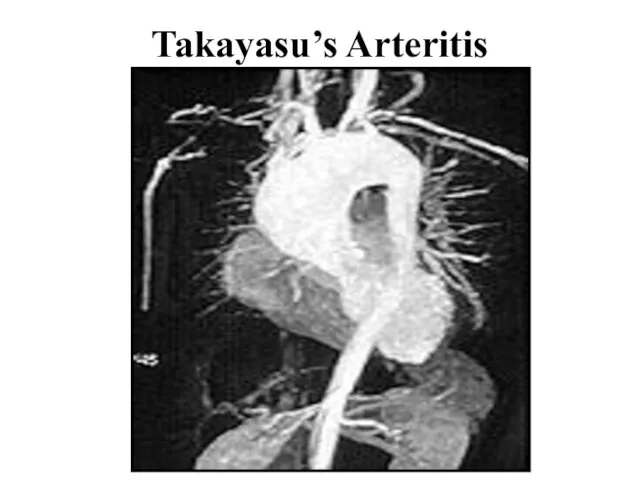
Слайд 17Takayasu’s Arteritis
Pulse-less disease
Incidence: 1-3/1 000 000/year.
Epidemiology: girls+young women
Japan, India, Africa, Asia,

South America, Europe, US.
F:M=7:1. Age 10-50years (90% <30y)
Pathology: Involves aortic arch, descending aorta and its branches + AV involvement, coronary and pulmonary arteries
Panarteritis with granuloma (mononuclears) narrowed vessels and thrombus formation
Слайд 18Takayasu’s Arteritis
General: malaise, fever, night sweats, weight loss, arthralgia/arthritis
Vascular:
Arm claudication/numbness
Pulses

changes/discrepancy
Hypertension
Renal failure
Aortic regurgitation (AR)
Pulmonary hypertension
Laboratory: anemia, ESR/CRP elevation
Diagnosis: angiography, MRI angiography
Treatment: steroids, cytotoxic drugs, control of hypertension, arterial reconstruction, AVR
Prognosis: 15 year survival 90%
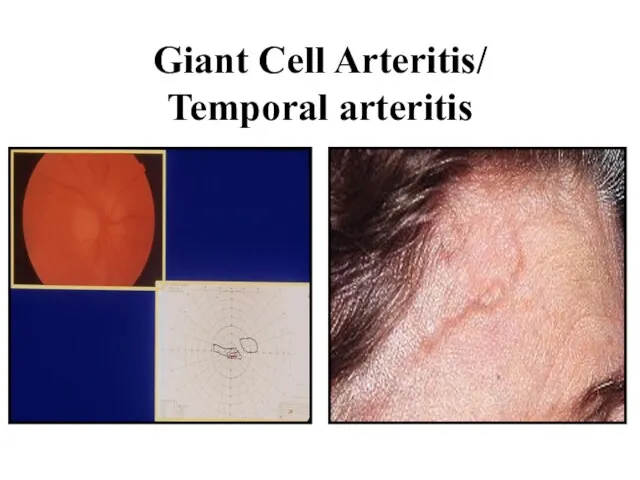
Слайд 20Giant Cell Arteritis/
Temporal arteritis
Слайд 21GCA
Medial and large vessels vasculitis
Branches of carotid artery
Temporal arteries
Strong association with PMR

(50%)
Morning stiffness
Shoulder’s and pelvic pain
Isolated PMR is associated with GCA in 20%
Слайд 22GCA/PMR
Age >50
F>>M
Rare in blacks
6-30/100000
HLA DR4, HLA DRB1
IL-2, INF
CD4+
Panarteritis with mononuclear cells accumulation

and giant cells, intimal proliferation
Ischemia of tissues
Слайд 23GCA
Fever
Headache
General signs
PMR
Scalp tenderness
Jaw claudication
Ischemic optic neuropathy, visual loss
Visceral ischemia, strokes
Aortic aneurisms,

dissection
Anemia
High ESR
Liver enzymes elevation
Слайд 24GCA
Diagnosis
US Doppler
TA biopsy
14 days
Treatment
Cs (40-60 mg/d ~1 months)
Aspirin
MTX
Follow up: ESR

