Содержание
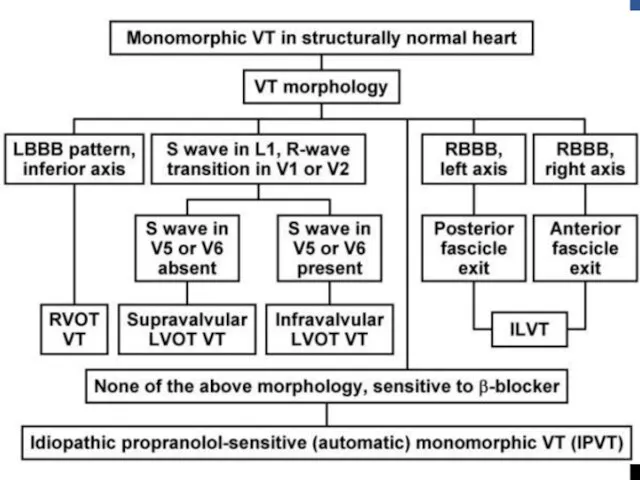
- 2. 10% of patients presenting with VT have no apparent structural heart disease VT in structurally normal
- 3. NON–LIFE-THREATENING (TYPICALLY MONOMORPHIC) Classified on basis of site of origin Most common sites are ventricular outflow
- 4. Idiopathic left VT Left posterior fascicle Left anterior fascicle High septal fascicle Others Mitral annulus Tricuspid
- 5. OUTFLOW TRACT VT Idiopathic VT originate most commonly in outflow tract area Nearly 80% of which
- 6. Phenotypes are a continuum of the same focal cellular process Premature ventricular complexes (PVCs) Nonsustained,repetitive monomorphic
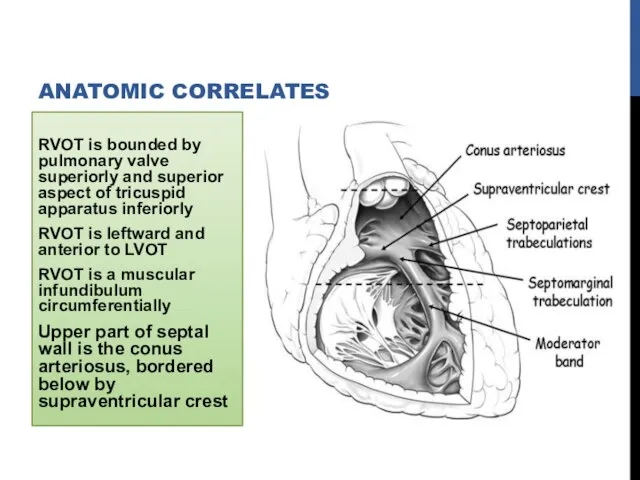
- 7. RVOT is bounded by pulmonary valve superiorly and superior aspect of tricuspid apparatus inferiorly RVOT is
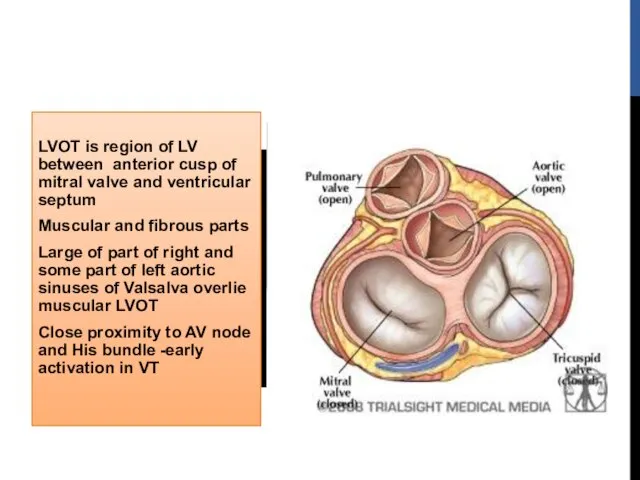
- 8. LVOT is region of LV between anterior cusp of mitral valve and ventricular septum Muscular and
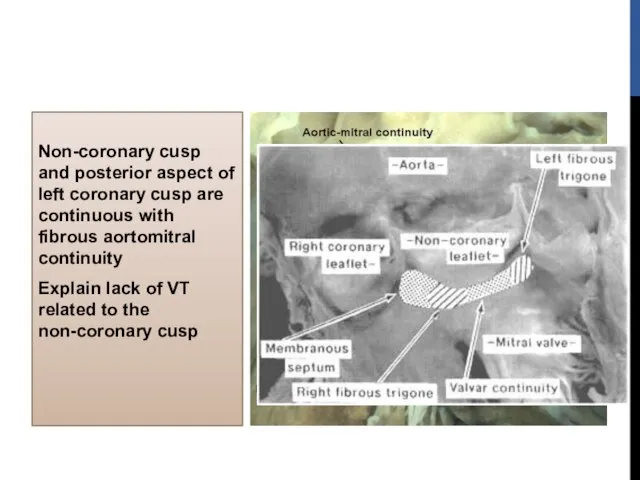
- 9. Non-coronary cusp and posterior aspect of left coronary cusp are continuous with fibrous aortomitral continuity Explain
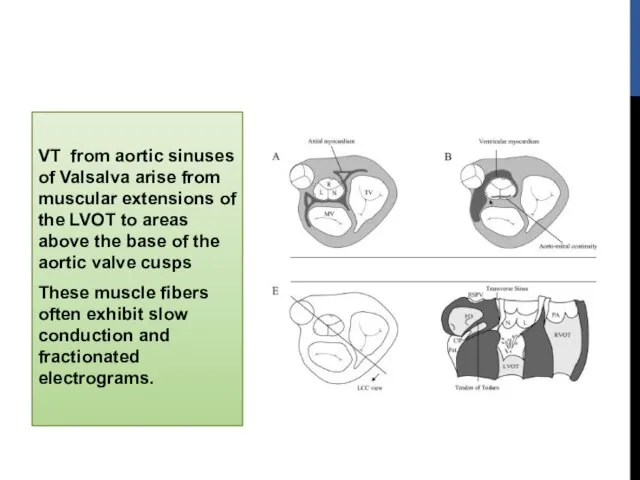
- 10. VT from aortic sinuses of Valsalva arise from muscular extensions of the LVOT to areas above
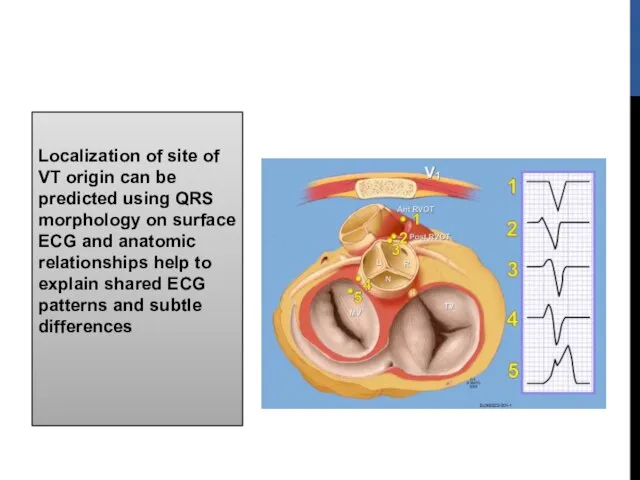
- 11. Localization of site of VT origin can be predicted using QRS morphology on surface ECG and
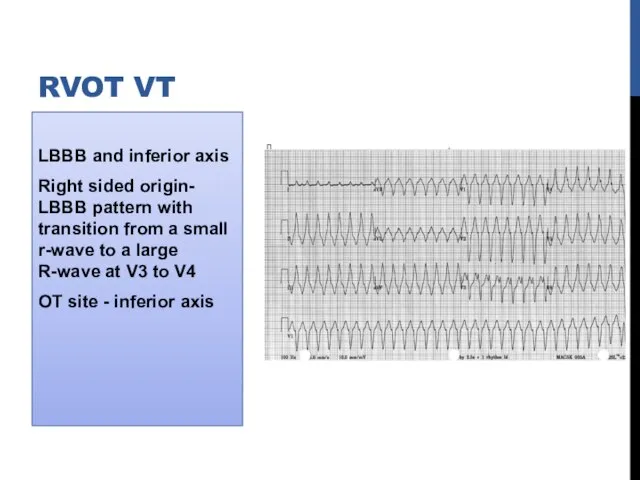
- 12. LBBB and inferior axis Right sided origin- LBBB pattern with transition from a small r-wave to
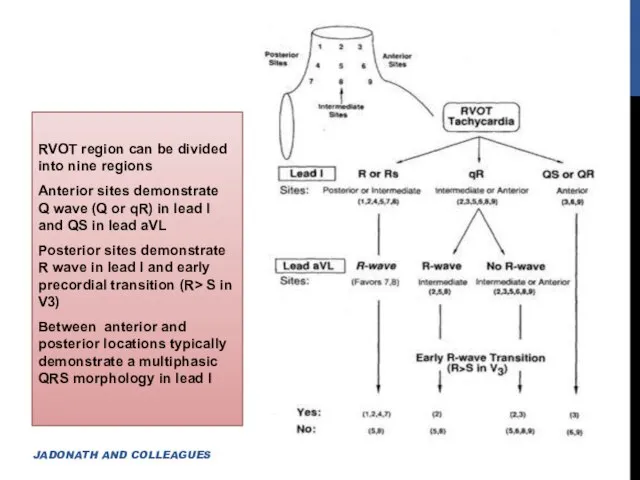
- 13. RVOT region can be divided into nine regions Anterior sites demonstrate Q wave (Q or qR)
