Содержание
- 2. Crohn’s Disease Aim of this module To increase the understanding of Crohn’s disease by looking at
- 3. How to use this module This module is designed by a student for students. The data
- 4. Epidemiology & Pathology of Crohn’s Disease
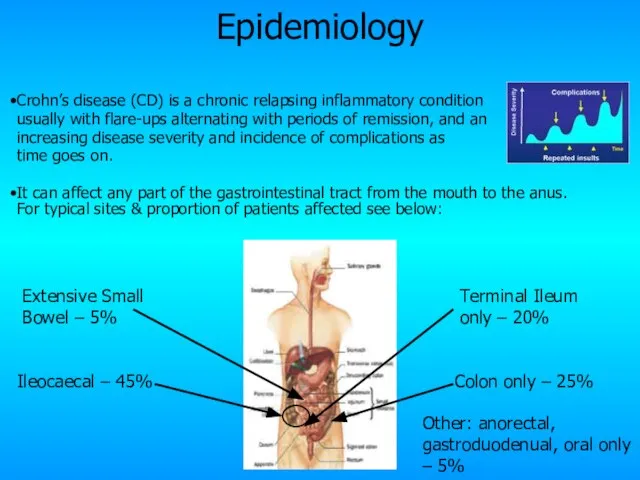
- 5. Crohn’s disease (CD) is a chronic relapsing inflammatory condition usually with flare-ups alternating with periods of
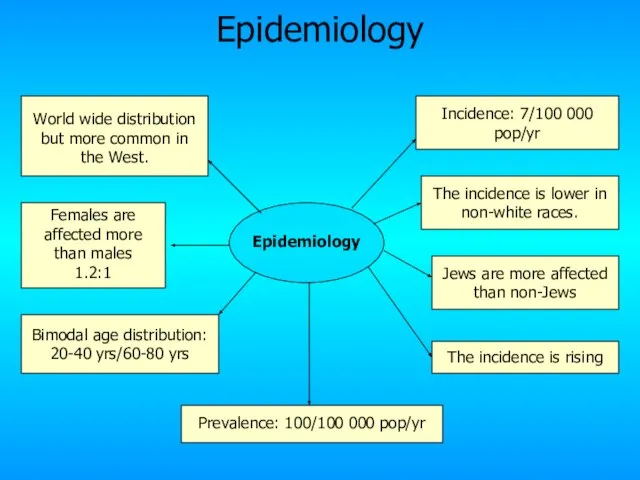
- 6. Epidemiology Incidence: 7/100 000 pop/yr Prevalence: 100/100 000 pop/yr World wide distribution but more common in
- 7. Pathology It is characterised by patchy transmural inflammation. The chronic inflammatory process leads of thickening of
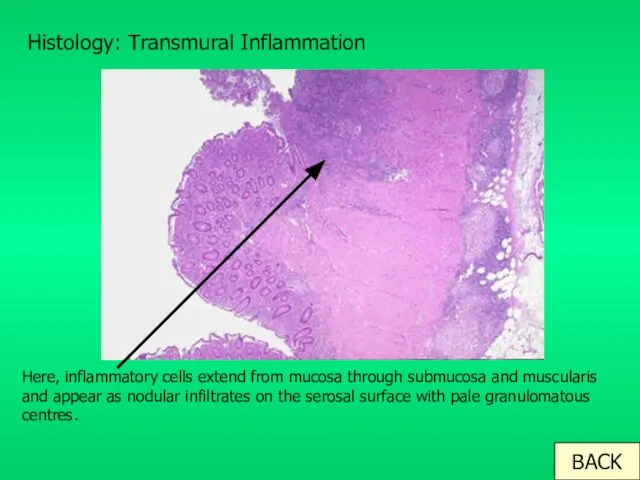
- 8. Histology: Transmural Inflammation Here, inflammatory cells extend from mucosa through submucosa and muscularis and appear as
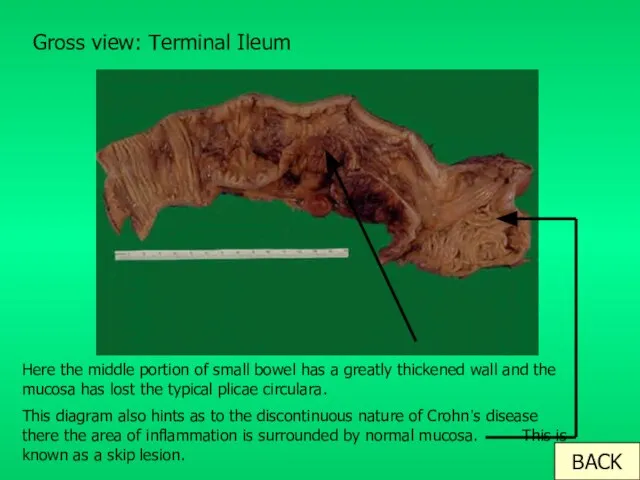
- 9. Gross view: Terminal Ileum Here the middle portion of small bowel has a greatly thickened wall
