Содержание
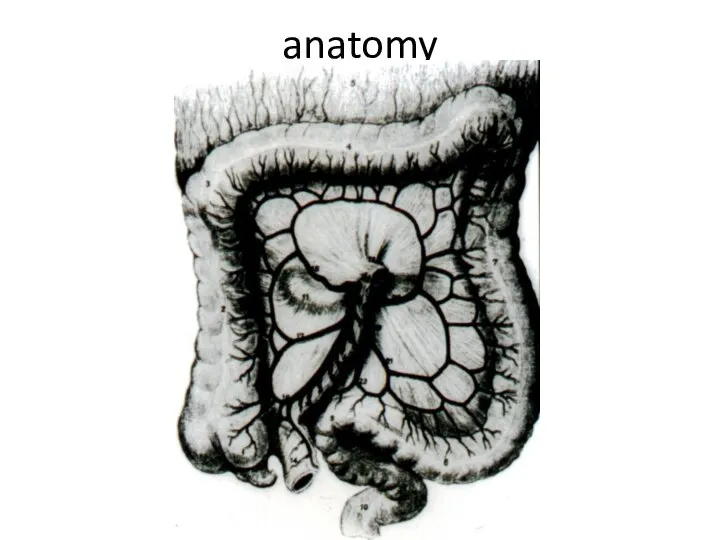
- 2. anatomy
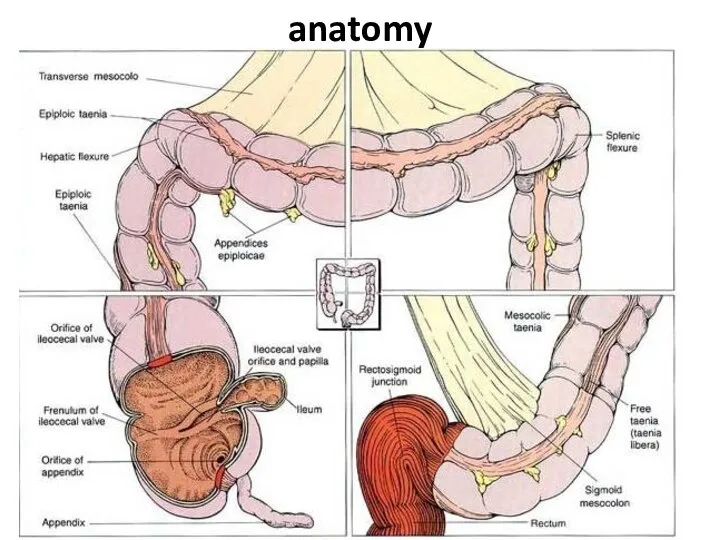
- 3. anatomy
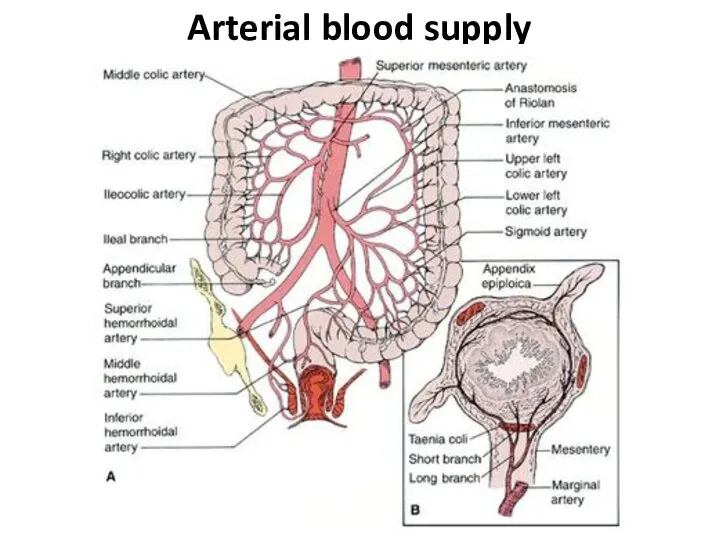
- 4. Arterial blood supply
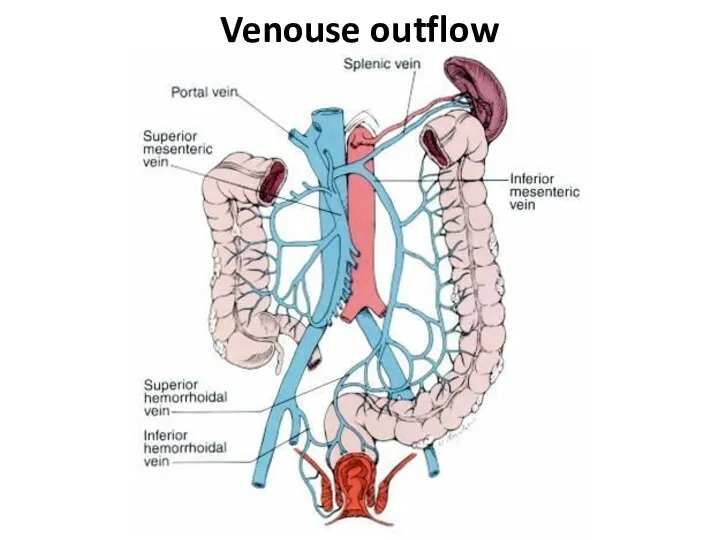
- 5. Venouse outflow
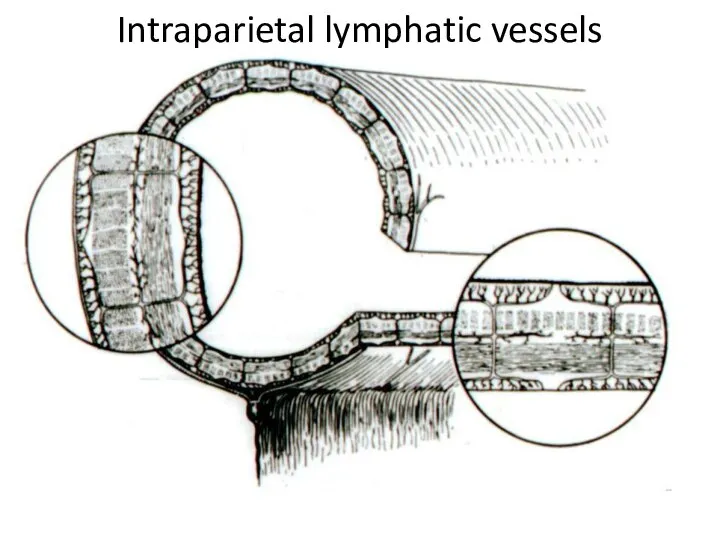
- 6. Intraparietal lymphatic vessels
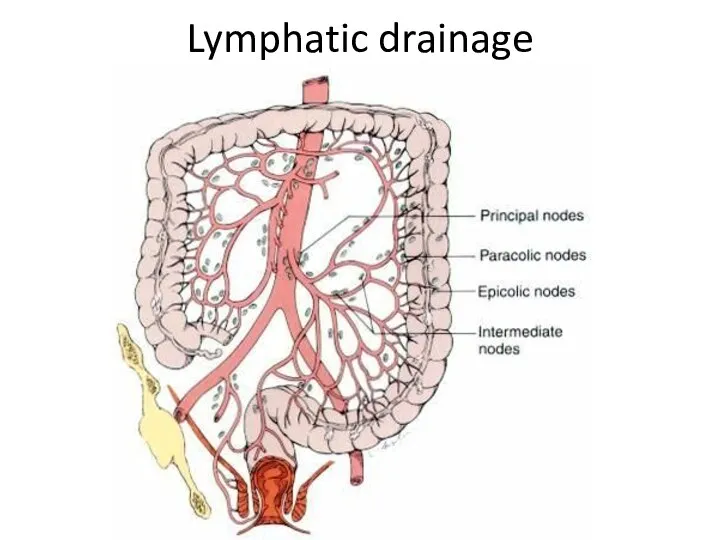
- 7. Lymphatic drainage
- 8. Differences of the right and left half Anatomy: on the right the lumen is wider, than
- 9. Special investigation methods 1. Physical investiga-tion 2. A proctosigmoido-scopy 3. Fibrocolonoscopy
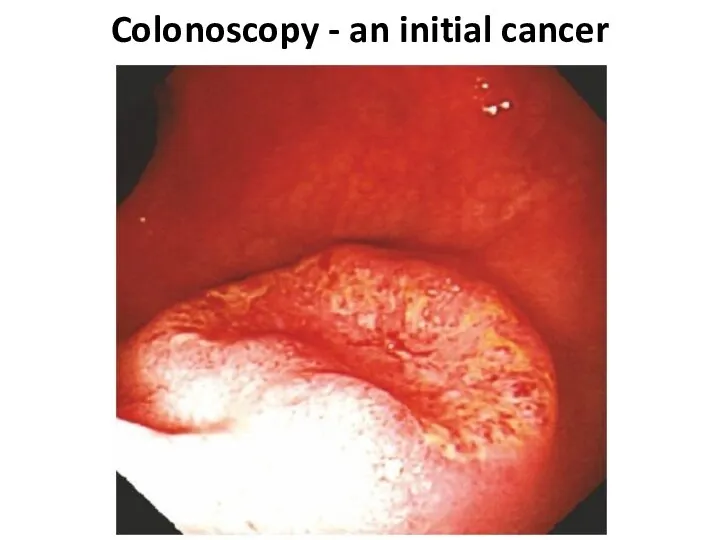
- 10. Colonoscopy - an initial cancer
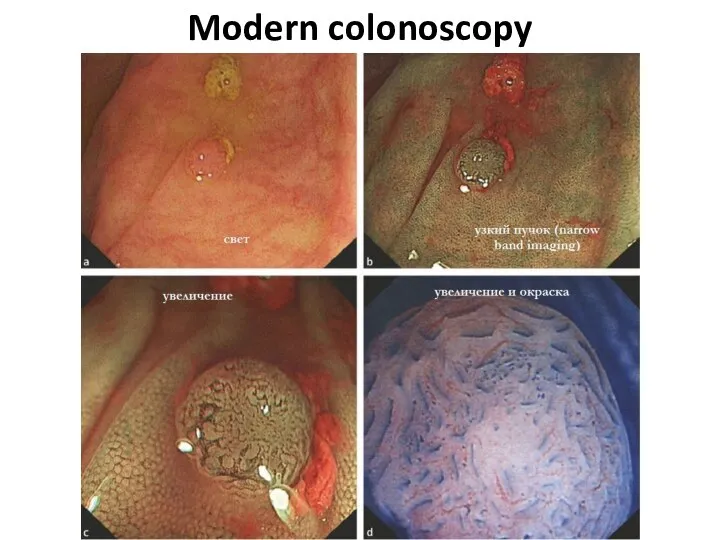
- 11. Modern colonoscopy
