Содержание
- 2. Infection most commonly involves heart valves (either native or prostatic) but may also occur on the
- 3. Incidence – 2.6-7:100,000 in the western world. Increasing among elderly. Predisposition – congenital heart disease, rheumatic
- 4. Clinical manifestation Cardiac manifestations Murmur 80-85% CHF 30-40% Arrhythmia Pericarditis Coronary emboli Non cardiac manifestations Fever
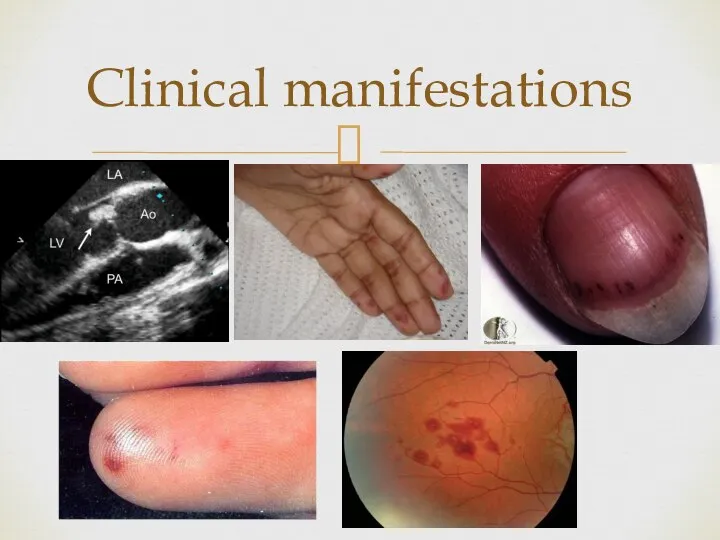
- 5. Clinical manifestations
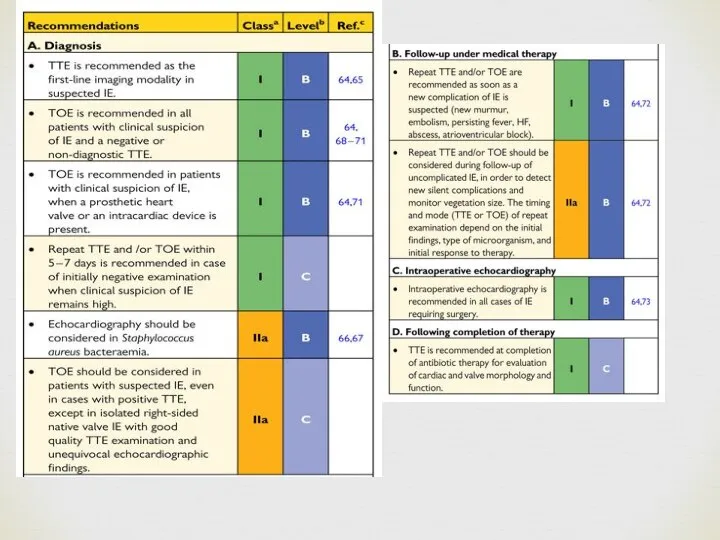
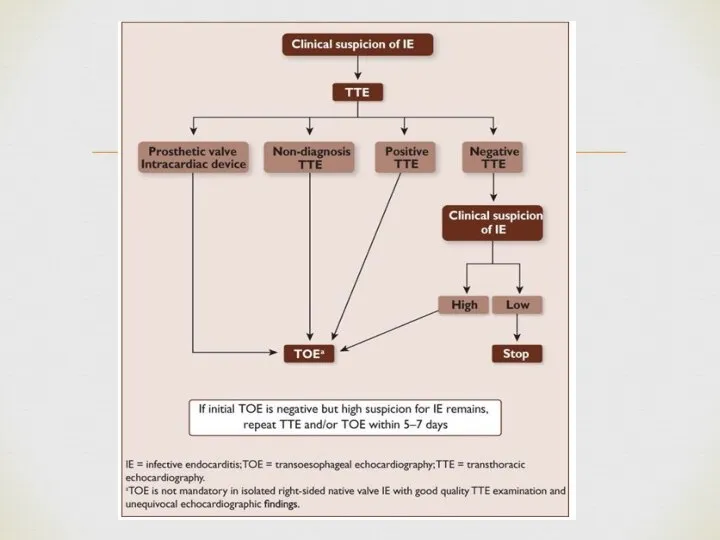
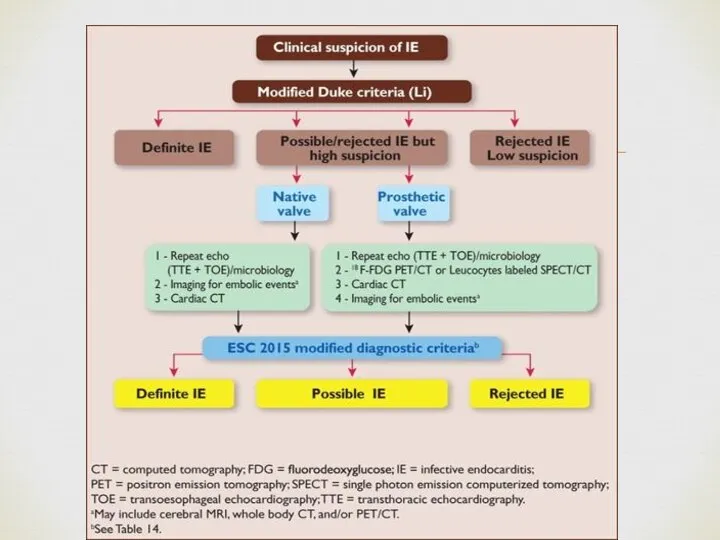
- 6. Diagnosis – Duke criteria Definite IE: Histology or culture of a cardiac vegetation, an embolized vegetation,
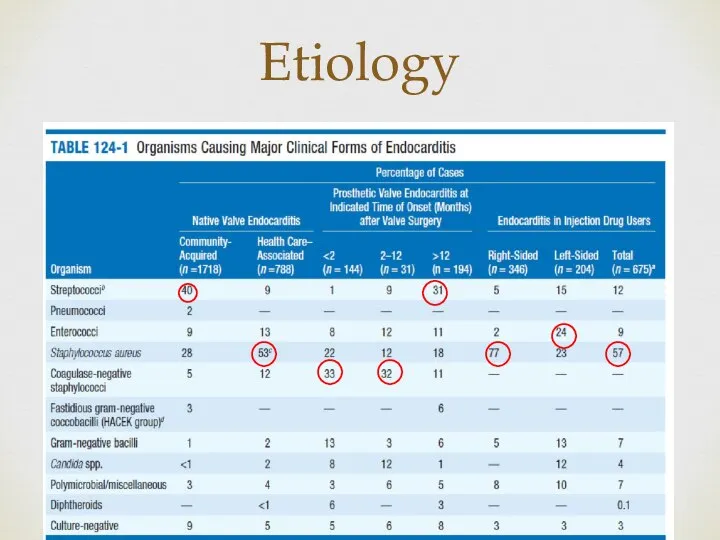
- 10. Etiology
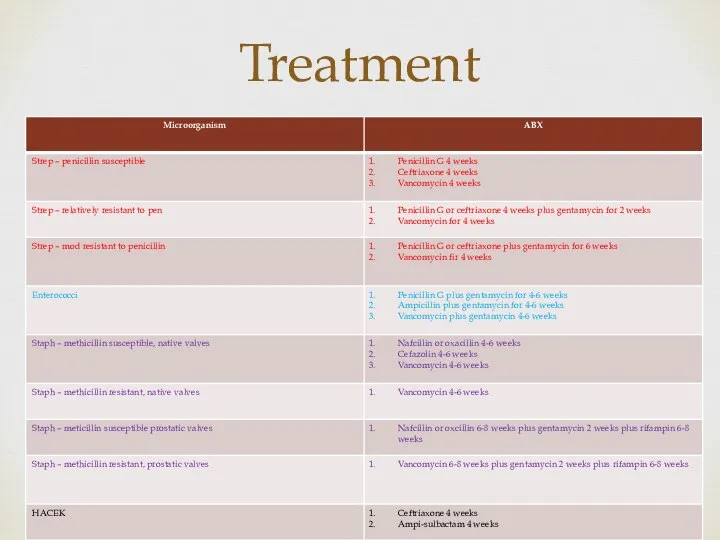
- 11. Treatment
- 12. B. quintana and B. henselae are the most common bartonella spp. implicated in endocarditis. Native valves
- 13. C. brunetti Gram neg cocco-bacillus Primary sources – cattle, sheep and goats Incidence – 24-54 cases
- 14. Main complications of left-sided valve infective endocarditis and their management HF is the most frequent and