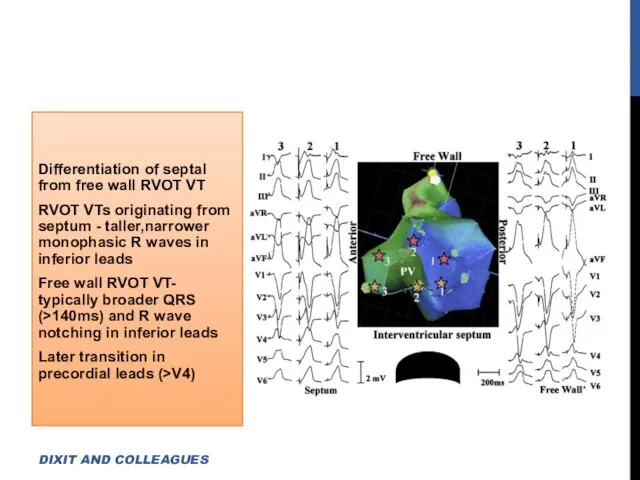
- 14. Differentiation of septal from free wall RVOT VT RVOT VTs originating from septum - taller,narrower monophasic
- 15. Anterior position of free wall relative to septum -Accounts for deeper S wave in lead V2
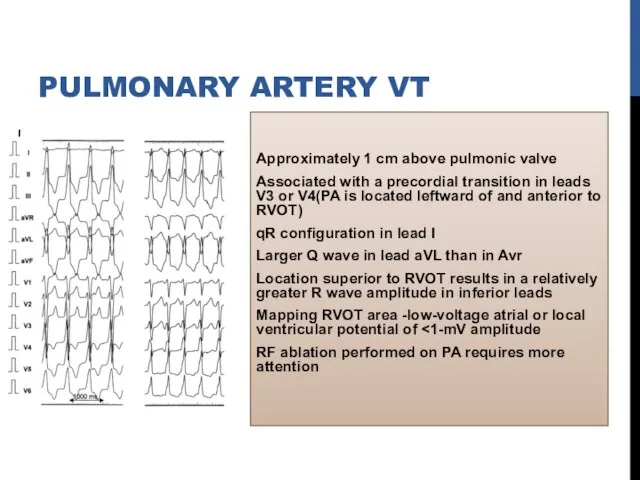
- 16. Approximately 1 cm above pulmonic valve Associated with a precordial transition in leads V3 or V4(PA
- 17. Atriofascicular fibers (Mahaim fibers) AVRT using Rt-sided accessory pathway VT after repair of TOF ARVD DIFFERENTIAL
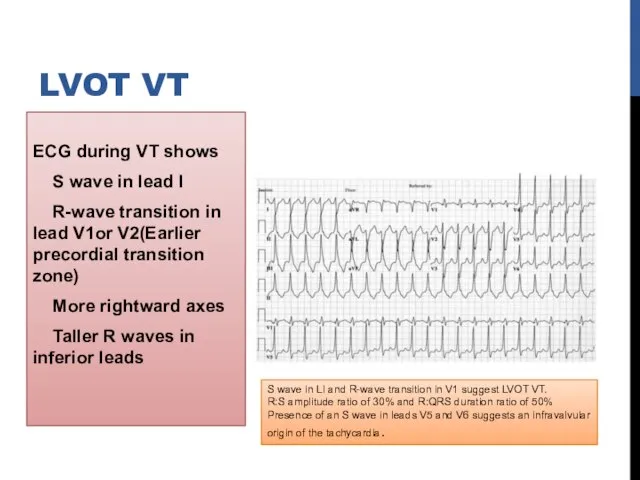
- 18. ECG during VT shows S wave in lead I R-wave transition in lead V1or V2(Earlier precordial
- 19. Shows one of the following depending on site of origin a)Basal left interventricular or septal origin
- 20. May originate from supravalvular or infravalvular endocardial region of coronary cusp of aortic valve Distinction is
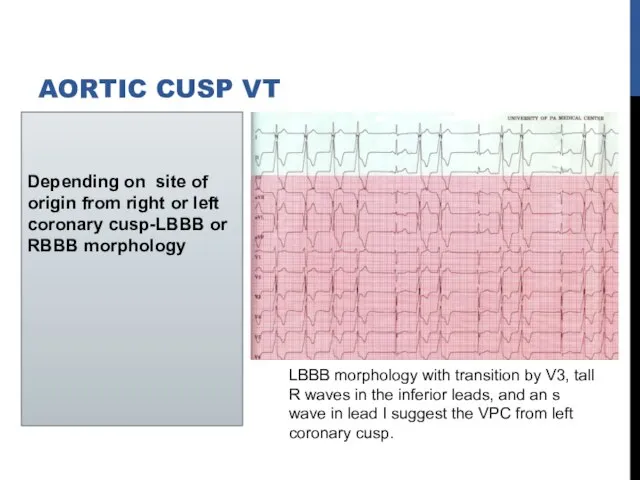
- 21. Depending on site of origin from right or left coronary cusp-LBBB or RBBB morphology AORTIC CUSP
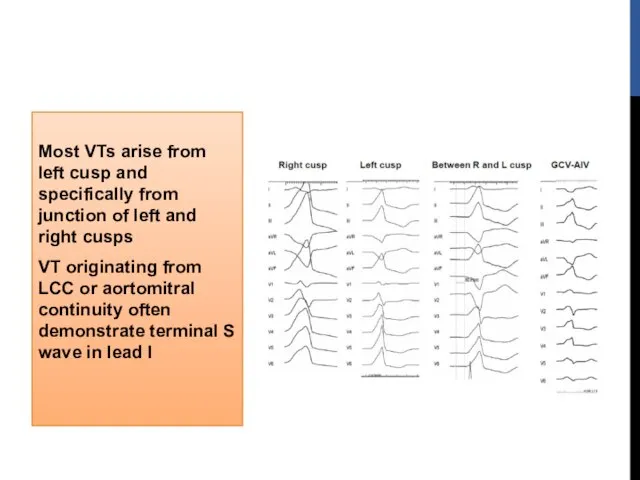
- 22. Most VTs arise from left cusp and specifically from junction of left and right cusps VT
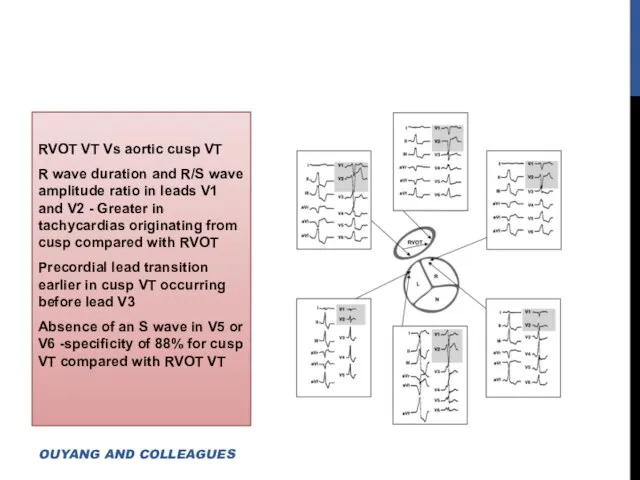
- 23. RVOT VT Vs aortic cusp VT R wave duration and R/S wave amplitude ratio in leads
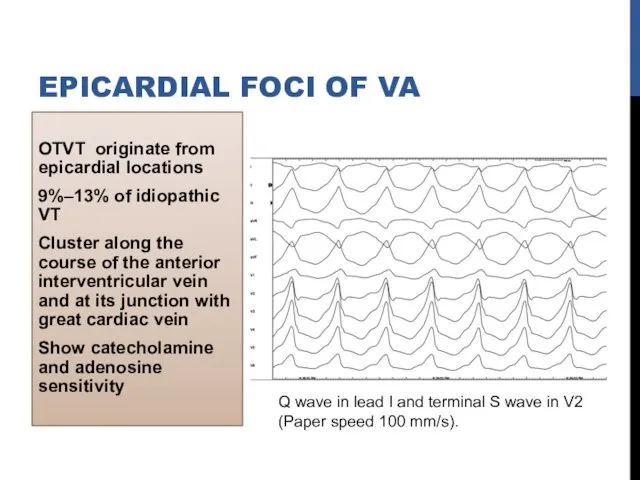
- 24. OTVT originate from epicardial locations 9%–13% of idiopathic VT Cluster along the course of the anterior
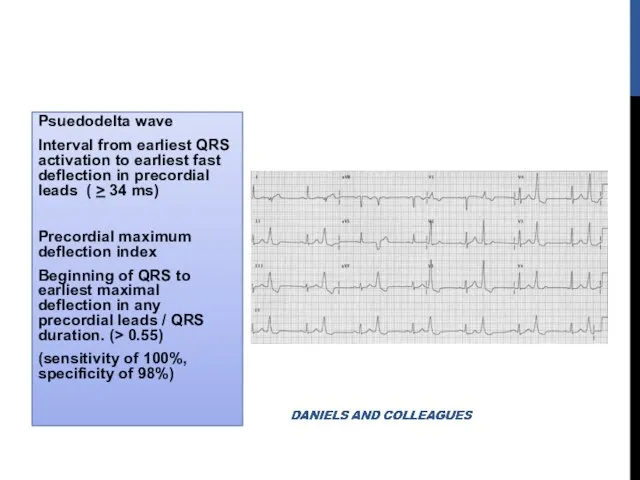
- 25. Psuedodelta wave Interval from earliest QRS activation to earliest fast deflection in precordial leads ( >
