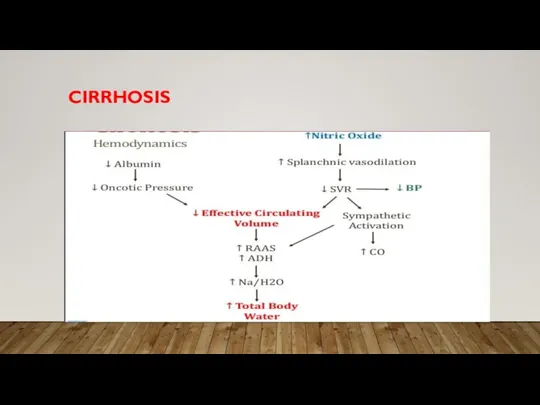
Слайд 2CIRRHOSIS
• End stage liver disease (irreversible)
• Result from many causes of chronic
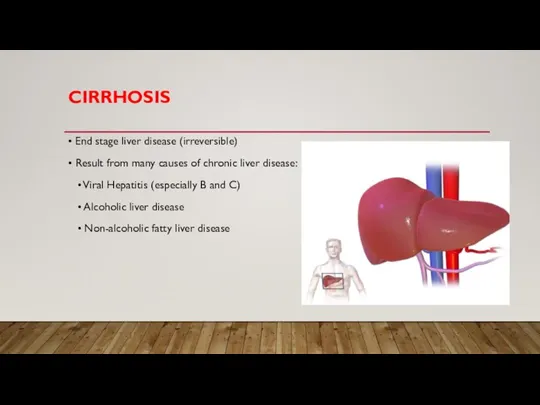
liver disease:
• Viral Hepatitis (especially B and C)
• Alcoholic liver disease
• Non-alcoholic fatty liver disease
Слайд 3CIRRHOSIS
• Liver tissue replaced by fibrosis and nodules
• Smooth liver surface replaced
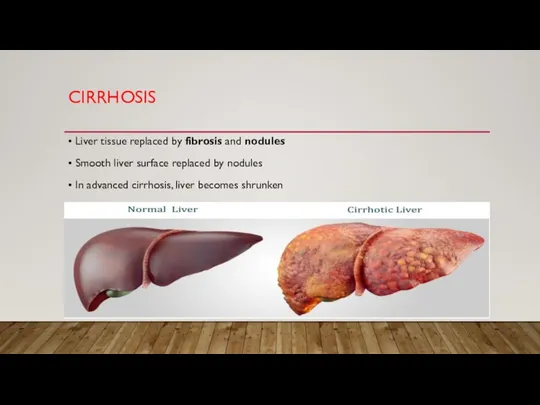
by nodules
• In advanced cirrhosis, liver becomes shrunken
Слайд 4CLINICAL FEATURES
• Hyperammonemia
• Asterixis, confusion, coma

Слайд 5HYPERAMMONEMIA
TREATMENT
• Low protein diet
• Lactulose
• Synthetic disaccharide (laxative)

• Colon breakdown by bacteria to fatty acids
• Lowers colonic pH; favors formation of NH4+ over NH3
• NH4 + not absorbed → trapped in colon
• Result: ↓plasma ammonia concentrations
Слайд 6CIRRHOSIS
CLINICAL FEATURES
• Jaundice
• Loss of bilirubin metabolism
• Hypoglycemia
• Loss

of gluconeogenesis
• Coagulopathy
• Loss of clotting factors
• Elevated PT/PTT
• Hypoalbuminemia
• May cause low oncotic pressure
• Contributes to ascites, edema
Слайд 7• Elevated estrogen
• Normally removed by liver
• Gynecomastia in
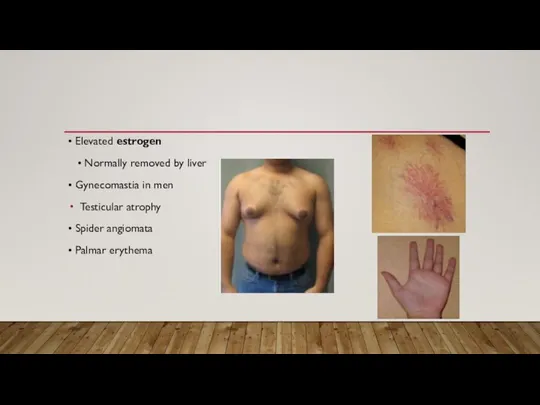
men
Testicular atrophy
• Spider angiomata
• Palmar erythema
Слайд 8CAPILLARY FLUID SHIFTS
• Capillary hydrostatic pressure (Pc)
• Drives fluid out of