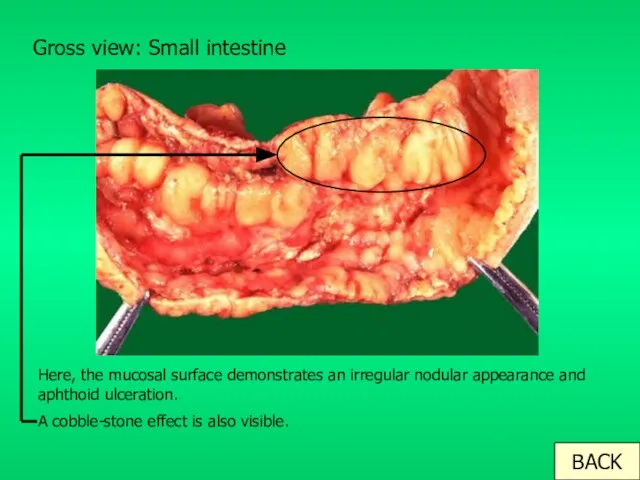
- 10. Gross view: Small intestine Here, the mucosal surface demonstrates an irregular nodular appearance and aphthoid ulceration.
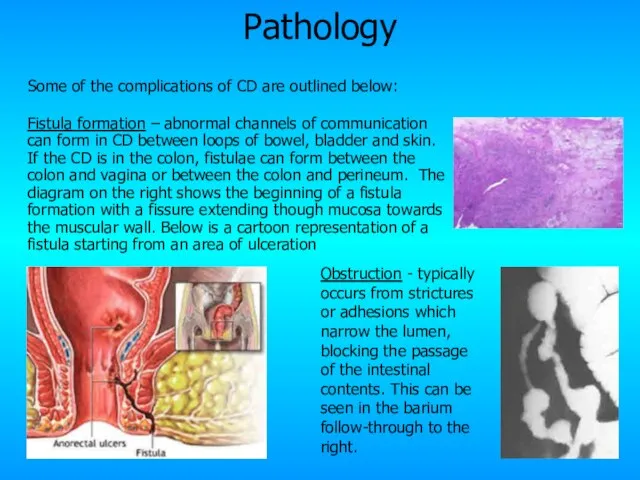
- 11. Pathology Some of the complications of CD are outlined below: Fistula formation – abnormal channels of
- 12. Aetiology and Pathogenesis of Crohn’s Disease
- 13. Aetiology & Pathogenesis The aetiology of Crohn’s disease is unknown. There are many proposed pathogenic mechanisms,
- 14. Genetic Factors There are 3 mutations on the CARD15 gene on Chromosome 16 that are associated
- 15. Environmental Factors A wide range of environmental factors have been found to play a role: Smoking
- 16. Immune response Host Immune Response Both the potential genetics underlying CD and the environmental and host
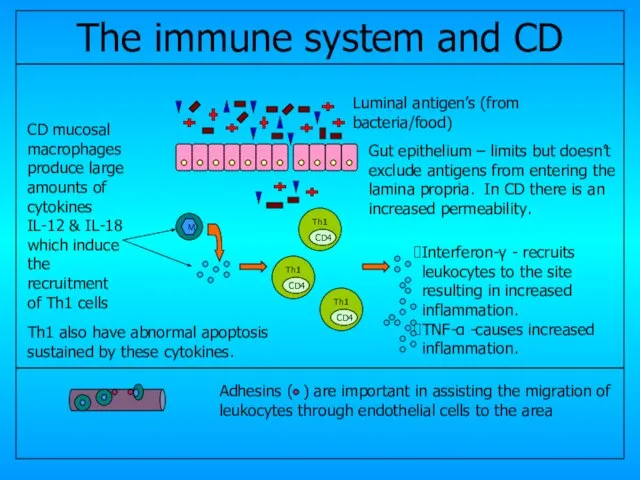
- 17. CD4 CD4 CD4 Gut epithelium – limits but doesn’t exclude antigens from entering the lamina propria.