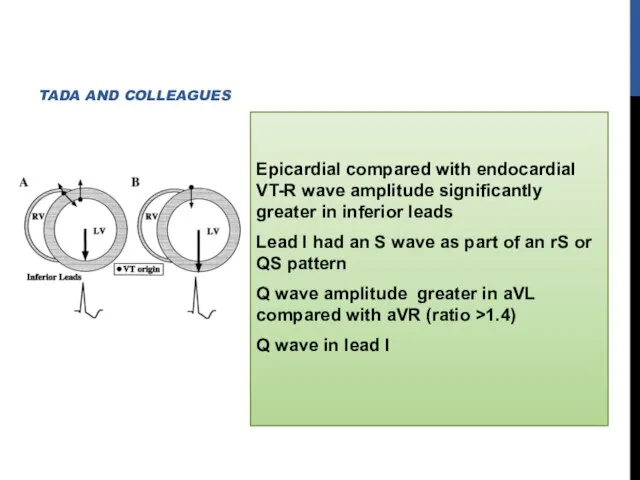
- 26. Epicardial compared with endocardial VT-R wave amplitude significantly greater in inferior leads Lead I had an
- 27. MITRAL ANNULUS, TRICUSPID ANNULUS PAPILLARY MUSCLE PERIVASCULAR EPICARDIAL ECTOPY
- 28. MITRAL ANNULAR VT Significant slurring of QRS complex onset resembling delta-wave Regardless of where along circumference
- 29. PVCs or VT also originate from RVOT along region of tricuspid annulus Most common site is
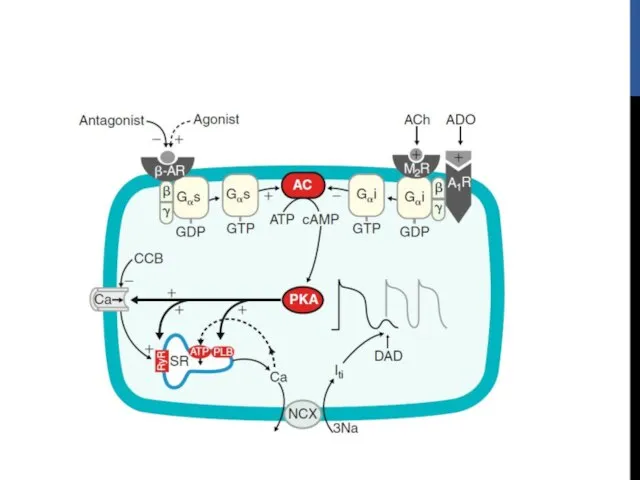
- 30. ELECTROPHYSIOLOGIC MECHANISM Outflow tract VT is due to triggered activity Secondary to cyclic AMP mediated DAD
- 32. CLINICAL FEATURES 20 and 40 years,Slight female preponderance May be asymptomatic but often present with palpitations,
- 33. TREATMENT May respond acutely to carotid sinus massage, Valsalva maneuvers or intravenous adenosine or verapamil Long-term
- 34. RFA When medical therapy is ineffective or not tolerated High success rate (>80%) Ablation of epicardial
- 35. Tachycardia localization 12-lead ECG Intracardiac activation Pace mapping
- 36. BIPOLAR ACTIVATION MAPPING
- 37. PACE MAPPING Useful because typically site of origin is focal and because underlying tissue is normal
- 38. ELECTROANATOMIC RE-CREATION OF 3D ANATOMY Helpful for catheter mapping and localization of site of origin Incessant
- 39. Predictors for successful ablation Single VT morphology Accurate pace maps Absence of a deltalike wave at
- 40. Some tachycardias arise from epicardium, necessitate ablation from great cardiac vein or epicardium itself using pericardial