capillaries into tissues
• Capillary oncotic pressure (∏c )
• Proteins (albumin) pull water into capillaries
• Resists movement of fluid out of capillaries
Слайд 9PORTAL HYPERTENSION
• Blood flows portal vein → liver → hepatic vein
• Cirrhosis
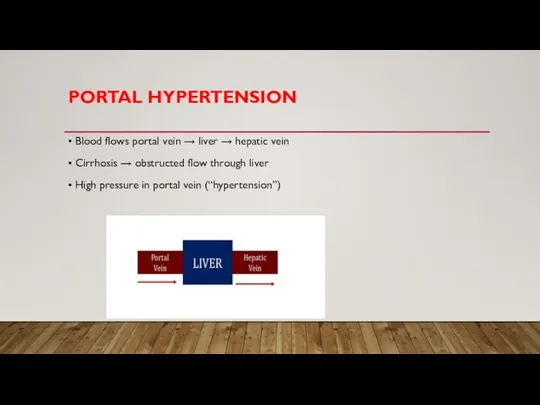
→ obstructed flow through liver
• High pressure in portal vein (“hypertension”)
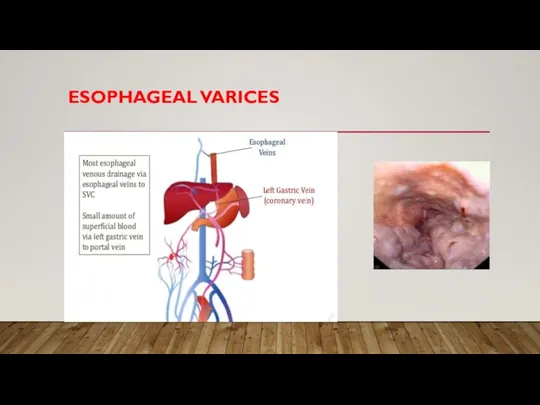
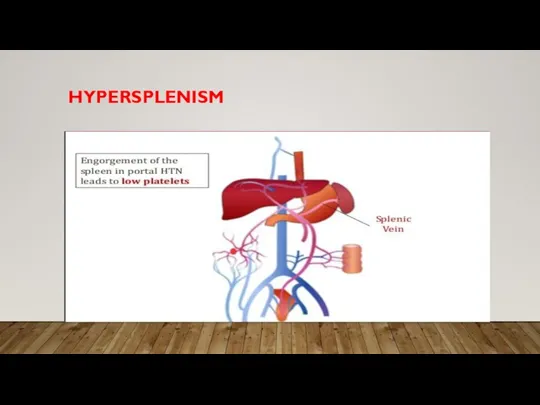
Слайд 12VENOUS COLLATERALS
VENOUS ANASTAMOSES
• High portal pressure opens “venous collaterals”
• Connection between

portal-systemic veins
• Normally small, collapsed vessels
• Engorge in portal hypertension
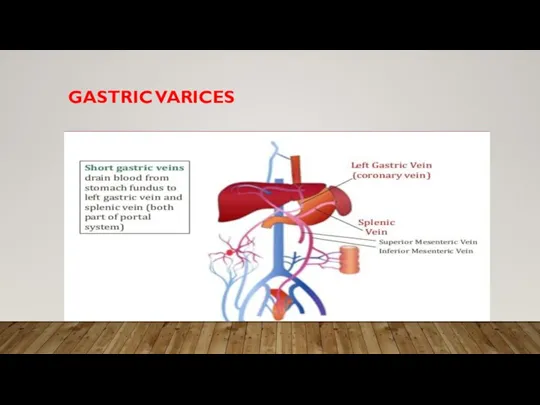
• Key collaterals:
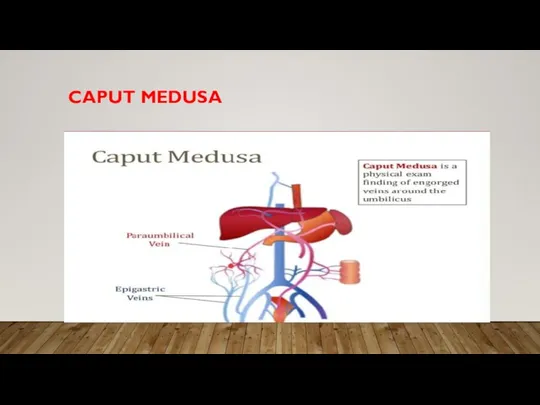
• Umbilicus – physical exam finding: “caput medusa”
• Esophagus – upper gastrointestinal bleeding
• Stomach – upper gastrointestinal bleeding
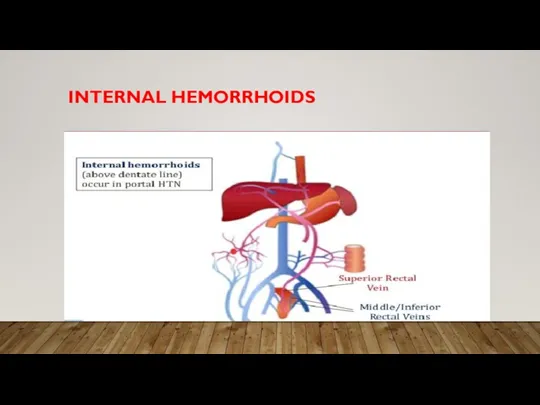
• Rectum – hemorrhoids which may also bleed
Слайд 18PORTAL VEIN THROMBOSIS
• Rare cause of portal hypertension
• Acute onset abdominal