- 12. Special investigation methods 4. irrigoscopy (including virtu-al) 5. abdominal cavity US 6. radial methods (CТ, PET,
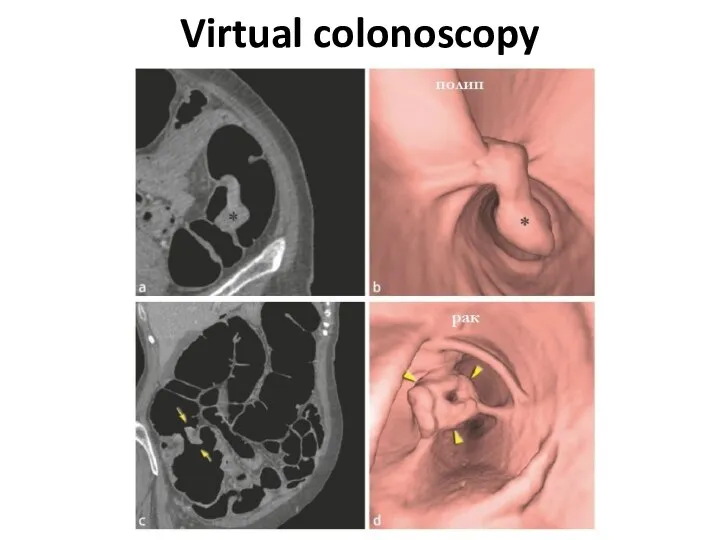
- 13. Virtual colonoscopy
- 14. At what a cancer localization more often anemy?
- 15. At what a cancer localization more often Visible bleeding?
- 16. AT WHAT A CANCER LOCALIZATION MORE OFTEN Disturbance of passability
- 17. AT WHAT A CANCER LOCALIZATION MORE OFTEN Perforation is more possible?
- 18. AT WHAT A CANCER LOCALIZATION MORE OFTEN Fistulas, phlegmons are possible?
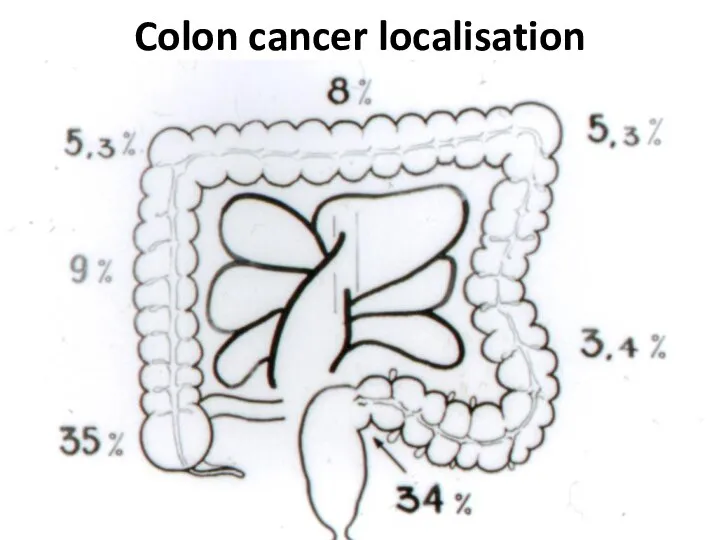
- 19. Colon cancer localisation
- 20. Cancer clinical signs 1. Functional signs without intestinal disorders (a pain, etc.) 2. Intestinal disorders (diarrheas,