- 41. Complications during outflow tract VT ablation are rare RBBB (1%) Cardiac perforation Damage to the coronary
- 42. IDIOPATHIC LEFT VT Three varieties left posterior fascicular VT -RBBB and LAD (90%) left anterior fascicular
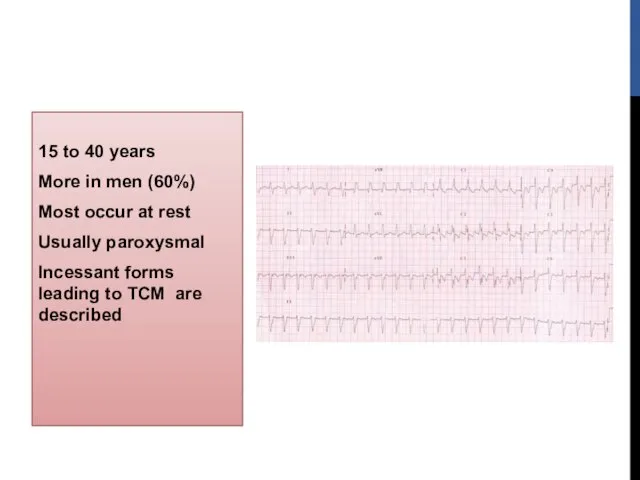
- 43. 15 to 40 years More in men (60%) Most occur at rest Usually paroxysmal Incessant forms
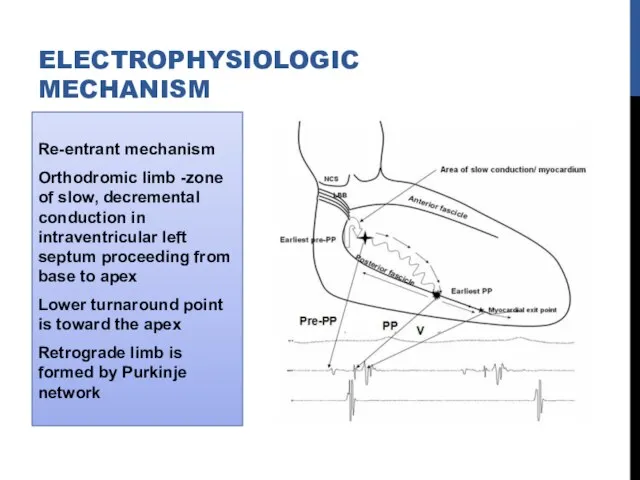
- 44. Re-entrant mechanism Orthodromic limb -zone of slow, decremental conduction in intraventricular left septum proceeding from base
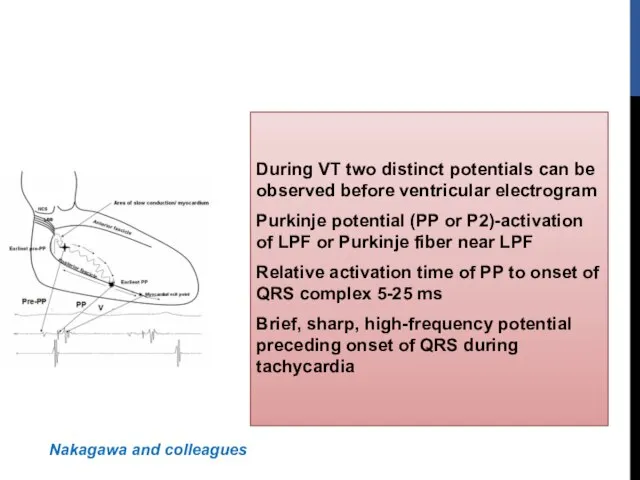
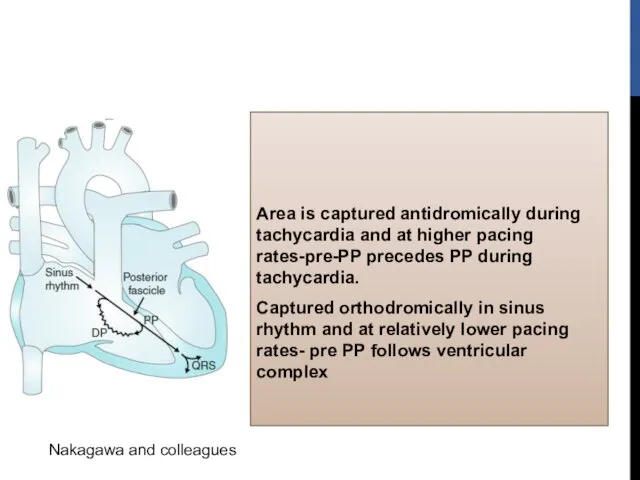
- 45. During VT two distinct potentials can be observed before ventricular electrogram Purkinje potential (PP or P2)-activation
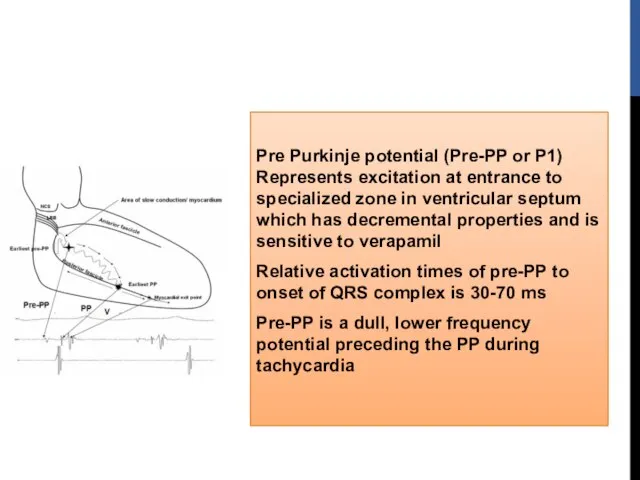
- 46. Pre Purkinje potential (Pre-PP or P1) Represents excitation at entrance to specialized zone in ventricular septum
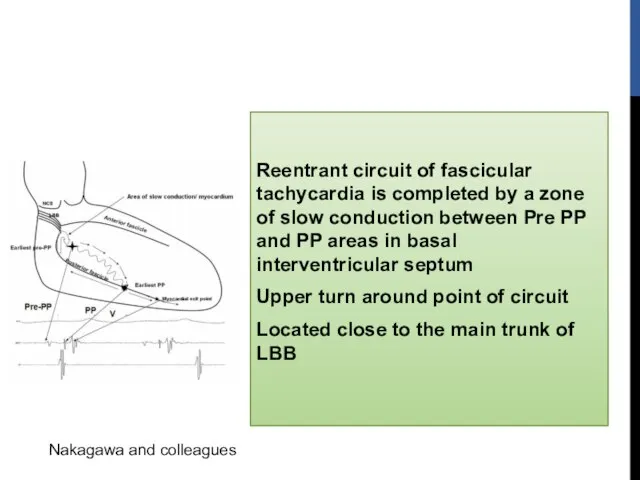
- 47. Reentrant circuit of fascicular tachycardia is completed by a zone of slow conduction between Pre PP
- 48. Area is captured antidromically during tachycardia and at higher pacing rates-pre-PP precedes PP during tachycardia. Captured
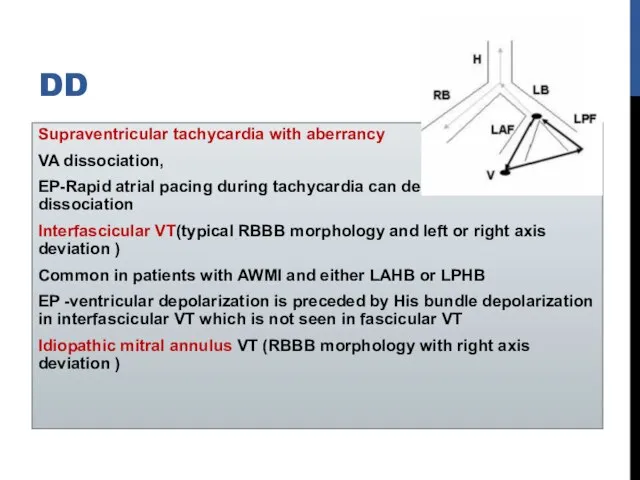
- 49. DD Supraventricular tachycardia with aberrancy VA dissociation, EP-Rapid atrial pacing during tachycardia can demonstrate AV dissociation
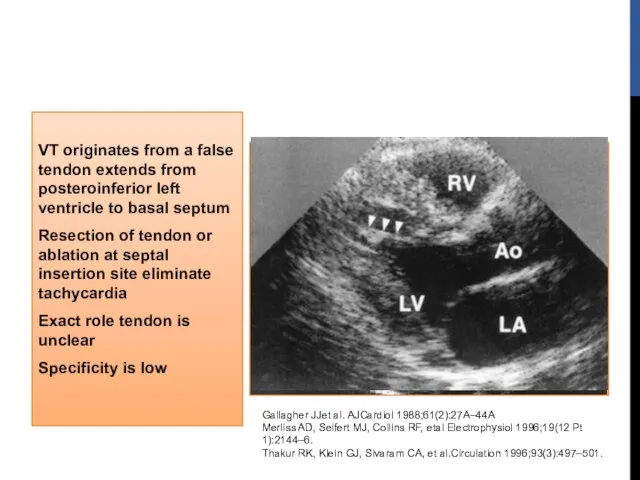
- 50. VT originates from a false tendon extends from posteroinferior left ventricle to basal septum Resection of
- 51. ECG Baseline 12-lead ECG is normal in most patients Exit near the area of the left
