Содержание
- 2. Dyspepsia syndrome is determined as pain or discomfort localized in the epigastric area closer to the
- 3. Patients' complaints on admission corresponding to the complex of symptoms in gastric dyspepsia: pains in the
- 4. A complex of symptoms in dyspepsia syndrome is to be distinguished from the one in gastroesophageal
- 5. Depending on the causes triggering dyspeptic disorders, there is organic and functional (non-ulcerative) dyspepsia.
- 6. Organic dyspepsia is recognized if the following markers are highlighted: esophageal disease: reflux- esophagitis gastric disease:
- 7. If to exclude the diseases mentioned after a through examination, the patients (in case the dyspeptic
- 8. Classification of functional dyspepsia. According to A. Smout et al. (1992) - according to intestinal motility:
- 9. According to N. Talley (1991), M. von Oytryve et al. (1993) - ulcerative-like variant; - refluxoid
- 10. In 20-69% of patients with ulcerative-like variant the duodeno-gastric reflux, delayed evacuation from the stomach, and
- 11. Clinical variation of non-ulcerative dyspepsia. Depending on the either symptoms predominated in the clinical presentation of
- 12. Clinical characteristics of various non-ulcerative dyspepsias Ulcerative-like type Pains localized in the epigastric area Pains subside
- 13. Dyskinetic type Early saturation Feeling of repletion in the epigastria area after the meals Nausea Upper
- 14. If the symptoms presented in patients do not correspond with the underlined variants, then the symptoms
- 15. Etiology and pathogenesis Chronic gastritis usually associated with pyloric helicobacterium (H. pylori), used to be recognized
- 16. Chronic gastritis associated with H. pylori is frequently revealed in patients with non-ulcerative dyspepsia syndrome. H.
- 17. The recent findings have also exposed the lack in distinction concerning the hydrochloric acid secretion in
- 18. Gastric and duodenal motility disorder proved to be the chief pathogenetic factors of non-ulcerative dyspepsia syndrome.
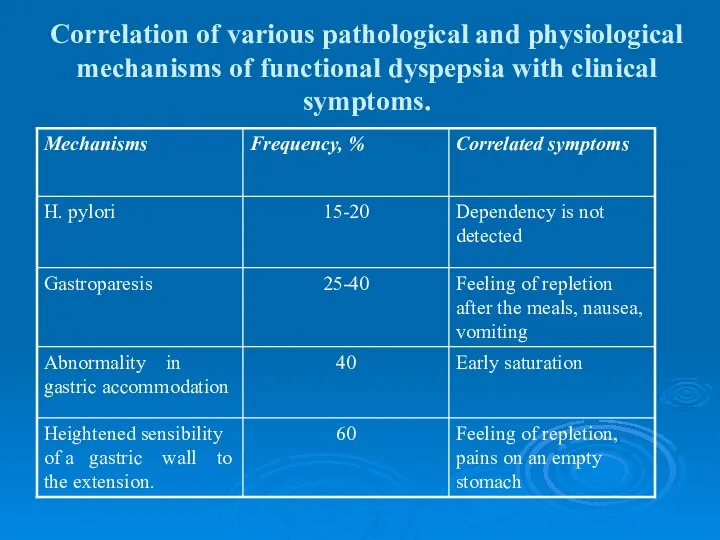
- 19. Correlation of various pathological and physiological mechanisms of functional dyspepsia with clinical symptoms.
- 20. Gastric accommodation disorder (accommodation is determined here as capability of the fundic part of the stomach
- 21. Gastric accommodation disorder (accommodation is determined here as capability of the fundic part of the stomach
- 22. If stomach evacuates the food well, the cause for the dyspeptic complaints is a heightened sensibility
- 23. Diagnosis and differential diagnosis. A complex of symptoms in non-ulcerative dyspepsia is of no specific ground,
- 24. It is essential to take into account secondary motility derangement of the upper parts of the
- 25. The syndrome of gastric dyspepsia in ulcerative disease characterizes with response on food, seasonal character of
- 26. stomach ulcer The diagnostical method of stomach ulcer is an X-ray examination. But in some cases,
- 27. Stomach cancer Stomach cancer is manifested by gastric dyspepsia, which characterizes with persistence and progression. The
- 28. chronic cholecystitis Dyspeptic complaints have a more frequent occurrence during the chronic cholecystitis development. Vomiting is
- 29. During the period of exacerbation, patients complain of nausea, bitter taste, eructation with bitter. Due to
- 30. pancreatic dyspepsia is expressed in exacerbation or severe course of the disease. It is manifested by:
- 31. Gastric dyspepsia in chronic gastritis is characterized with the dependency on diet violence. It is presented
- 32. As the disease progresses, patients with chronic gastritis have tendency to hyposecretion and reduction in acidity
- 33. Antral gastritis, gastroduodenitis may resemble ulcerative disease of the duodenum in their clinical manifestations. The disease
- 34. Gastroesophageal reflux disease is a chronic recurrence conditioned by retrograde entrance of food mass into esophagus.