- 21. Cancer clinical forms 1) toxico-anemic 2) enterocolitic 3) dyspeptic 4) obturational 5) pseudo-inflammatory 6) tumoral
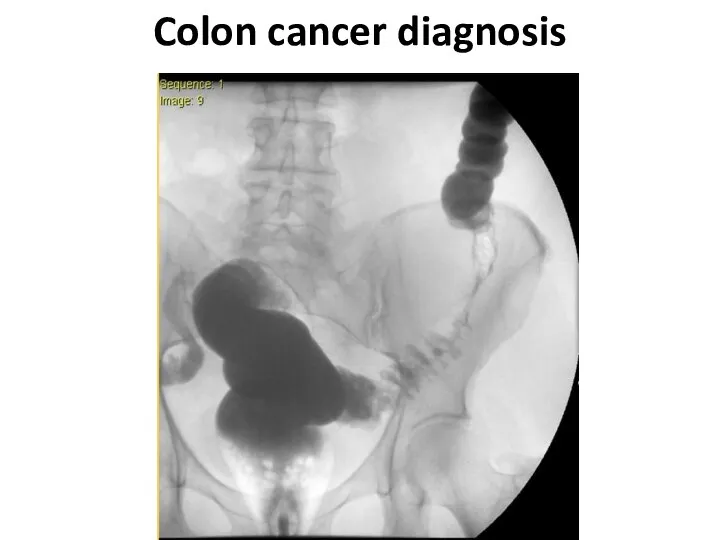
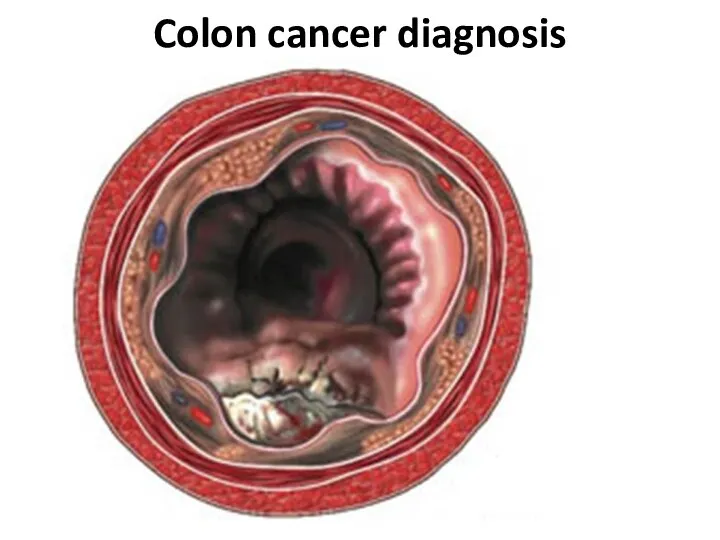
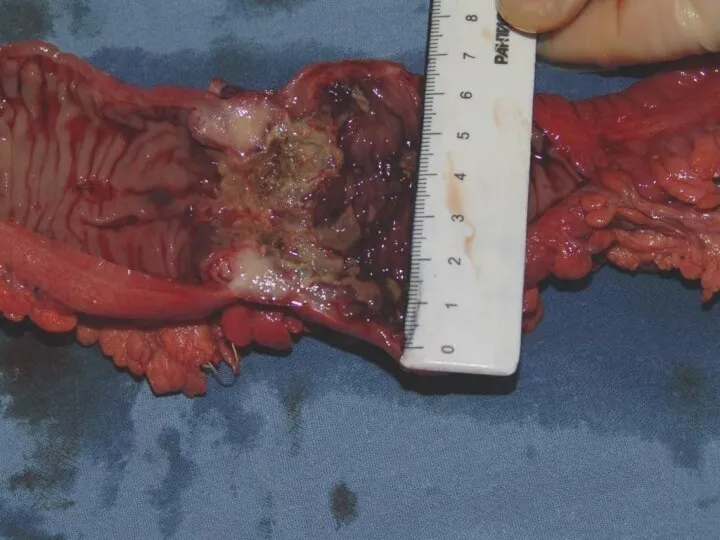
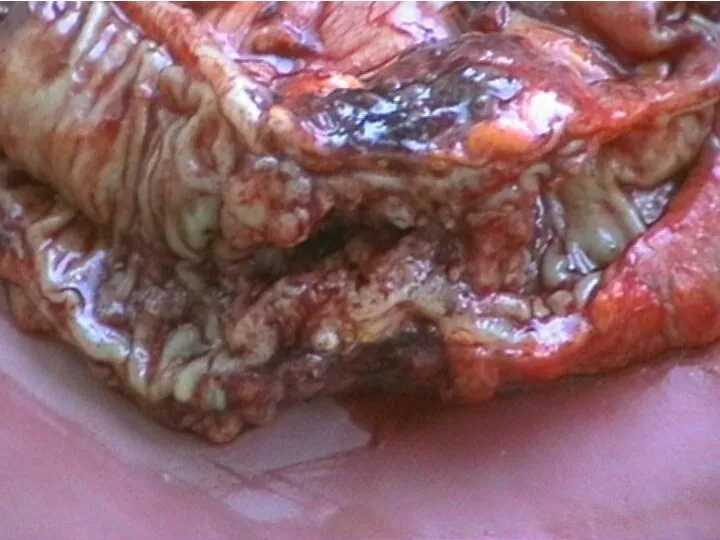
- 22. Colon cancer diagnosis
- 23. Colon cancer diagnosis
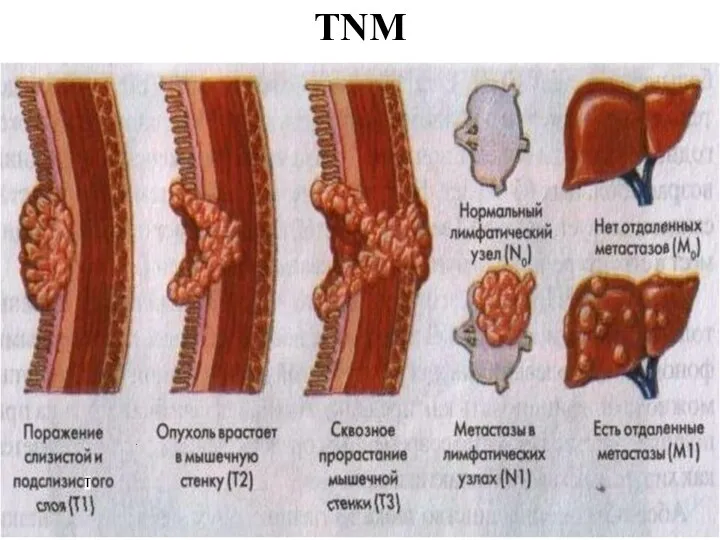
- 26. TNM
- 27. TNM - T Tx - the estimation of a primary tumour is impossible T0 - the
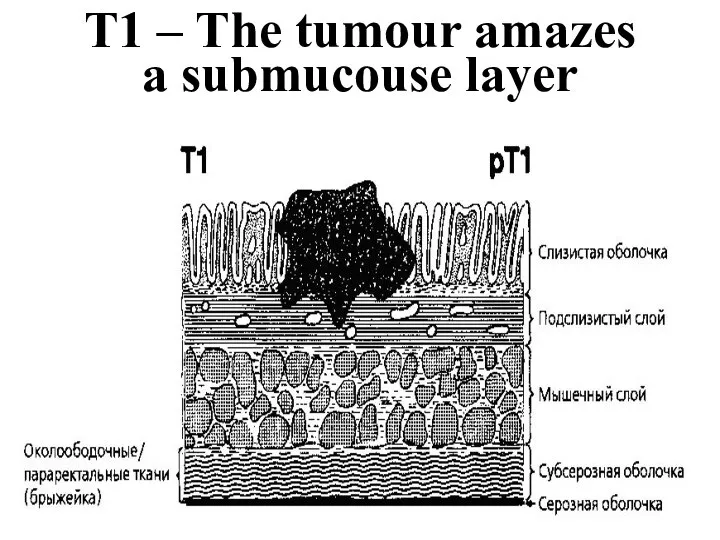
- 28. T1 – The tumour amazes a submucouse layer
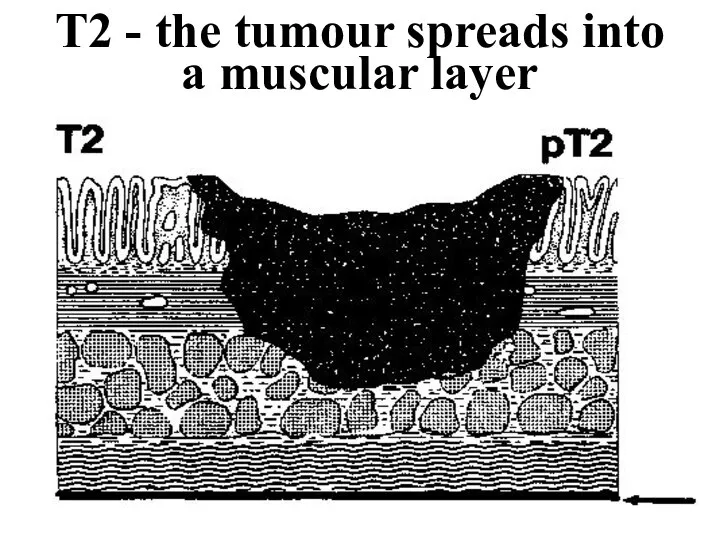
- 29. T2 - the tumour spreads into a muscular layer
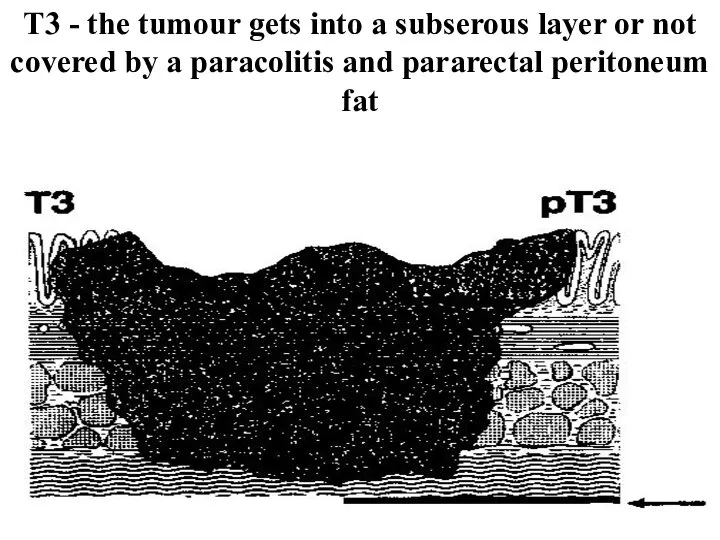