- 15. Uncontrolled infection Perivalvular extension of IE is the most frequent cause of uncontrolled infection and is
- 16. Neurological complications Symptomatic neurological events develop in 15–30% of all patients with IE and additional silent
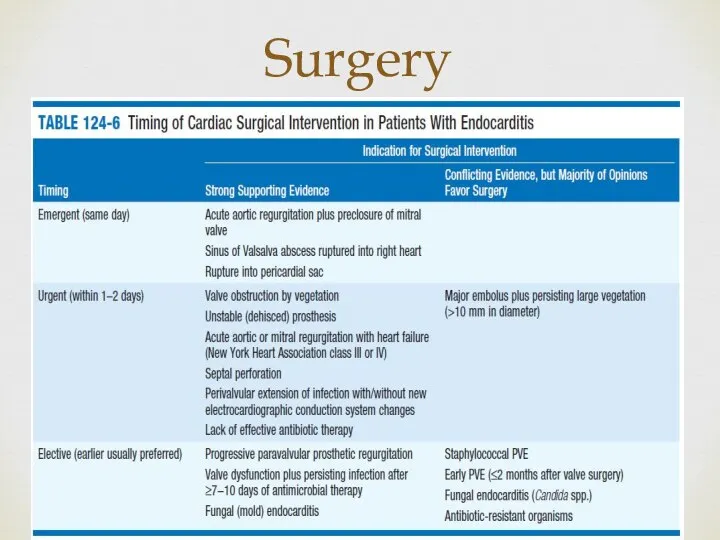
- 17. Surgery
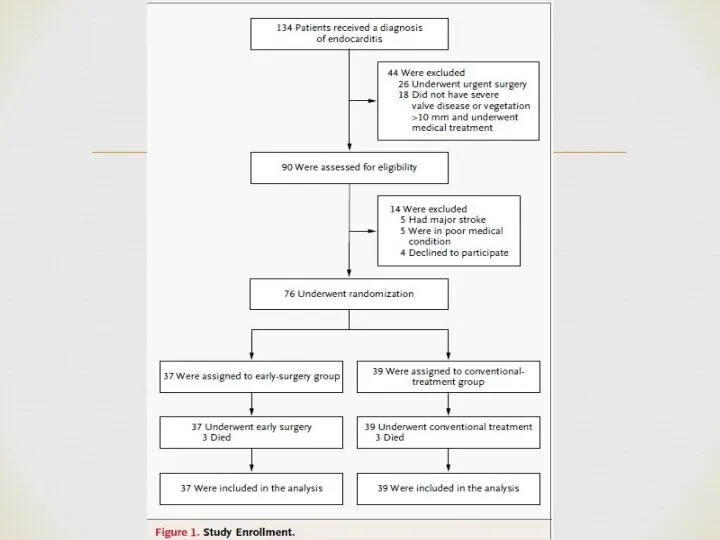
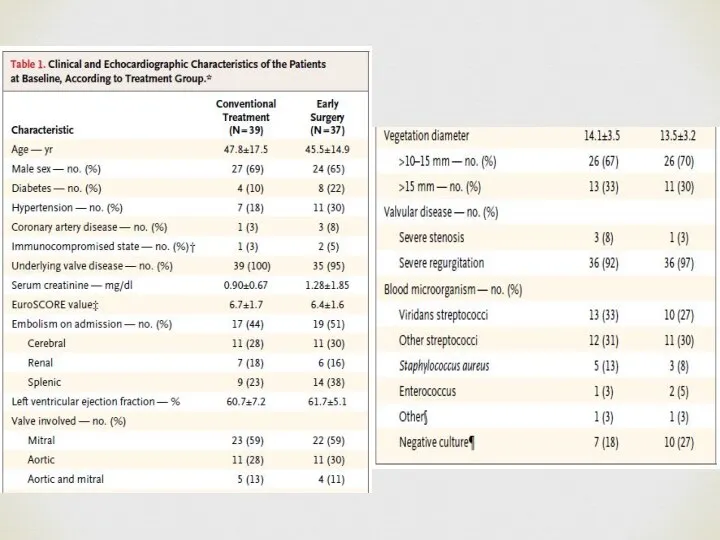
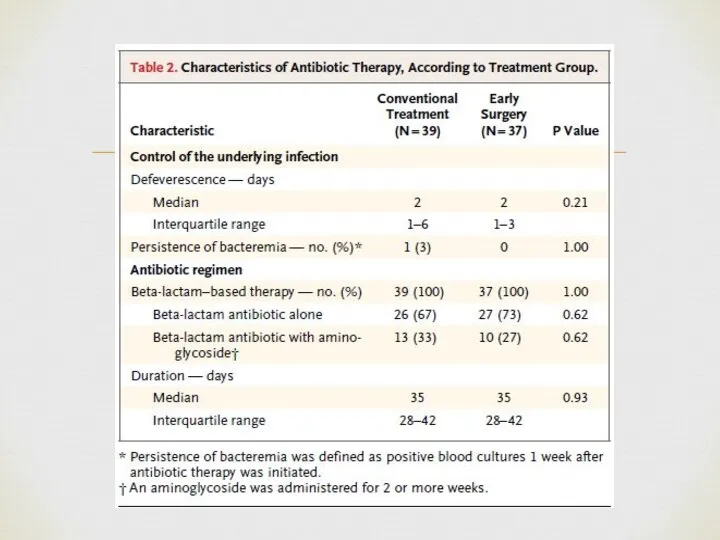
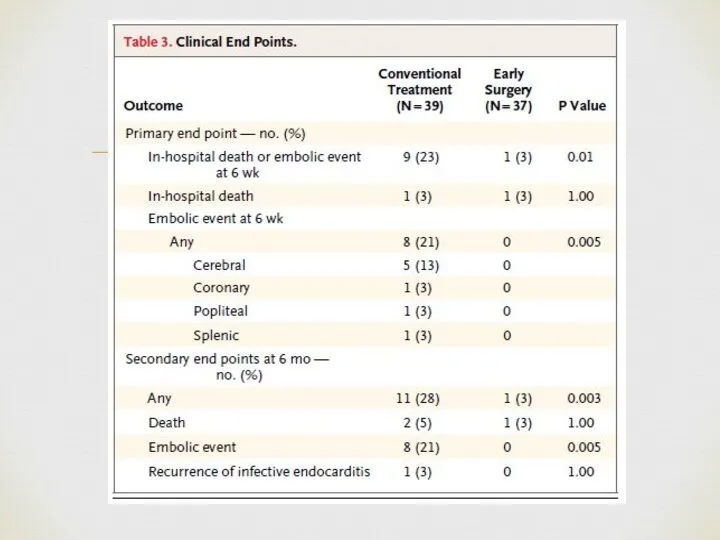
- 24. Patient population: relatively young, low rate of comorbidities. Microbiology: high rate of Streptococcal infections, low rate
- 25. Prophylaxis
- 26. Non-specific prevention measures to be followed in high-risk and intermediate-risk patients
- 27. Recommendations for prophylaxis of infective endocarditis in the highest-risk patients according to the type of at-risk
- 28. Recommendations for antibiotic prophylaxis for the prevention of local and systemic infections before cardiac or vascular
- 29. 49y male Staphylococcus aureus NVE 3 weeks of IV antibiotics Undergoing MVR due to ruptured chorda
- 30. How do you count the duration of therapy? It is reasonable that the counting of days
- 32. Скачать презентацию
















 Технология получения современных вакцин и диагностикумов