pain
• Splenomegaly (palpable spleen one exam)
• May result in gastric varices with bleeding
• Liver biopsy will be normal
Слайд 19ASCITES
• Accumulation of fluid in peritoneal cavity
• In liver disease, from

portal hypertension +/- low albumin
Слайд 20SAAG
SERUM ASCITES ALBUMIN GRADIENT
• Test of ascitic fluid
• Two reasons

for new/worsening ascites
• Portal hypertension
• Malignancy (leaky vasculature)
• Sample of ascitic fluid via paracentesis
• Serum albumin – ascites albumin = SAAG
Слайд 21SAAG
SERUM ASCITES ALBUMIN GRADIENT
• SAAG >1.1 g/dL
• Large difference

between serum and ascites albumin
• High pressure driving fluid (not albumin) into peritoneum
• Seen in portal hypertension
SAAG <1.1 g/Dl
Albumin levels similar between serum and ascites
• Leaky vasculature leading to fluid/albumin into peritoneum
Seen in malignant ascites (malignant cells in peritoneal cavity)
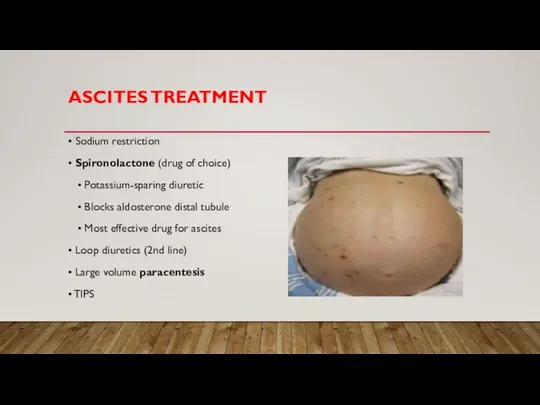
Слайд 22ASCITES TREATMENT
• Sodium restriction
• Spironolactone (drug of choice)
• Potassium-sparing diuretic
• Blocks aldosterone distal tubule
• Most effective drug for ascites
• Loop diuretics (2nd line)
• Large volume paracentesis
• TIPS
Слайд 23TIPS
TRANSJUGULAR INTRAHEPATIC PORTOSYSTEMIC SHUNT
Transjugular Intrahepatic Portosystemic Shunt
• Treatment of portal
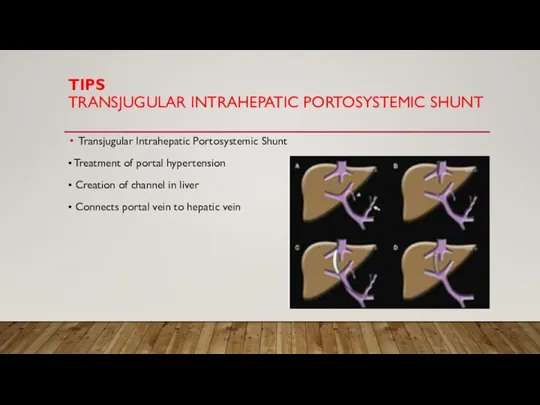
hypertension
• Creation of channel in liver
• Connects portal vein to hepatic vein
Слайд 24SBP
SPONTANEOUS BACTERIAL PERITONITIS
• Ascitic fluid infection
• Bacteria in gut gain

entry into ascitic fluid
• Usually E. coli and Klebsiella; rarely strep/staph
• Fever, abdominal pain/tenderness
• ↑ ascitic absolute PMNs (≥250 cells/mm3)
• Common treatment:
• 3rd generation cephalosporin (cefotaxime)
• Gram positive and gram negative coverage
• Achieves good levels in ascitic fluid
Слайд 25MELD SCORE
MODEL FOR END-STAGE LIVER DISEASE
• Scoring system for chronic liver

disease or cirrhosis
• Estimates 3-month mortality from liver disease
• Point system using:
• Bilirubin level
• Creatinine level
• INR
• >40 = 71% mortality
<9 = 2% mortality
Слайд 26CHILD-PUGH CLASSIFICATION
• Five variables to predict risk/survival
• Points for encephalopathy,