Слайд 25PMR
Diagnosis
Shoulder and hip pain
Stiffness
High ESR
Absence of signs GCA
Treatment
Cs (20mg/d)

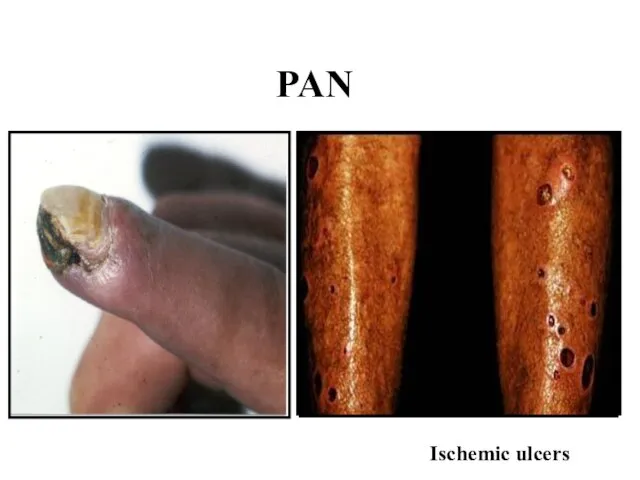
Слайд 26Polyarteritis Nodosa (PAN)
Incidence: 5-9 to 80/1 000 000
Epidemiology: M:F=2-3:1, young patients
Pathology: fibrinoid

necrosis medium/small arteries, aneurysms formation, mononuclear cells and PMNC infiltration, lumen thrombosis, obliteration of the lumen, sparing of pulmonary arteries. Segmental lesions
In kidney – arteritis without GN
Primary or secondary (RA, Sjogren’s syndrome, SLE, Hepatitis B, Hepatitis C, HIV, FMF, hairy cell leukemia)
Слайд 27Polyarteritis Nodosa
Clinical features:
General: severe disease, weight loss, mild to high fever, malaise

Musculo-skeletal (64%): arthralgia, asymmetric polyarthritis, myalgia
Skin (43|%): palpable purpura, ulceration, ischemic necrosis
Neural (50%): peripheral neuropathy, mononeuritis multiplex, CVA
Слайд 28Polyarteritis Nodosa
GIT: abdominal pain, mesenteric thrombosis, peritonitis, bleeding
Kidney (60%): hypertension, renal failure,

proteinuria, hematuria – not glomerulonephritis, hemorrhage from microaneurisms
Cardiac (36%): CHF, MI
Eyes: retinal detachment, scleritis
Genito-urinary (25%): testicular, ovarian pain
Слайд 30PAN
Laboratory data: ESR↑, anemia, globulins↑,
30% HBS Ag+, aHCV+, 20-30% pANCA+
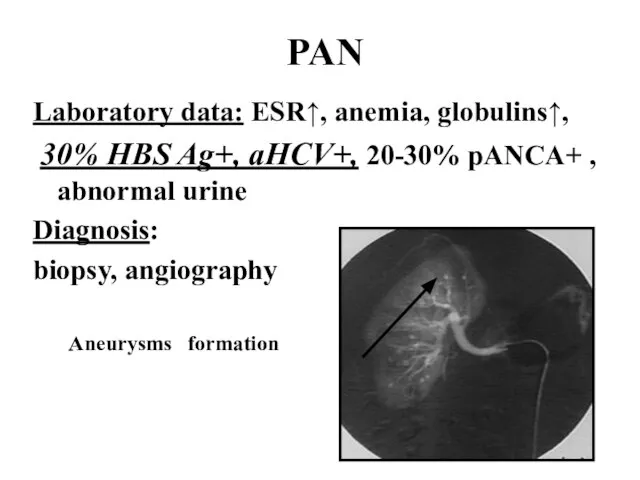
, abnormal urine
Diagnosis:
biopsy, angiography
Aneurysms formation
Слайд 31PAN
Prognosis: 5 year survival 15%-80%
Treatment:
Hepatitis neg: Steroids, Cyclophosphamide, Imuran, Methotrexate
Hepatitis pos:

Antiviral treatment (Interferon, plasmapheresis, Ribaverin), Cs, plasma exchange
Relapse in 10%
Слайд 32Microscopic polyangiitis
Necrotizing vasculitis of small vessels
M>F, >55y
GN (80%)
Pulmonary capillaritis (12%) – hemorrhage
Cardiac

and GIT involvement
Vascular lesions are similar to PAN, but in kidney – typical GN
ESR, anemia, leukocytosis, thrombocytosis, abnormal urine, pANCA pos+++
Diagnosis: kidney biopsy (pauci-immune GN)
Treatment: Cs, CYC
Relapse in 34%
Слайд 33Churg-Strauss Syndrome
Incidence: 1-2/1 000 000
Epidemiology: M:F=2:1
Pathology:
allergic necrotizing angiitis, eosinophils infiltration, extra-vascular

granuloma formation
Small and medium sized vessels
Слайд 34Churg-Strauss Syndrome
Prodromal period: bronchial asthma
Second phase:
eosinophilia
Lóffler s-me - eosinophilic pneumonia

eosinophilic gastroenteritis
Third phase: systemic vasculitis
Слайд 35Churg-Strauss Syndrome
Clinical features:
General signs: fever, malaise, weight loss
Lung involvement: asthma, lung infiltrates,

allergic rhinitis and sinusitis
GIT involvement: abdominal pain, diarrhea, bleeding
NS involvement: mononeuritis multiplex
Heart disease
Kidney involvement: GN
Skin: purpura
Arthritis
Слайд 36Churg-Strauss Syndrome
Peripheral lung infiltrates
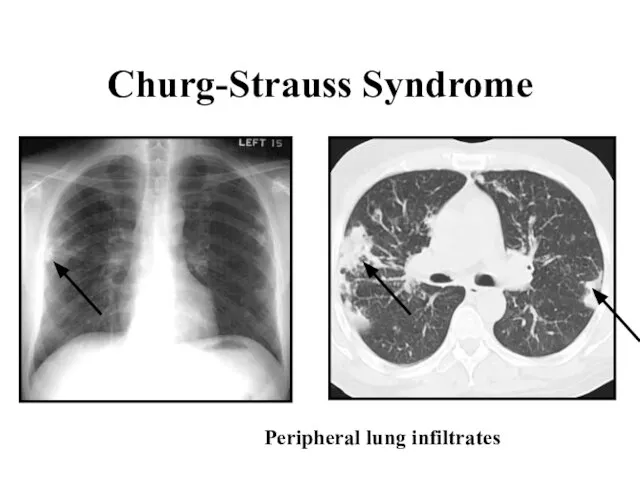
Слайд 37Churg-Strauss Syndrome
Laboratory data: anemia, ESR ↑,
5 000-10 000 eosinophils/mm3, IgE ↑,

pANCA + (70%)
Diagnosis: biopsy
Prognosis: 5 years survival-65%
Treatment: Steroids, Cyclophosphamide, Imuran
Слайд 38Wegener’s Granulomatosis
Incidence: 3/1 000 000
Epidemiology: M:F=1,2:1
Rare in blacks
Age >40 y
Pathology: necrotizing vasculitis

of small arteies and veins, neutrophils accumulation and granuloma: upper airways (sinuses and nasopharyngs), lungs, kidney (pauci-immune GN no granuloma)
INF, TNF, CD4+ (Th1 type)
cANCA
Слайд 39Wegener’s Granulomatosis
General signs: fever, malaise, weight loss
Upper Respiratory Tract (95%): sinusitis, otitis

media, nasal ulceration, septal perforation, subglottic stenosis
Often Staph aureus
Low Respiratory Tract (80%): Pulmonary infiltrates, nodules, cavities (cough, dyspnea, hemopthysis), bronchiectasia
Kidney (75%): Glomerulonephritis, hypertension, renal failure
Слайд 40Wegener’s Granulomatosis
Purpura (45%)→Necrotic ulcers
Arthritis (50-70%)
Eyes (52%): orbital/periorbital mass and damage, scleritis, vasculitis,