- 52. Long-term prognosis is very good Patients who have incessant tachycardia may develop tachycardia related cardiomyopathy Intravenous
- 53. RADIOFREQUENCY ABLATION Associated with significant symptoms or who are intolerant or resistant to medical therapy Strategies
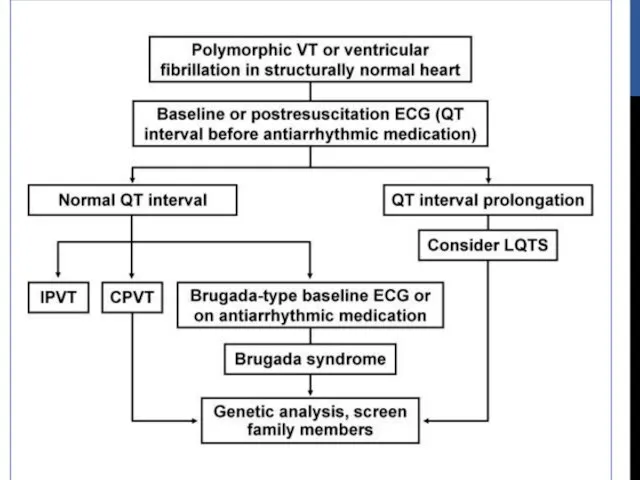
- 54. LIFE-THREATENING (TYPICALLY POLYMORPHIC VT) Rare Generally occurs with genetic ion channel disorders Associated with SCD Abnormalities
- 55. Long QT Syndrome Brugada Syndrome CPVT Short QT Syndrome LIFE-THREATENING (TYPICALLY POLYMORPHIC VT)
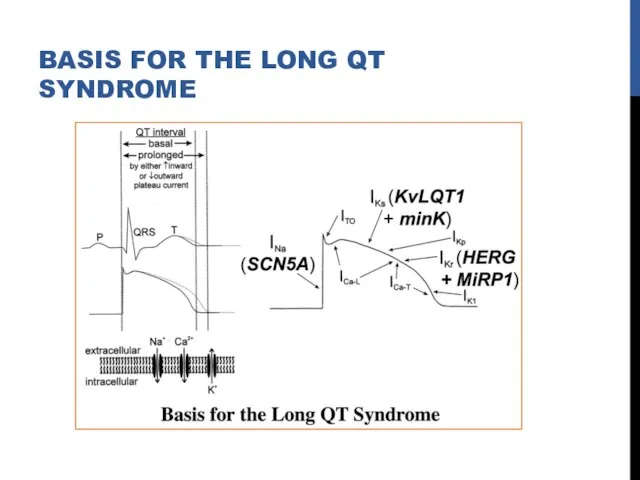
- 56. LONG QT SYNDROME Corrected QT interval 440 ms in men and 460 ms in women with
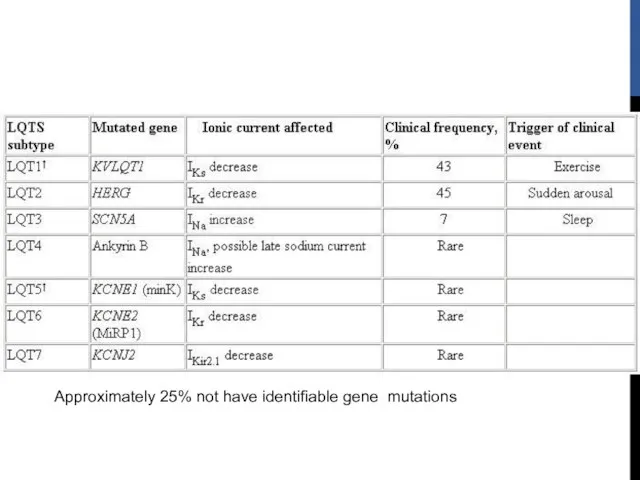
- 57. BASIS FOR THE LONG QT SYNDROME
- 58. Approximately 25% not have identifiable gene mutations
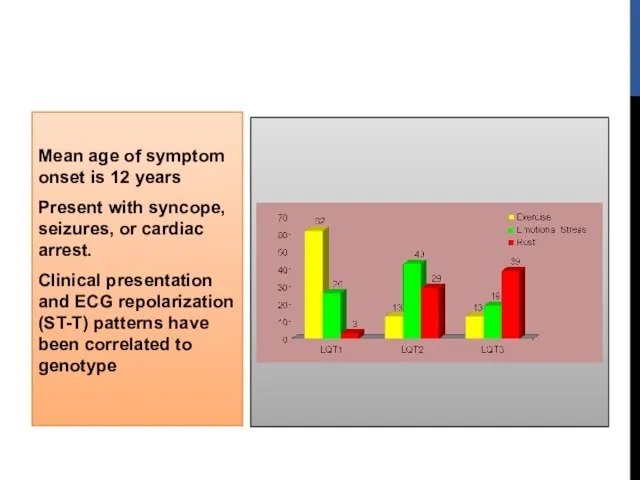
- 59. Mean age of symptom onset is 12 years Present with syncope, seizures, or cardiac arrest. Clinical
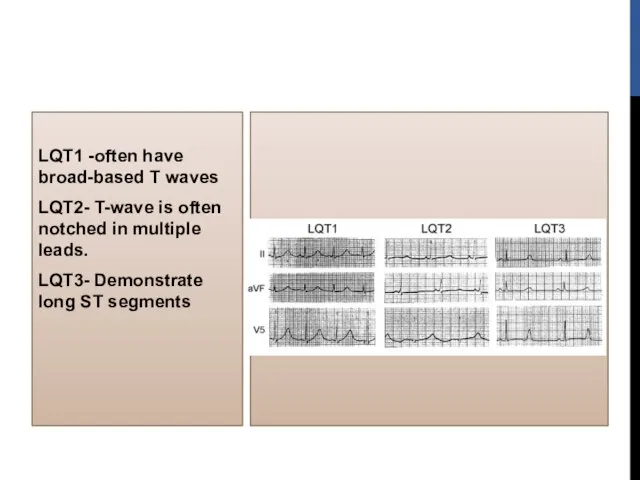
- 60. LQT1 -often have broad-based T waves LQT2- T-wave is often notched in multiple leads. LQT3- Demonstrate
- 62. MANAGEMENT Avoid trigger events and medications prolong QT interval Risk stratification -degree of QT prolongation, genotype
- 63. MEDICATIONS PROLONG QT INTERVAL Antiarrhythmic: procainamide, quinidine, amiodarone, sotalol Antihistamine: astemizole, terfenadine Antimicrobial/antifungal: trimethoprim sulfa, erythromycin,
- 64. MANAGEMENT BB -patients with syncope and asymptomatic patients with significant QT prolongation Role of BB in
- 65. MANAGEMENT ICD are indicated for secondary prevention of cardiac arrest and for patients with recurrent syncope