- 30. Т3 - the tumour gets into a subserous layer or not covered by a paracolitis and
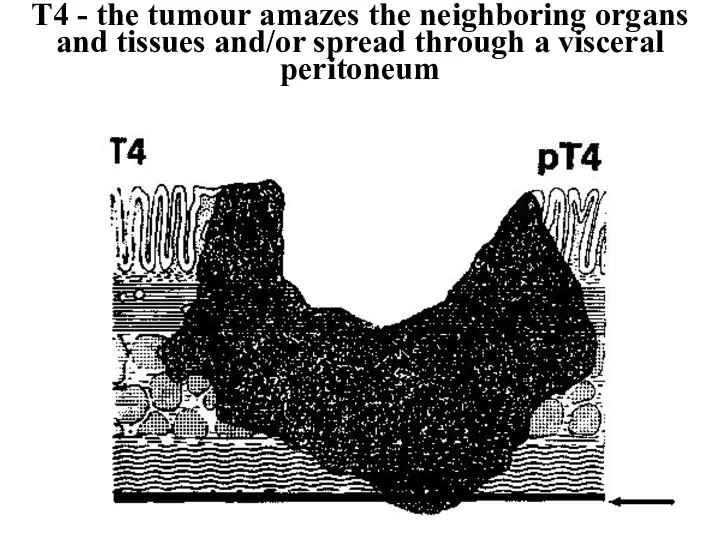
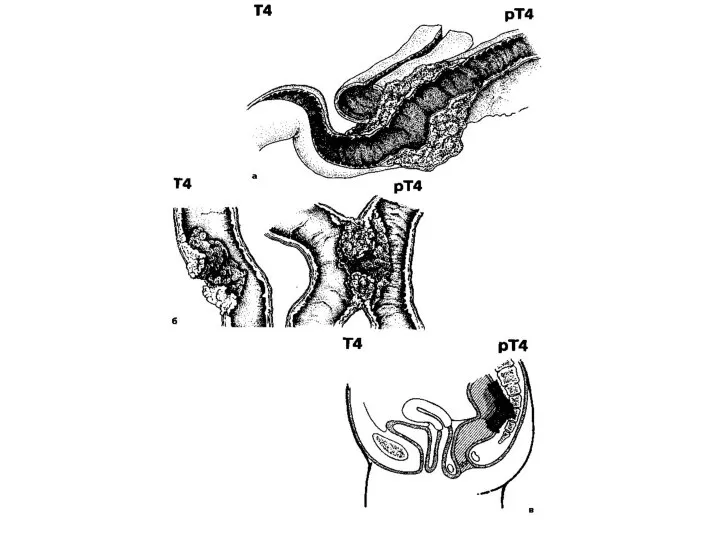
- 31. Т4 - the tumour amazes the neighboring organs and tissues and/or spread through a visceral peritoneum
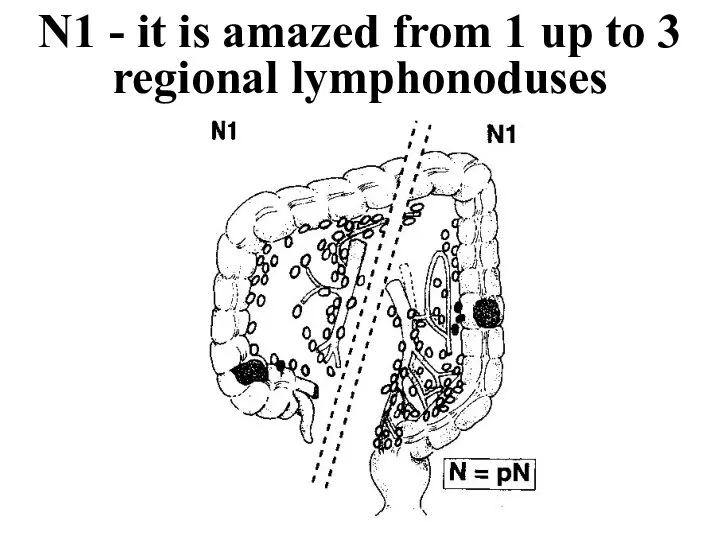
- 33. N1 - it is amazed from 1 up to 3 regional lymphonoduses
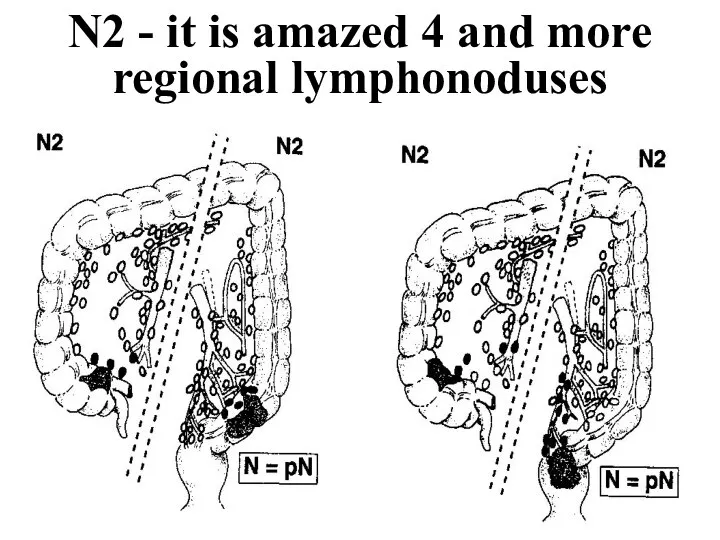
- 34. N2 - it is amazed 4 and more regional lymphonoduses
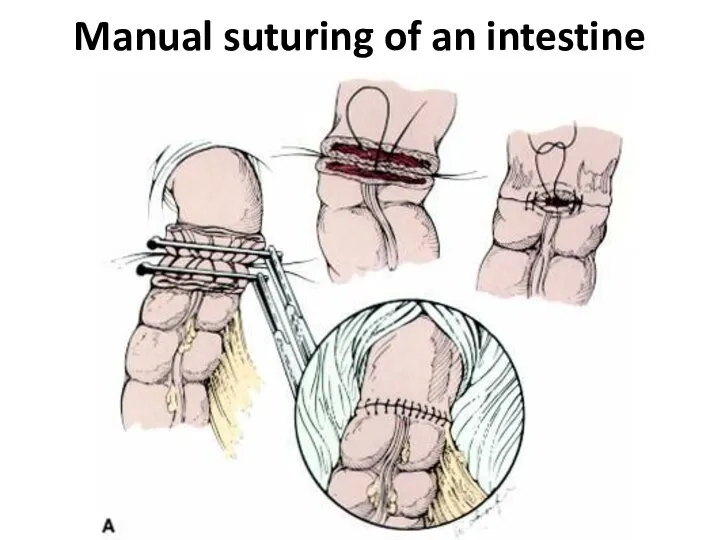
- 35. Manual suturing of an intestine
- 36. Staplers
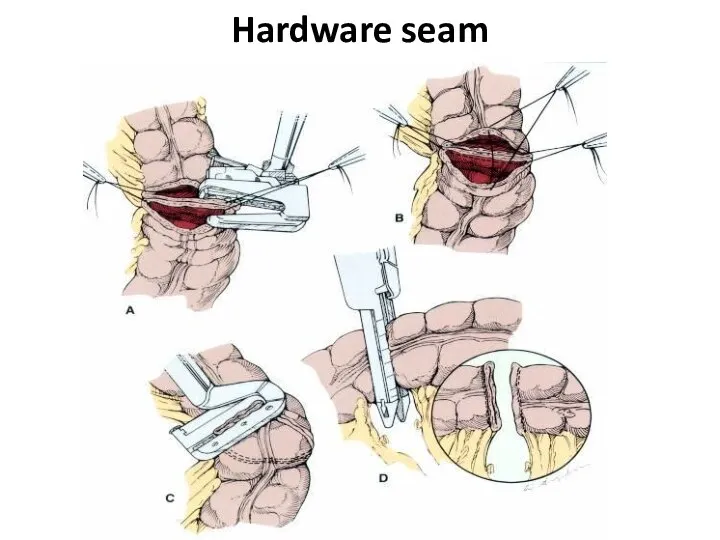
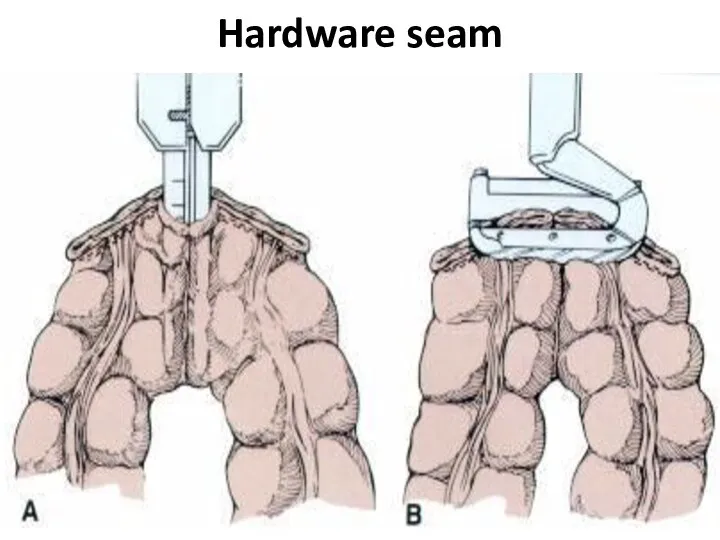
- 37. Hardware seam
- 38. Hardware seam
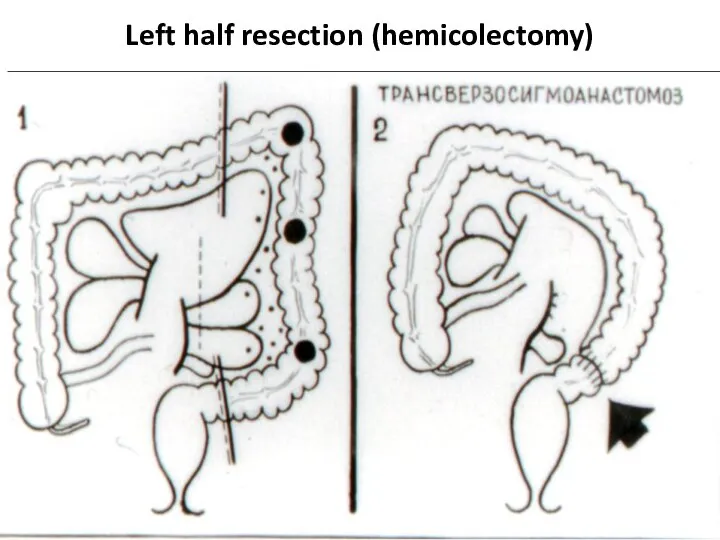