- 18. Clinical features of Crohn’s Disease
- 19. Clinical Features The clinical presentation can be very variable depending upon the site and predominant pathology
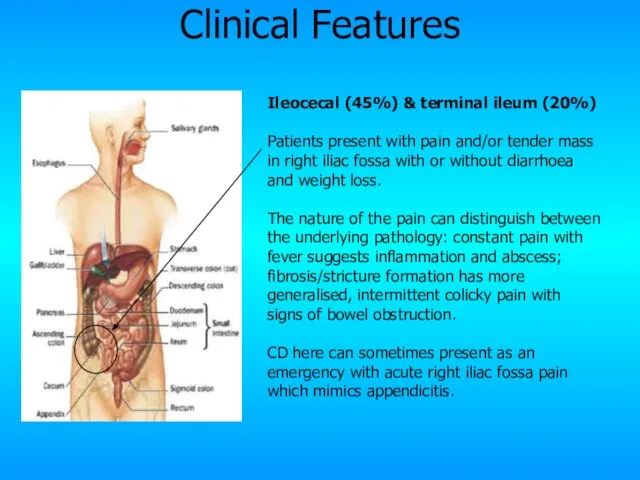
- 20. Ileocecal (45%) & terminal ileum (20%) Patients present with pain and/or tender mass in right iliac
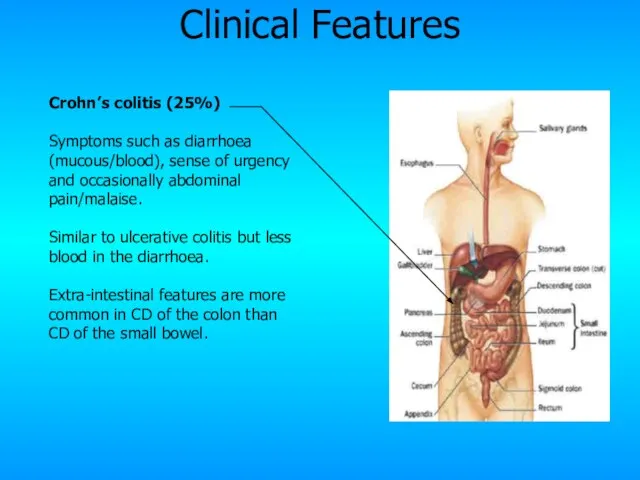
- 21. Crohn’s colitis (25%) Symptoms such as diarrhoea (mucous/blood), sense of urgency and occasionally abdominal pain/malaise. Similar
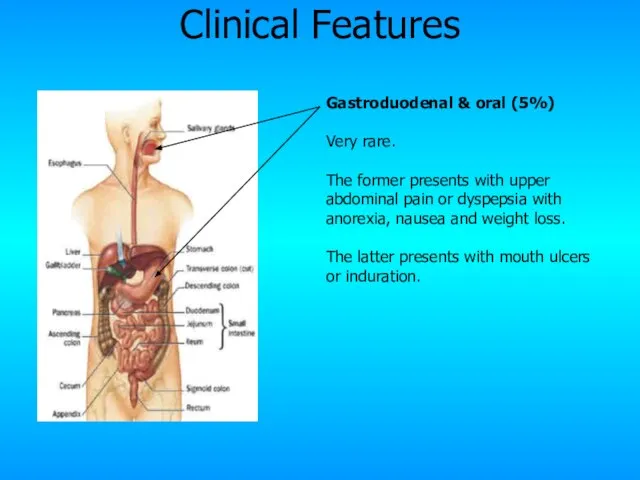
- 22. Gastroduodenal & oral (5%) Very rare. The former presents with upper abdominal pain or dyspepsia with
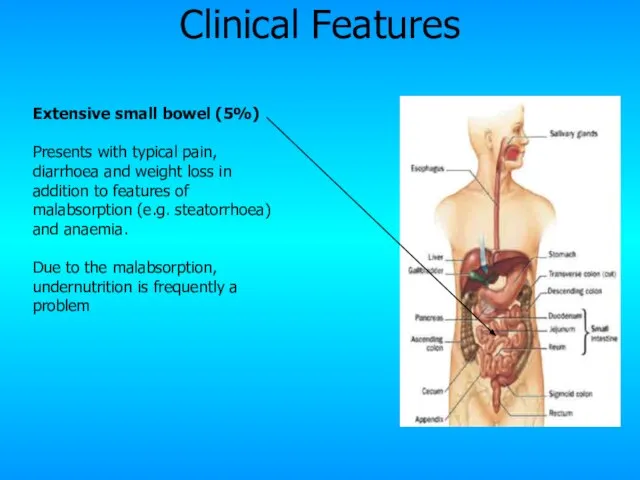
- 23. Extensive small bowel (5%) Presents with typical pain, diarrhoea and weight loss in addition to features
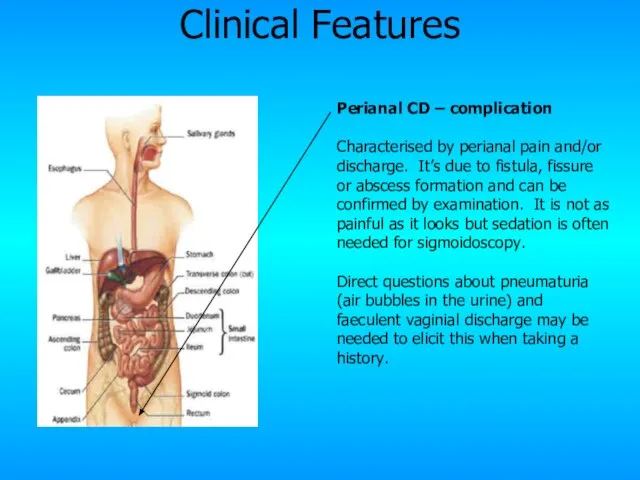
- 24. Perianal CD – complication Characterised by perianal pain and/or discharge. It’s due to fistula, fissure or
- 25. Intestinal Complications Anal and perianal complications Fissure in ano or fistula in ano Haemorrhoids Skin tags