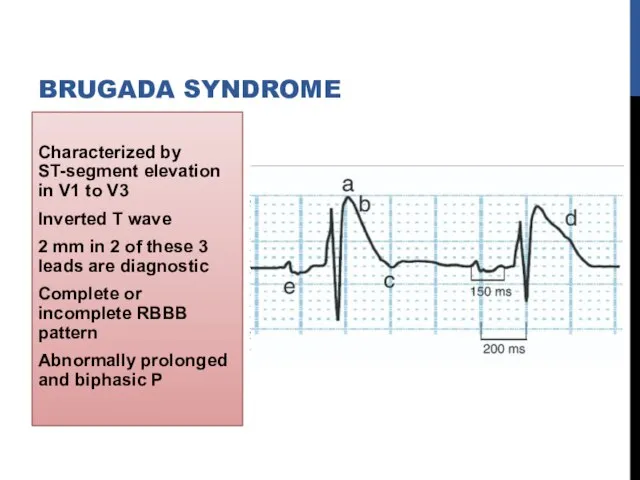
- 66. Characterized by ST-segment elevation in V1 to V3 Inverted T wave 2 mm in 2 of
- 67. ST-SEGMENT ABNORMALITIES IN LEADS V1 TO V3
- 68. Typical ECG pattern can be transient and may only be detected during long-term ECG monitoring Methods
- 69. CLINICAL PRESENTATION 0.12% to 0.14% in general population Syncope or cardiac arrest Predominantly in men in
- 70. Risk of SCD with Brugada syndrome is substantial Risk of recurrent events during 4 years of
- 71. TREATMENT Drugs inhibit Ito (such as quinidine) and increase calcium current (such as isoproterenol) are effective
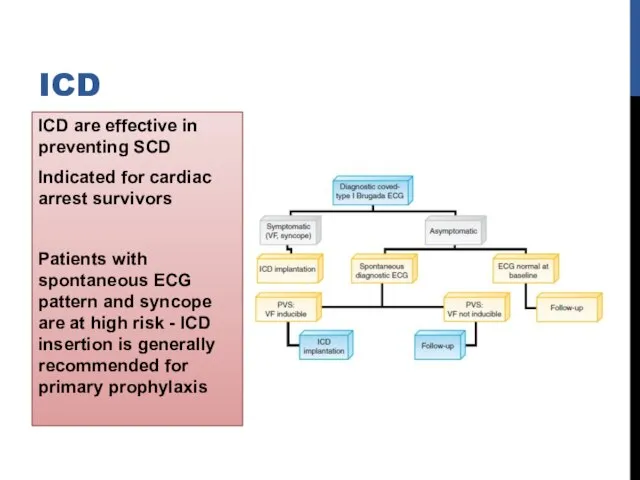
- 72. ICD are effective in preventing SCD Indicated for cardiac arrest survivors Patients with spontaneous ECG pattern
- 73. Different genes involved SCN5A gene mutations (BrS1) - loss of function of cardiac sodium channel (NaV
- 74. Codes for cardiac sodium channel that opens during phase 2 of the action potential In Brugada,
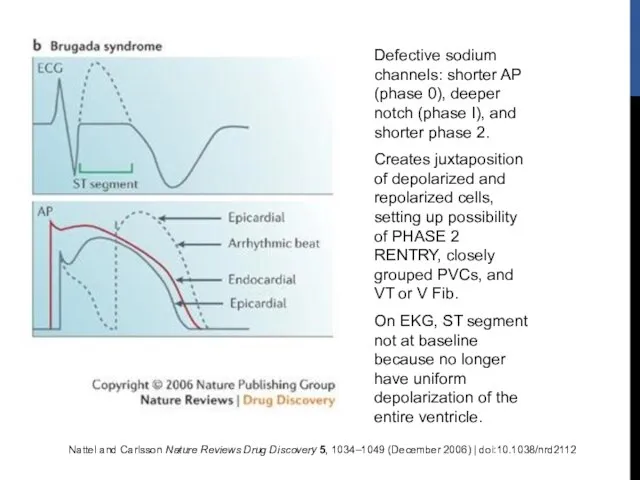
- 75. Nattel and Carlsson Nature Reviews Drug Discovery 5, 1034–1049 (December 2006) | doi:10.1038/nrd2112 Defective sodium channels:
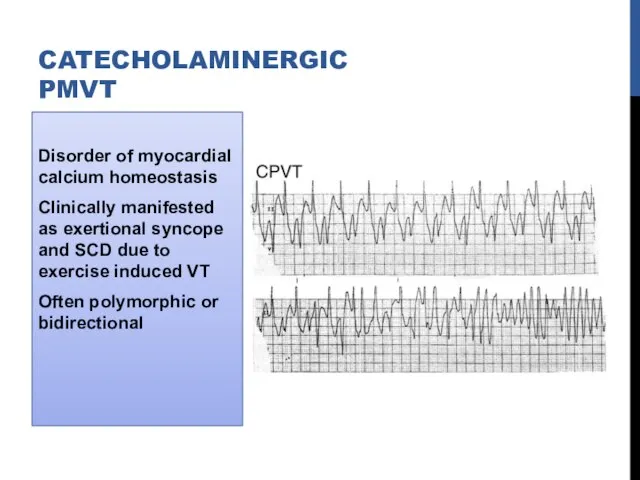
- 76. Disorder of myocardial calcium homeostasis Clinically manifested as exertional syncope and SCD due to exercise induced
- 77. Autosomal dominant (50% )-mutation of cardiac ryanodine receptor (RyR2 gene) Autosomal recessive (3% to 5% )-mutations
- 78. Ryanodine receptor spans membrane of sarcoplasmic reticulum Releases calcium triggered by calcium entry into cell through
- 79. Resting ECG is unremarkable, prominent U waves may be seen Typical VT patterns are reproducible with