- 39. Left half resection (hemicolectomy)
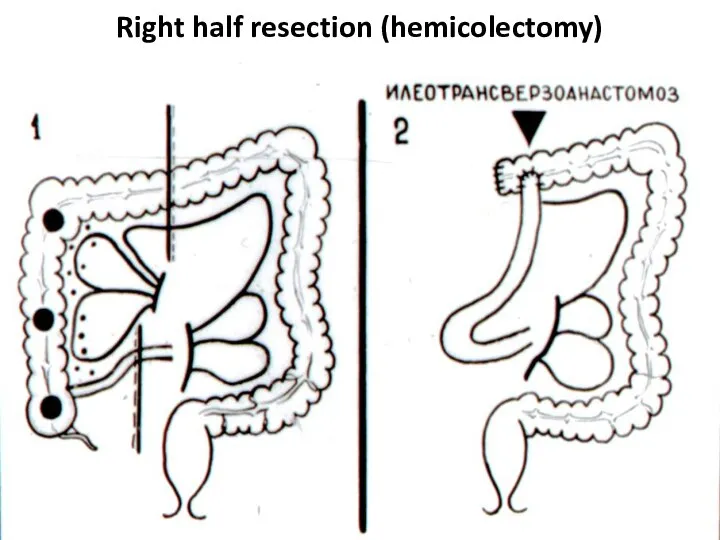
- 40. Right half resection (hemicolectomy)
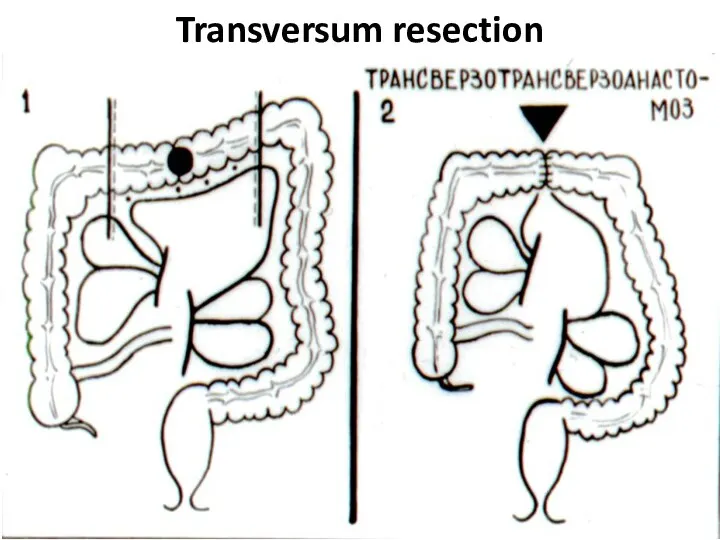
- 41. Transversum resection
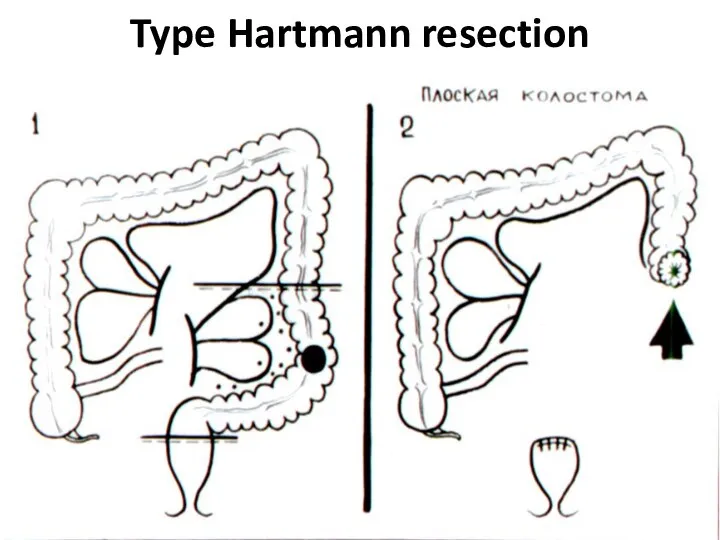
- 42. Type Hartmann resection
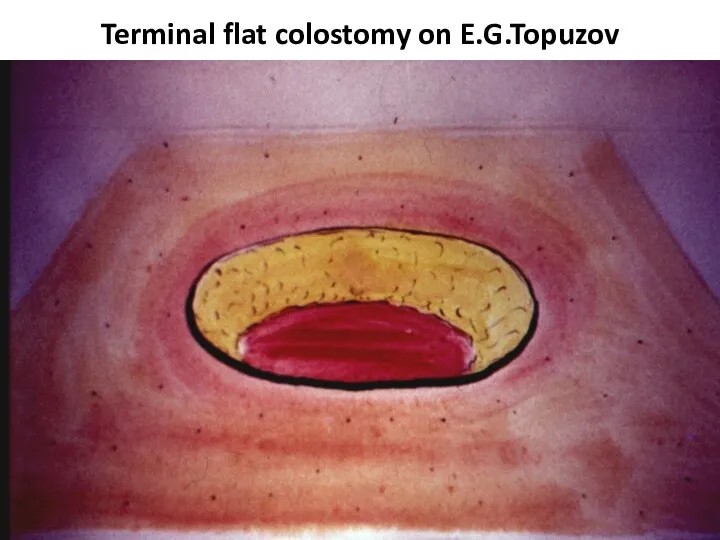
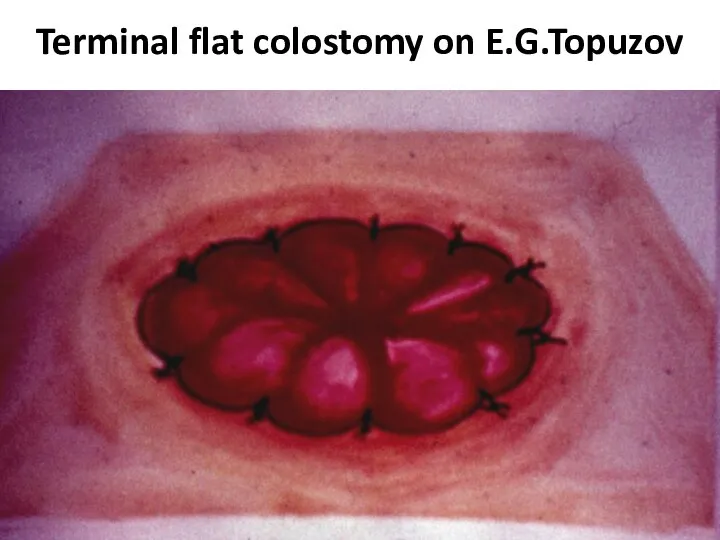
- 43. Terminal flat colostomy on E.G.Topuzov
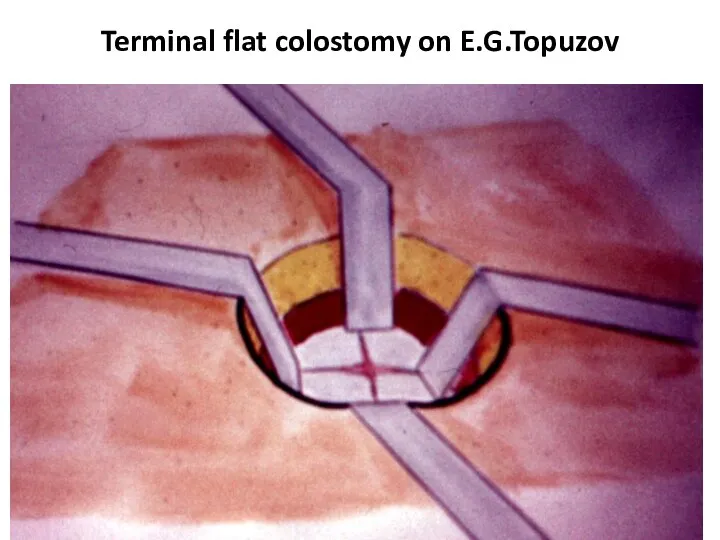
- 44. Terminal flat colostomy on E.G.Topuzov
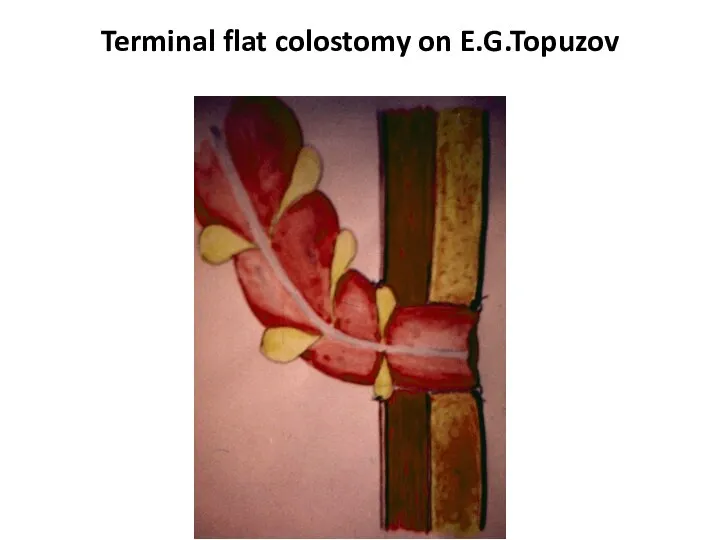
- 45. Terminal flat colostomy on E.G.Topuzov
- 46. Terminal flat colostomy on E.G.Topuzov
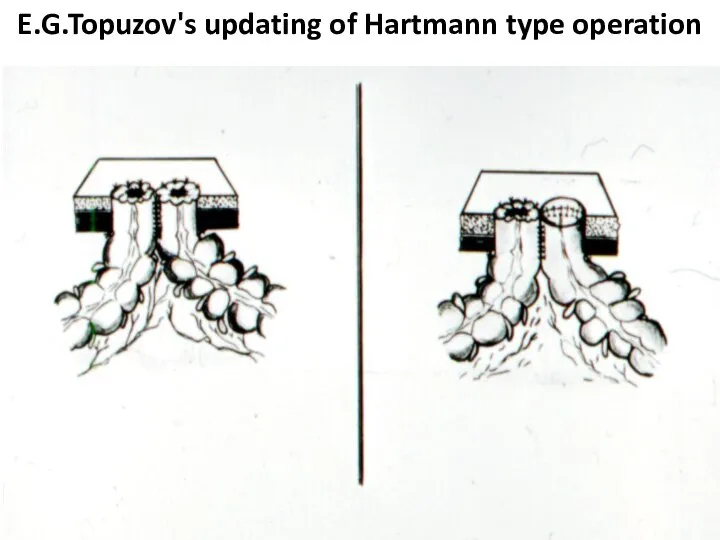
- 47. E.G.Topuzov's updating of Hartmann type operation
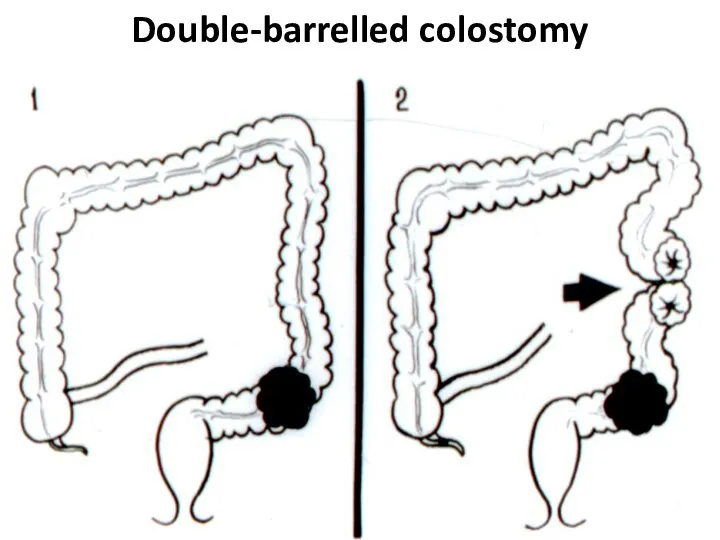