ascites, bilirubin, albumin, PT
• Score ranges from 5 to 15
• 5 or 6: Child-Pugh class A cirrhosis
• 7 to 9: Child-Pugh class B cirrhosis
• 10 to 15: Child-Pugh class C cirrhosis (worst)
Слайд 27CIRRHOSIS
DIAGNOSIS
Gold standard is liver biopsy
• Not required if diagnosis is

clear from history
• Done only when biopsy will change management
• Imaging (ultrasound, CT, MRI)
• May show small, nodular liver
• Not sensitive or specific for diagnosis
• More helpful for detection of hepatocellular carcinoma
• Clinical diagnosis (common)
• Presence of ascites
• Low platelet count
• Spider angiomata



















 Общая тенденции – рост числа детей и подростков с ИЭ
Общая тенденции – рост числа детей и подростков с ИЭ Genetically modified organisms - salvation for the poor and hungry or something poisonous and harmful for people?
Genetically modified organisms - salvation for the poor and hungry or something poisonous and harmful for people? Воспалительные заболевания_02420a36d306cd27840d8606526092dc
Воспалительные заболевания_02420a36d306cd27840d8606526092dc Тонкощі використання інсектоакариців у дрібних тварин
Тонкощі використання інсектоакариців у дрібних тварин Игры с использованием Су-джок терапии для детей с нарушением речи
Игры с использованием Су-джок терапии для детей с нарушением речи Стрептококтар. Стрептококтардың
Стрептококтар. Стрептококтардың Разговор о важном – Предупреждён, значит вооружён. Профилактика ВИЧ-инфекции
Разговор о важном – Предупреждён, значит вооружён. Профилактика ВИЧ-инфекции Сигналінг
Сигналінг Аппараты с пружинящими наклонно-накусочными плоскостями
Аппараты с пружинящими наклонно-накусочными плоскостями Программная реализация системы поддержки принятия решений по выбору эндодонтических файлов
Программная реализация системы поддержки принятия решений по выбору эндодонтических файлов Система крови. Первая помощь в остановке кровотечений
Система крови. Первая помощь в остановке кровотечений Последовательность снятия комплекта средств индивидуальной защиты
Последовательность снятия комплекта средств индивидуальной защиты Артерияның жедел окклюзиясы
Артерияның жедел окклюзиясы Курс детского здоровья
Курс детского здоровья Оборудование и устройство средневековых аптек
Оборудование и устройство средневековых аптек Профилактика сердечно-сосудистых заболеваний
Профилактика сердечно-сосудистых заболеваний Патофизиология системы выделения
Патофизиология системы выделения Гематология
Гематология Полипренолы – природный фактор регенерации живых клеток
Полипренолы – природный фактор регенерации живых клеток Тәуліктік ЭКГ мониторлау
Тәуліктік ЭКГ мониторлау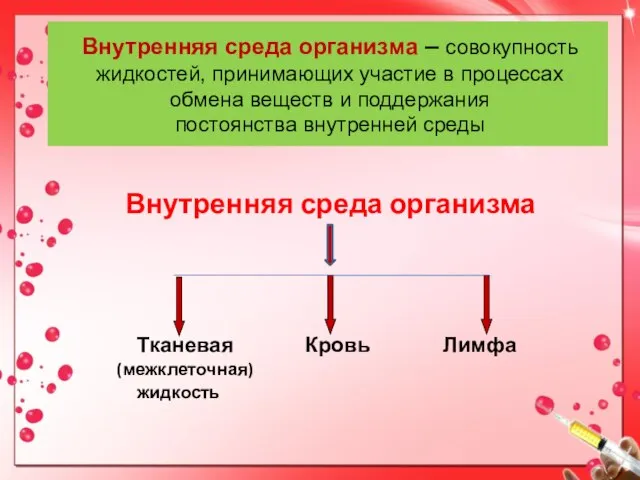 Внутренняя среда организма, клетки крови, кровообращение
Внутренняя среда организма, клетки крови, кровообращение Нормы СанПиН в маникюрном кабинете
Нормы СанПиН в маникюрном кабинете hernia4r
hernia4r Патологии зубочелюстной области и их роль в возникновении заболеваний внутренних органов
Патологии зубочелюстной области и их роль в возникновении заболеваний внутренних органов Новокузнецкая городская клиническая больница №29
Новокузнецкая городская клиническая больница №29 Этические вопросы реанимации новорожденных детей
Этические вопросы реанимации новорожденных детей Плевра куысына сұйықтық жиналу синдромы. Тыныс жетіспеушілігі синдромы
Плевра куысына сұйықтық жиналу синдромы. Тыныс жетіспеушілігі синдромы Эритропоэтин. Eritropoetin
Эритропоэтин. Eritropoetin