- 80. Medical management-BB 46% may have recurrent events while receiving therapy CCB -limited effectiveness Flecainide (blocks RyR2
- 81. ICD Cardiac arrest Life-threatening VA despite maximal medical therapy Initial ICD shock with its accompanying pain
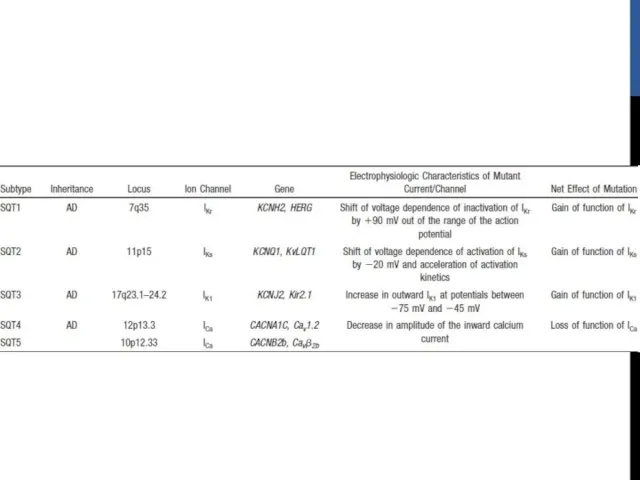
- 82. SHORT QT SYNDROME Rare disorder Characterized by short QT intervals of 300 to 320 ms Shortening
- 84. ICD implantation for secondary and primary prevention Preliminary observations suggest quinidine might be useful
- 85. IDIOPATHIC PROPRANOLOL-SENSITIVE VT (IPVT) Usually occurs by fifth decade of life Can arise from LV or
- 86. TREATMENT OF IPVT BBs effective in acute situations Insufficient information available regarding long-term management Survivors of
- 89. REFERENCES ZIPES 5th EDITION BRAUNWALD 9TH EDITION HURST 13TH EDITION VENTRICULAR ARRHYTHMIAS IN NORMAL HEARTS,SHUAIB LATIF,
- 91. Скачать презентацию


















































 Сердечно-сосудистая система
Сердечно-сосудистая система Отравление парацетамолом
Отравление парацетамолом Кариес. Кариесогенные факторы в полости рта. Способы их выявления и устранения. Зубные отложения и методы их выявления
Кариес. Кариесогенные факторы в полости рта. Способы их выявления и устранения. Зубные отложения и методы их выявления Первая помощь при получении солнечных ожогов, солнечных и тепловых ударов
Первая помощь при получении солнечных ожогов, солнечных и тепловых ударов Портфолио по учебной практике
Портфолио по учебной практике Болезнь Пфаундлера — Гурлер, гаргоилизм
Болезнь Пфаундлера — Гурлер, гаргоилизм Опиоидные аналгетики