- 48. Double-barrelled colostomy
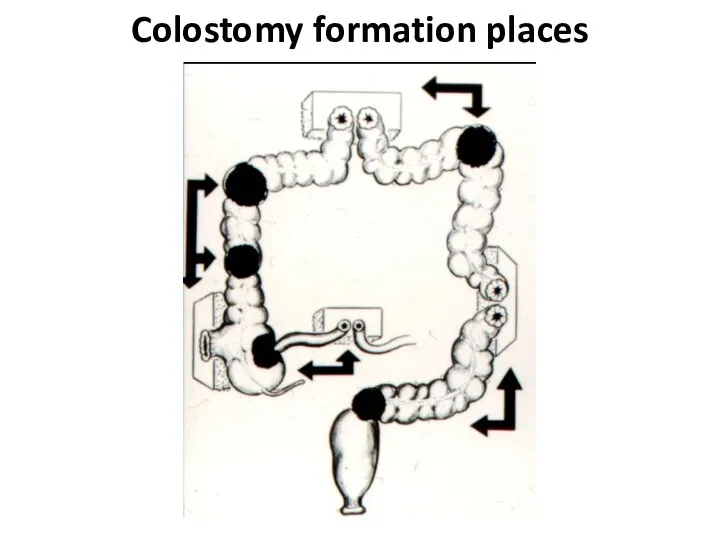
- 49. Colostomy formation places
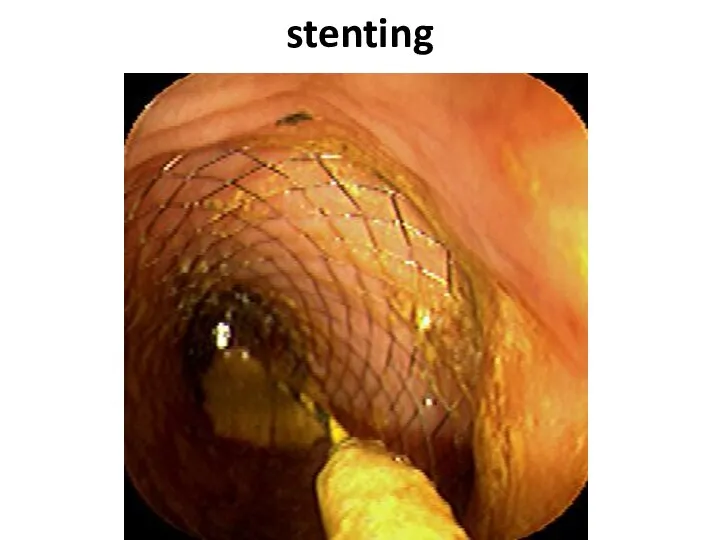
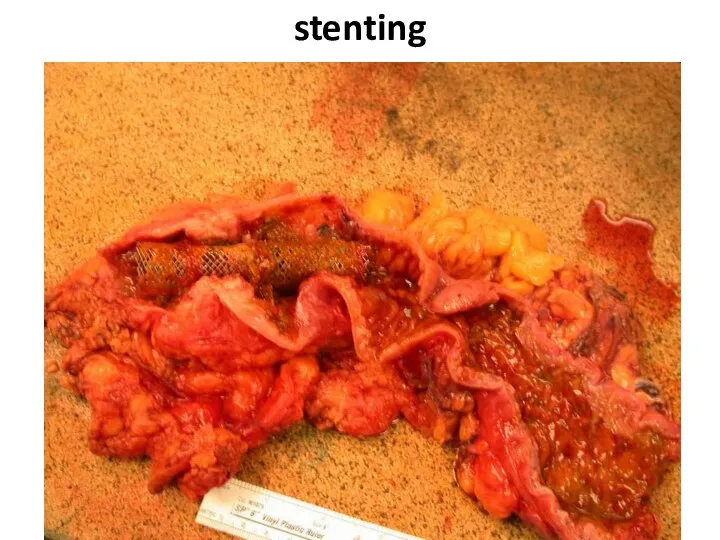
- 50. stenting
- 51. stenting
- 52. complications The intestinal obstruction is most typical for a tu-mor localization in the colon left half
- 53. complications The inflammation in tissues surrounding a tumour (up to phlegmon or abscess de-velopment) is marked
- 54. Question Pain in the right ileal region, a tumour and a heat. With what diseases you
- 55. complications Perforation of an intestine can be as in a zone of the tumour, at its
- 56. Question At what colon can-cer complication Schetkin-Blumberg sign more often is defined?