NS: peripheral neuropathy, central (33%)
Heart (8%): pericarditis, CHF, MI, arrhythmias
DVT and PE more then in healthy
Слайд 41Wegener’s Granulomatosis
Orbital and nasal granuloma
Pulmonary nodes
And cavitation
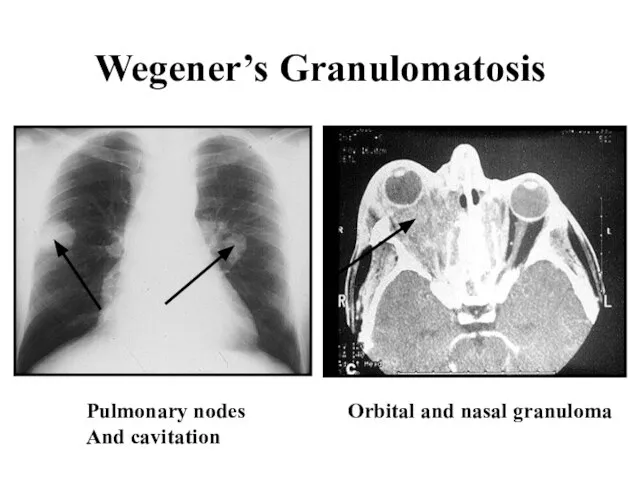
Слайд 42Wegener’s Granulomatosis
Laboratory data: leukocytosis, anemia, ESR↑, cANCA + (90%), abnormal urine, RF+,

thrombocytosis
Diagnosis: nasal biopsy (granuloma), open lung biopsy (granuloma and vasculitis)
Renal biopsy is not specific
Слайд 43Wegener’s Granulomatosis
Prognosis: 5 years survival - 50-75%
Progressive renal failure
Late organ damage
Co-morbidities
Cancer (bladder)
Follow

up: clinically, ANCA???
Treatment: CYC (oral/IV) and Cs, Imuran, MTX, MMF, Trimethoprim Sulfamethoxazole (Resprim)
Biological (RTX+, ETN-)
Слайд 44Henoch-Schőnlein Purpura
Incidence: 4-10/100 000
Epidemiology: M:F=1,2:1, age 4-14 years
Pathogenesis: IC vasculitis (Drugs? Infections?)
Pathology:

small vessels necrotizing leukocytoclastic vasculitis, fibrinoid necrosis, IC, IgA and C3 deposition (skin, gut, kidney [glomerrular& tubular]), MNC infiltration
Слайд 45Henoch-Schőnlein Purpura
Clinical features:
General signs
Skin: palpable purpura (100%), ulceration (rare)
Arthritis, arthralgia (60%)
GIT vasculitis

(85%) abd. pain, diarrhea, bleeding
Renal (IgA nephropathy) disease (10-40%) – segmental proliferative GN +/- crescents, IgA + C³ deposition (Berger’s disease) – hematuria, proteinuria
Слайд 46Henoch-Schőnlein Purpura
Purpura, Arthritis
Ischemic colitis
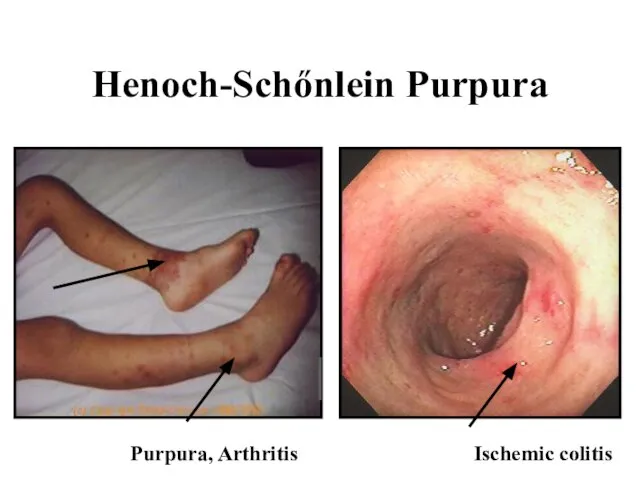
Слайд 47Henoch-Schőnlein Purpura
Laboratory data: elevated ESR/CRP, leukocytosis, mild anemia, hematuria, high IgA
Diagnosis: clinical