Технология получения современных вакцин и диагностикумов Модернизация амбулаторно-поликлинической помощи
Модернизация амбулаторно-поликлинической помощи Гериатрические аспекты в пульмонологии и кардиологии
Гериатрические аспекты в пульмонологии и кардиологии Влияние наушников на слух человека
Влияние наушников на слух человека Фармакология средств, используемых для лечения болезней ЖКТ
Фармакология средств, используемых для лечения болезней ЖКТ Морской конёк (гиппокамп)
Морской конёк (гиппокамп) ALPPS: тайна пяти букв
ALPPS: тайна пяти букв Tverdye_lekarstvennye_formy (1)
Tverdye_lekarstvennye_formy (1) Сказ. Збудник
Сказ. Збудник Макет презентации. Кафедра факультетской педиатрии
Макет презентации. Кафедра факультетской педиатрии Компенсаторные приспособления слепых
Компенсаторные приспособления слепых Рентгенологические особенности строения зубов и челюстей
Рентгенологические особенности строения зубов и челюстей Периартрит локтевого, лучезапястных суставов
Периартрит локтевого, лучезапястных суставов Краниометрия. Медицинаның бассүйекті өлшейтін бөлімі болып табылады
Краниометрия. Медицинаның бассүйекті өлшейтін бөлімі болып табылады Медицинская помощь при бесплодии. Программа Аңсаған сәби
Медицинская помощь при бесплодии. Программа Аңсаған сәби Рекомендации ESC/ESH по лечению артериальной гипертензии
Рекомендации ESC/ESH по лечению артериальной гипертензии Санитарно- эпидемиологические требования к устройству, оборудованию и содержанию парикмахерских
Санитарно- эпидемиологические требования к устройству, оборудованию и содержанию парикмахерских Ингибиторы циклооксигеназы
Ингибиторы циклооксигеназы Вроджені вади розвитку шлунково-кишкового тракту
Вроджені вади розвитку шлунково-кишкового тракту Обморожение. Часть 1
Обморожение. Часть 1 Актуальные проблемы патогенетической терапии ОКИ (диарейные болезни)
Актуальные проблемы патогенетической терапии ОКИ (диарейные болезни) Урологиялық аспаптар
Урологиялық аспаптар Особенноси ухода за больными с заболеваниями пищеварительной системы
Особенноси ухода за больными с заболеваниями пищеварительной системы физическое здоровье
физическое здоровье История обезболивания
История обезболивания Регуляция осмотического давления
Регуляция осмотического давления Обморожение. Первая помощь при обморожении
Обморожение. Первая помощь при обморожении Внематочная беременность
Внематочная беременность