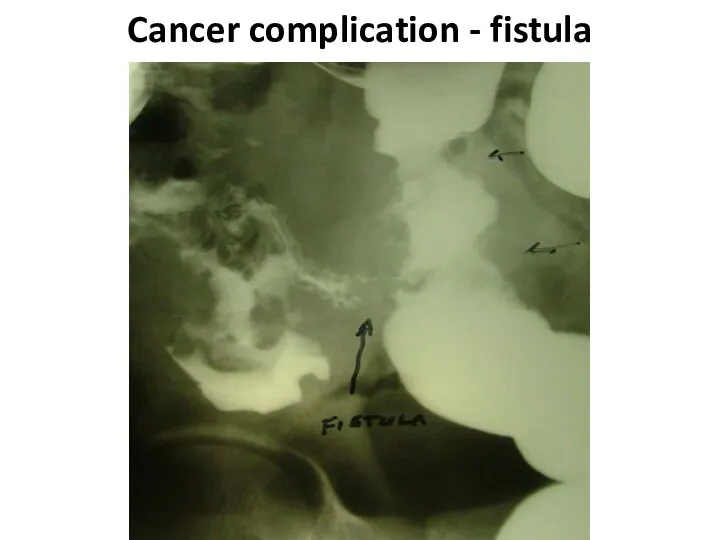
- 57. complications Formation of fistulas at spreading at the nea-rest hollow organs (co-lo-small intestinal, co-lo-gastric, colo-vesical) carry
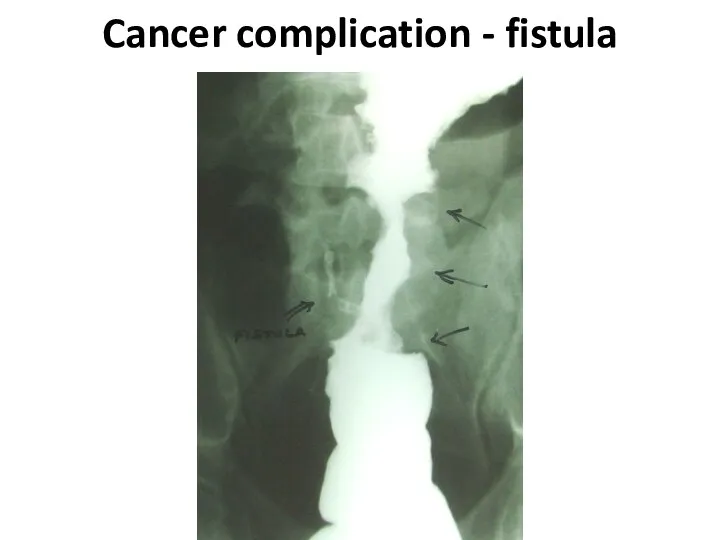
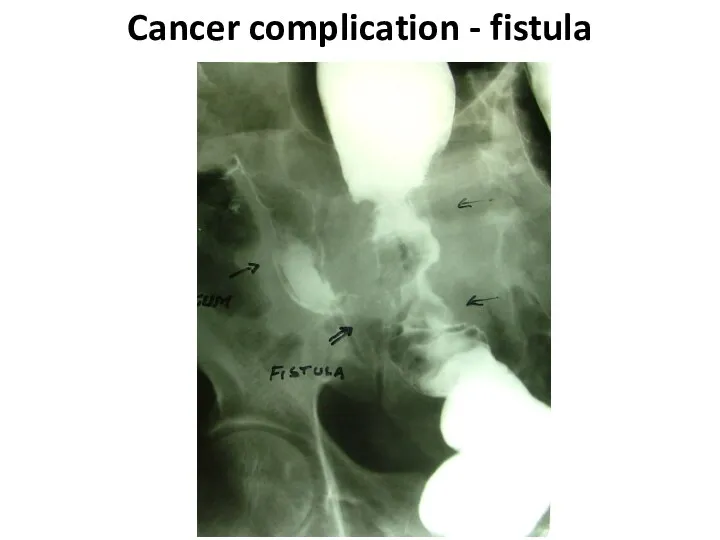
- 58. Cancer complication - fistula
- 59. Cancer complication - fistula
- 60. Cancer complication - fistula
- 61. complications The intestinal bleeding happens, as a rule, insig-nificant. Sometimes it is shown in the form
- 62. Colon diseases
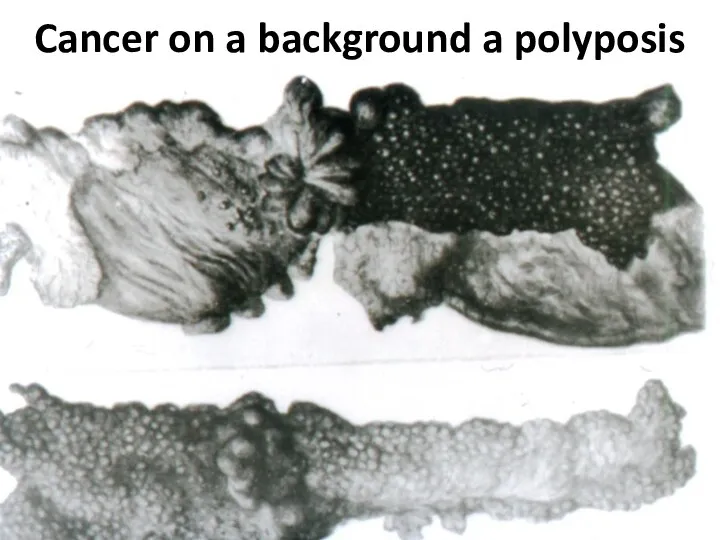
- 63. Cancer on a background a polyposis
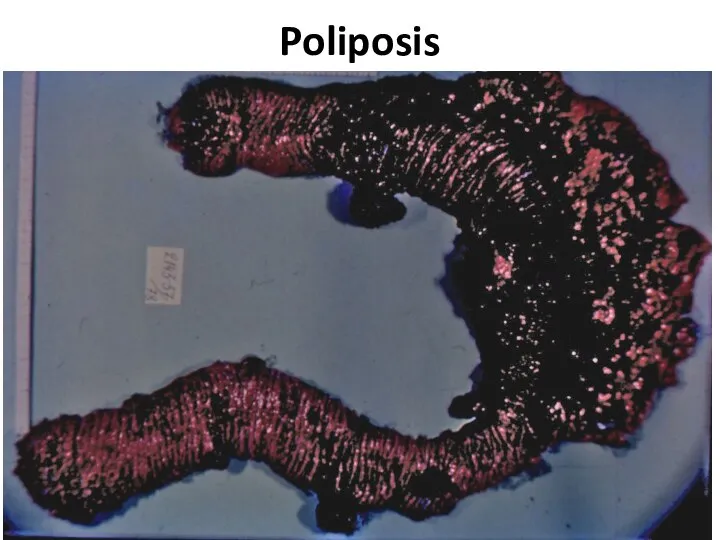
- 64. Poliposis
- 65. Nonspecific colitises 1. Ulcerouse 2. Granulomatous (Crohn's disease) 3. Ischemic
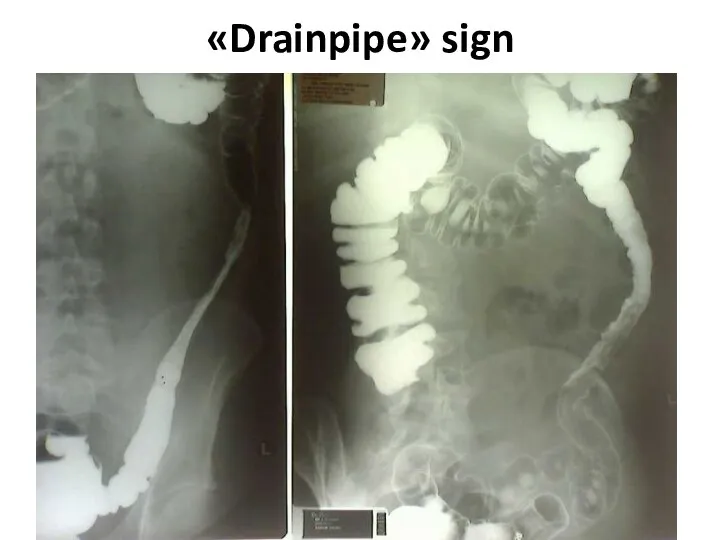