+/- biopsy
Prognosis: good (except severe GIT vasculitis and IgA nephropathy)
Treatment: rest, tratement of underlying disease, NSAID, Cs, CYC – only in severe internal organ involvement
Слайд 48Essential Mixed Cryoglobulinemia
Cryo – cold-precipitable Ig (mono/polyclonal)
Systemic signs
Primary - rare
Secondary in most

cases
Слайд 49Cryoglobulinemic Vasculitis
Biopsy:
Skin: Inflammatory infiltrate involving small blood vessels, fibrinoid necrosis, EC
hyperplasia, hemorrhage, Ig and IC deposition
Kidney: Membranous GN
Hepatitis C specific Ig, monoclonal IgM RF++
ESR++, anemia, CRF, low C3/C4, HCV RNA+++, high IgM
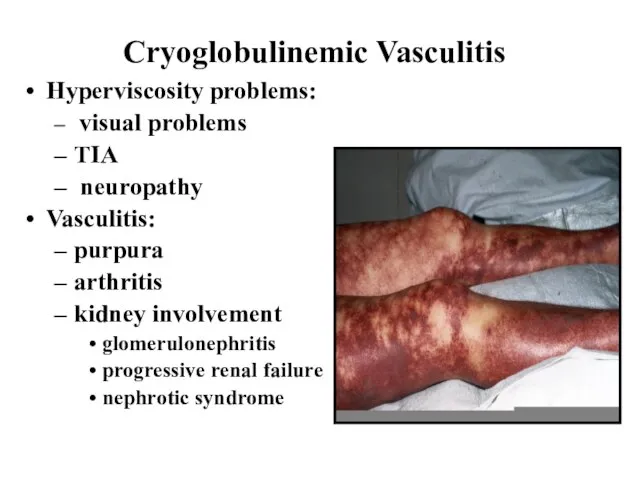
Слайд 50Cryoglobulinemic Vasculitis
Hyperviscosity problems:
visual problems
TIA
neuropathy
Vasculitis:
purpura
arthritis
kidney involvement
glomerulonephritis
progressive renal
failure
nephrotic syndrome
Слайд 51Cryoglobulinemic Vasculitis
Prognosis: poor, depends on viremia
Treatment:
plasmapheresis,
antiviral therapy (Ribaverin + Interferon

α)
Cs = CYC
Слайд 52Behcet’s Disease
Epidemiology: Japan, Meddle East (Silk rood)
Family penetration
Clinical feature:
Oral aphthous ulcers (100%)

– 3/year
Genital ulcerations (80%)
Eye inflammation (65%)-anterior/posterior uveitis, retinal vasculitis
Skin inflammation (70%)-(folliculitis-like, acne-like, erythema nodosum-like)
Vasculitis (arterial-CNS, venous – thrombosis superficial and deep)
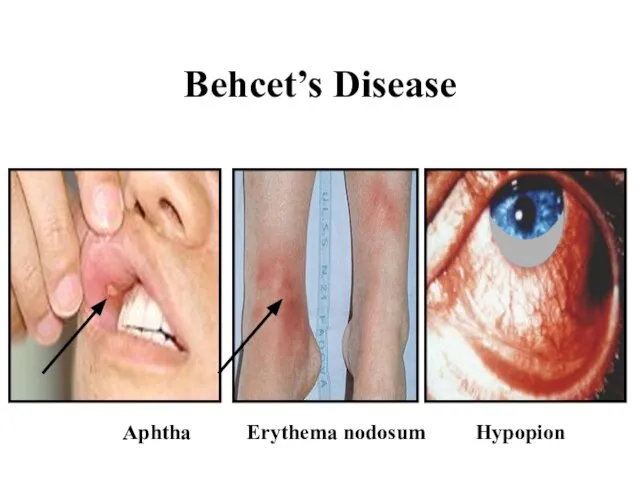
Слайд 53Behcet’s Disease
Aphtha
Erythema nodosum
Hypopion
Слайд 54Behcet’s Disease
Laboratory data: HLA B51 pos.
Pathergy skin test
Prognosis: serious in uveitis