- 35. Pains in the epigastrium associated or not with the food taken may occur quite often. Vomiting
- 36. Methods of differential diagnosis applied in functional dyspepsia. Esophagogastroduodenoscopy X-ray examination Ultrasonography Intragastric and intraesophageal monitoring
- 37. Clinical and biomedical blood tests, as well as ultrasound investigations of the abdomen, gastroduodenoscopy and X-ray
- 38. It is supposed to be important to take alarm symptoms or «red flags» into account while
- 39. Alarm symptoms are characterized as follows: fever anemia dysphagy leukocytosis visible admixture accelerated ESR blood in
- 40. Treatment. The treatment procedures are to be complex and include not only drug administration, but also
- 41. Antacidic and antisecretory drugs (H2-blockers and blockers of proton pump) are indicated in ulcerative-like variant of
- 42. Some patients (about 20-25%) may express positive response to anti-helicobacterial eradication therapy. The treatment may have
- 43. Eradication therapy T. Omeprasoli 20 mg 2 t. a day T. Clarithromycini 500 mg 2 t.
- 44. The basic means of patients' treatment of a developing dyskinetic variant is supposed to be prokinetic
- 45. The use of metodopramide (especially long-term one) may cause untoward and side effects in a great
- 46. European Motilium investigations in non-ulcerative dyspepsia treatment at doses of 5-20 mg 3-4 times a day
- 47. Итомед (Itomed) итоприда гидрохлорид 50 мг 3 раза в день side effects: -лейкопения, тромбоцитопения, гинекомастия, гиперпролактинемия;
- 48. Cyzapride (propulside, coordinacs) attracts much attention. This drug is quite effective in functional dyspepsia (in 60-90%>
- 50. Скачать презентацию















































 Предложения пациентского сообщества по развитию системы ВМП
Предложения пациентского сообщества по развитию системы ВМП Галактоземия
Галактоземия Zinc for the prevention or treatment of acute viral respiratory tract infections in adults: a rapid systematic review
Zinc for the prevention or treatment of acute viral respiratory tract infections in adults: a rapid systematic review Инфекционные заболевания
Инфекционные заболевания Особенности обследования больных с гнойными заболеваниями
Особенности обследования больных с гнойными заболеваниями Нарушение умственной работоспособности
Нарушение умственной работоспособности Аутизм, РАС – биокоррекция с помощью диеты и продуктов Тенториум
Аутизм, РАС – биокоррекция с помощью диеты и продуктов Тенториум Программа повышения квалификации Нейропсихология детского возраста
Программа повышения квалификации Нейропсихология детского возраста Топ-5 цветов по мнению дальтоников
Топ-5 цветов по мнению дальтоников Почечный тубулярный ацидоз
Почечный тубулярный ацидоз Соблюдение гигиенических норм и правила ношение масок
Соблюдение гигиенических норм и правила ношение масок Личная гигиена. Гигиена кожи, одежды
Личная гигиена. Гигиена кожи, одежды Замена митрального клапана. Реконструктивные операции на митральном клапане
Замена митрального клапана. Реконструктивные операции на митральном клапане Вирус гепатита С. История
Вирус гепатита С. История Московский Государственный Медико-Стоматологический Университет
Московский Государственный Медико-Стоматологический Университет Medical law
Medical law постинъекционные осложнения
постинъекционные осложнения Полезная и вредная еда
Полезная и вредная еда Формирование территориальных фондов медицинского страхования на примере ТФОМС Челябинской области
Формирование территориальных фондов медицинского страхования на примере ТФОМС Челябинской области Синдром полости в легком
Синдром полости в легком ДЦП. Спастическая диплегия
ДЦП. Спастическая диплегия Оказание качественной эффективной медицинской помощи путем достижения медицинской работниками доверия пациента
Оказание качественной эффективной медицинской помощи путем достижения медицинской работниками доверия пациента Жарақаттар. Жарақат деген не?
Жарақаттар. Жарақат деген не? линические и эпидемиологические аспекты очагового распространения сифилиса среди детей и подростков в Смоленском регионе
линические и эпидемиологические аспекты очагового распространения сифилиса среди детей и подростков в Смоленском регионе Поражение тонкой кишки - колиты
Поражение тонкой кишки - колиты Физическая реабилитация и коррекция плоскостопия у детей дошкольного возраста (5-6 лет)
Физическая реабилитация и коррекция плоскостопия у детей дошкольного возраста (5-6 лет) Общая пропедевтика системы пищеварения
Общая пропедевтика системы пищеварения Пищеварительная система. Занятие №1
Пищеварительная система. Занятие №1