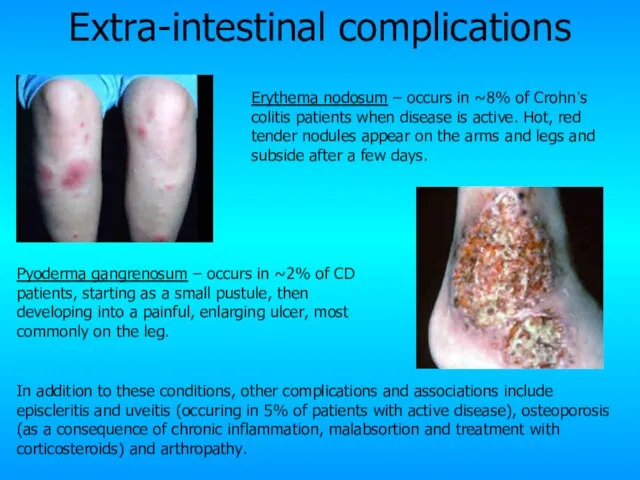
- 26. Extra-intestinal complications Sclerosing Cholangitis – occurs in a small proportion of patients. The pathogenesis is unknown
- 27. Extra-intestinal complications Pyoderma gangrenosum – occurs in ~2% of CD patients, starting as a small pustule,
- 28. Diagnosis and Management of Crohn’s Disease
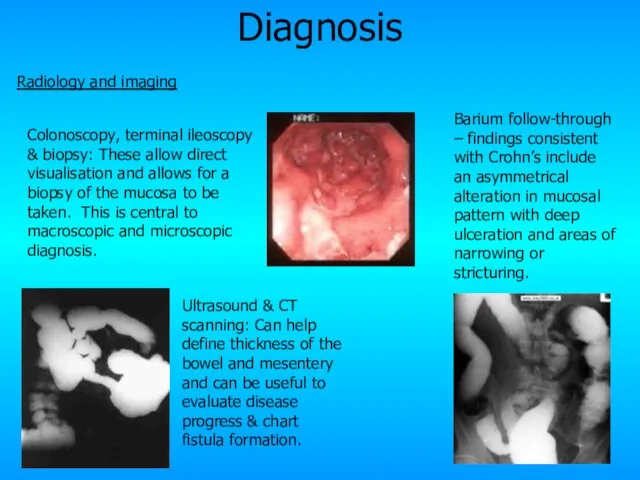
- 29. Diagnosis Radiology and imaging Ultrasound & CT scanning: Can help define thickness of the bowel and
- 30. Diagnosis Blood tests Haematology: results suggesting anaemia, ? platelet count & ? ESR suggests an inflammatory
- 31. Differential Diagnosis There are many differential diagnosis for Crohn’s disease, complicated further by the differing presentations
- 32. Management Management is best if a MDT approach is adopted, including physicians, surgeons, specialist nurses, dieticians
- 33. Medical management Dietary advice and nutritional support including vitamin supplementation to counter-act any deficiencies that develop.