- blindness, CNS vasculitis, thrombosis
Treatment: Colchicine
CS +/- MTX, Imuran, Salazopyrine
CS +Neoral
Thalidomide
Anticoagulants



















































 Инфраструктурные инвестиции
Инфраструктурные инвестиции Културен туризъм: международен маркетинг Бележки към кръглата маса организирана от ПП ГЕРБ Асеновград, 23.06.09
Културен туризъм: международен маркетинг Бележки към кръглата маса организирана от ПП ГЕРБ Асеновград, 23.06.09 Pos материалы гербион
Pos материалы гербион Презентация на тему Неофициальные символы России
Презентация на тему Неофициальные символы России CPA launches FOD
CPA launches FOD Методы и приборы разрушающего контроля, применяемые при обследовании
Методы и приборы разрушающего контроля, применяемые при обследовании ЖИЗНЬ И БЫТ В СРЕДНЕВЕКОВОМ ЗАМКЕ
ЖИЗНЬ И БЫТ В СРЕДНЕВЕКОВОМ ЗАМКЕ Презентация компании MOST Marketing«Франчайзинговый пакет: как разработать,чтобы привлечь франчайзи»
Презентация компании MOST Marketing«Франчайзинговый пакет: как разработать,чтобы привлечь франчайзи» Колористика при окрашивании волос. Тест
Колористика при окрашивании волос. Тест Предложение по летнему корпоративному отдыху на стадионе «Труд» (пос. «Старая Купавна»)
Предложение по летнему корпоративному отдыху на стадионе «Труд» (пос. «Старая Купавна») Греческая вазопись
Греческая вазопись Холод в нефтянной промышленности
Холод в нефтянной промышленности Урок-путешествие по разделу «Были-небылицы». Оценка достижений
Урок-путешествие по разделу «Были-небылицы». Оценка достижений LobbyWorks
LobbyWorks Самоиндукция
Самоиндукция Correct сommunication. Правильное общение
Correct сommunication. Правильное общение Тема: «Положение человека в системе животного мира. Эволюция гоминид».
Тема: «Положение человека в системе животного мира. Эволюция гоминид». Презентация на тему Выживание в природных условиях после аварии
Презентация на тему Выживание в природных условиях после аварии  ангелы
ангелы Интеллектуально-познавательная игра
Интеллектуально-познавательная игра Анализ применимости ПИК «СтОФ» для массовой оценки стоимости движимого имущества Тевелева Оксана Валерьевна тел: (499) 724-15-14, 8(903)208-
Анализ применимости ПИК «СтОФ» для массовой оценки стоимости движимого имущества Тевелева Оксана Валерьевна тел: (499) 724-15-14, 8(903)208- Fruit and vegetables
Fruit and vegetables Ты подвиг совершил во имя жизни на земле
Ты подвиг совершил во имя жизни на земле Обязательства из односторонних сделок и из действий в чужом интересе. Обязательства из договоров, не подлежащие судебной защите
Обязательства из односторонних сделок и из действий в чужом интересе. Обязательства из договоров, не подлежащие судебной защите ТВ - тюнеры
ТВ - тюнеры Применение программного комплекса CorPos (FORCE Technology Norway AS) для диагностики и прогнозирования коррозии на внутренних стенках газопров
Применение программного комплекса CorPos (FORCE Technology Norway AS) для диагностики и прогнозирования коррозии на внутренних стенках газопров Евгений Замятин
Евгений Замятин Characteristic of grain mass
Characteristic of grain mass