Опиоидные аналгетики Женская половая система
Женская половая система Сознание больного
Сознание больного Вывих надколенника
Вывих надколенника Тропические болезни - новая медико-биологическая проблема сибирского региона
Тропические болезни - новая медико-биологическая проблема сибирского региона Аденоиды
Аденоиды Как танец влияет на здоровье человека
Как танец влияет на здоровье человека Синдром обструктивного апноэ сна (СОАС)
Синдром обструктивного апноэ сна (СОАС) Анатомо-физиологические особенности строения полости рта в возрастном аспекте
Анатомо-физиологические особенности строения полости рта в возрастном аспекте Нәрестелерде туа пайда болған бауыр патологиясы
Нәрестелерде туа пайда болған бауыр патологиясы Заболевания желчевыводящей системы и поджелудочной железы
Заболевания желчевыводящей системы и поджелудочной железы Патология репродуктивной системы у собак
Патология репродуктивной системы у собак юперио сент 1
юперио сент 1 Привлечение медицинских работников. Мурманская область
Привлечение медицинских работников. Мурманская область АнтиХрапин
АнтиХрапин Синдром Лериша
Синдром Лериша UCSC Genome Browser
UCSC Genome Browser Пневмонии у детей
Пневмонии у детей Гемолитические анемии, обусловленные дефицитом глюкозо-6-фосфатдегидрогеназы (Г-6-ФДГ)
Гемолитические анемии, обусловленные дефицитом глюкозо-6-фосфатдегидрогеназы (Г-6-ФДГ) Грыжи пищеводного отверстия диафрагмы
Грыжи пищеводного отверстия диафрагмы Отбор гистологического и цитологического материалов
Отбор гистологического и цитологического материалов Уход за тяжелобольными пациентами
Уход за тяжелобольными пациентами