- 34. Drug Information BACK Class Aminosalicylates Corticosteroids Infliximab Methotrexate Name Balsalazide, mesalazine, olsalazine, sulfasalazine Prednisolone Infliximab Methotrexate
- 35. Surgical management Surgery is indicated for perforation or haemorrhage (emergency) or for small-bowel obstruction, Crohn's colitis,
- 36. Prognosis Mortality The cumulative mortality is approximately twice that of the general population. Death is primarily
- 37. Summary Crohn’s disease is a chronic inflammatory condition of the gastrointestinal tract characterised by transmural inflammation,
- 38. The different sections If you want to revisit any of the sections of this module please
- 39. Case Study 30-year-old woman was admitted with a 4-week history of increasing bloody diarrhoea and abdominal
- 40. Case Study The rectal biopsy taken at sigmoidoscopy showed a small area of ulceration of the
- 41. Thank you I hope this has been of some help to your studies!
- 43. Скачать презентацию


























 Государственный и муниципальный кредит
Государственный и муниципальный кредит Подготовка к ГИА. Знаки препинания в сложносочиненном и сложноподчиненном предложении
Подготовка к ГИА. Знаки препинания в сложносочиненном и сложноподчиненном предложении Что такое постдемократия
Что такое постдемократия Возникновение искусства тату и профессии татуировщика
Возникновение искусства тату и профессии татуировщика Рабочая инструкция сборки формы “Вилка стойки” 12300-2905515-01 KURTZ
Рабочая инструкция сборки формы “Вилка стойки” 12300-2905515-01 KURTZ Стратегическая модель Ж. -М. Дрю
Стратегическая модель Ж. -М. Дрю  Презентация на тему Измерение физических величин
Презентация на тему Измерение физических величин Чьи глаза?
Чьи глаза? «Шведский стол»
«Шведский стол» Иосиф Дик «Красные яблоки»
Иосиф Дик «Красные яблоки» Презентация на тему ПРОСТЕЙШИЕ
Презентация на тему ПРОСТЕЙШИЕ  Этикет 4 класс
Этикет 4 класс Произведения народного искусства
Произведения народного искусства Сравнительный анализ доходности индексных ПИФов и ПИФов акций
Сравнительный анализ доходности индексных ПИФов и ПИФов акций Presentation Title
Presentation Title  Die Geschichte des Fußballs
Die Geschichte des Fußballs Как мы общаемся с миром
Как мы общаемся с миром My favorite company
My favorite company Презентация
Презентация День правовой помощи детям
День правовой помощи детям Принятие решений в условиях существования рисков с низкими вероятностями реализации
Принятие решений в условиях существования рисков с низкими вероятностями реализации Письмо
Письмо Тактильная чувствительность
Тактильная чувствительность Инвестиция, как важнейшее условие для реализации проекта
Инвестиция, как важнейшее условие для реализации проекта Конструирование брюк
Конструирование брюк ПРОГРАМНЕ ЗАБЕЗПЕЧЕННЯ СПЕЦІАЛЬНИХ ІНФОРМАЦІЙНО-ТЕЛЕКОМУНІКАЦІЙНИХ СИСТЕМ
ПРОГРАМНЕ ЗАБЕЗПЕЧЕННЯ СПЕЦІАЛЬНИХ ІНФОРМАЦІЙНО-ТЕЛЕКОМУНІКАЦІЙНИХ СИСТЕМ Особенности продвижения транспортных услуг
Особенности продвижения транспортных услуг Священнослужители в рядах Русской армии
Священнослужители в рядах Русской армии