- 66. «Drainpipe» sign
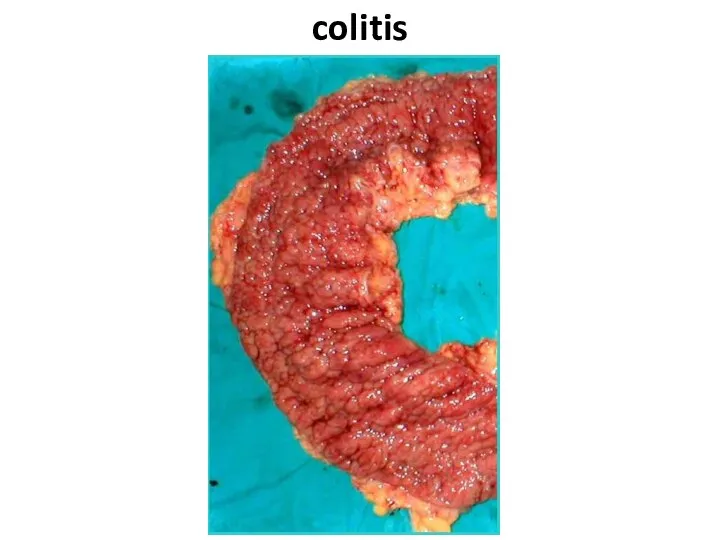
- 67. colitis
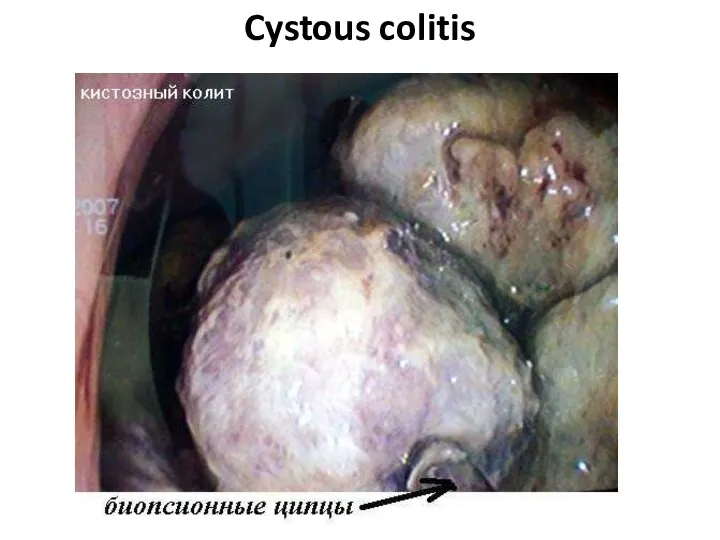
- 68. Cystous colitis
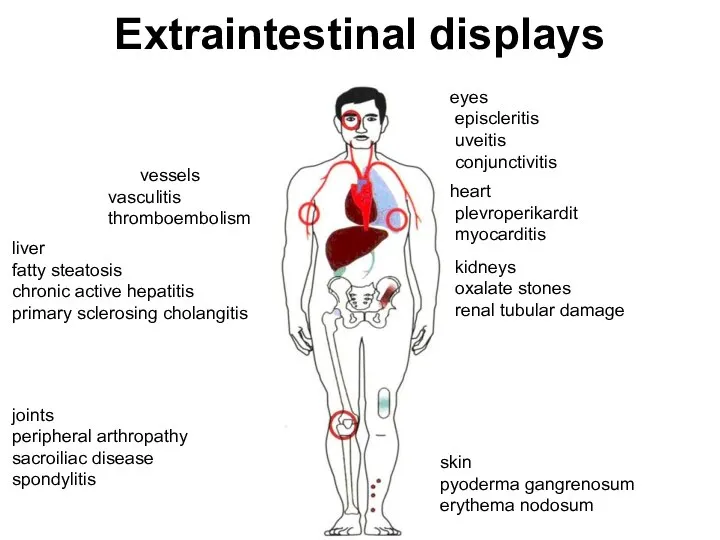
- 69. Extraintestinal displays vessels vasculitis thromboembolism liver fatty steatosis chronic active hepatitis primary sclerosing cholangitis joints peripheral
- 70. complications Toxic megacolon Perforation Peritonitis Intestinal obstruction Bleedings Abscesses Fistulas Infiltrates
- 71. Indications to operation at ulcerouse colitis Intestinal bleeding. 1. The frequency of bowel movements 12 or
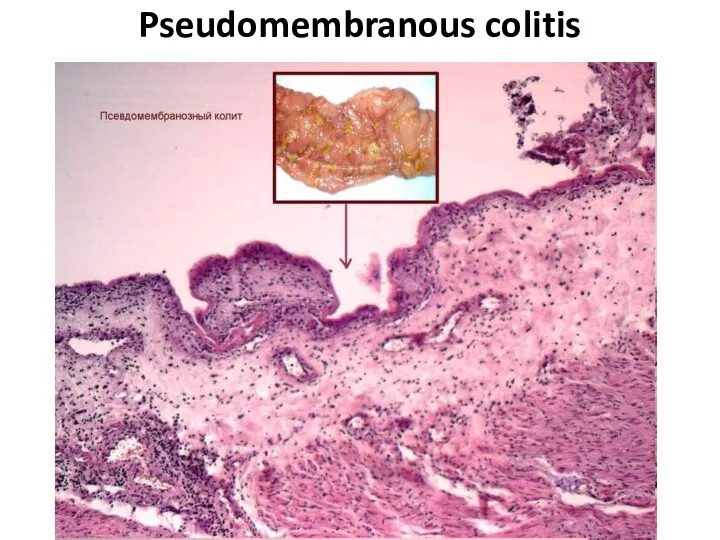
- 72. Pseudomembranous colitis
- 73. Polips Hyperplastic Tubular adenoma Tubulary-villiferous adenoma Villiferous adenoma
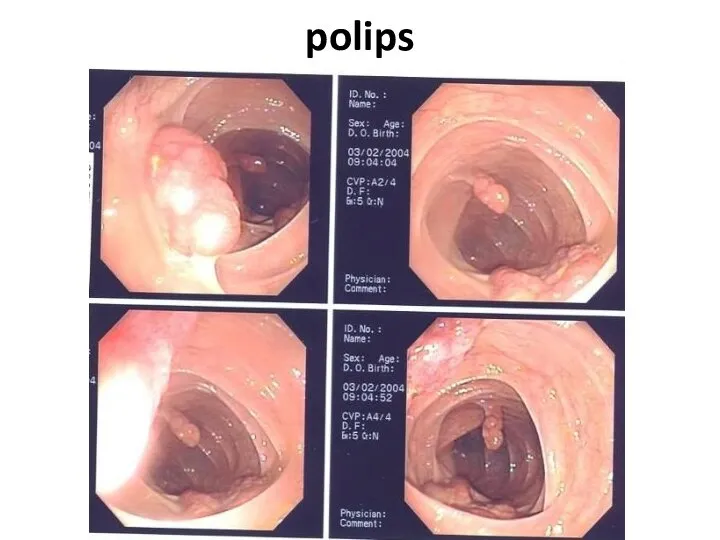
- 74. polips
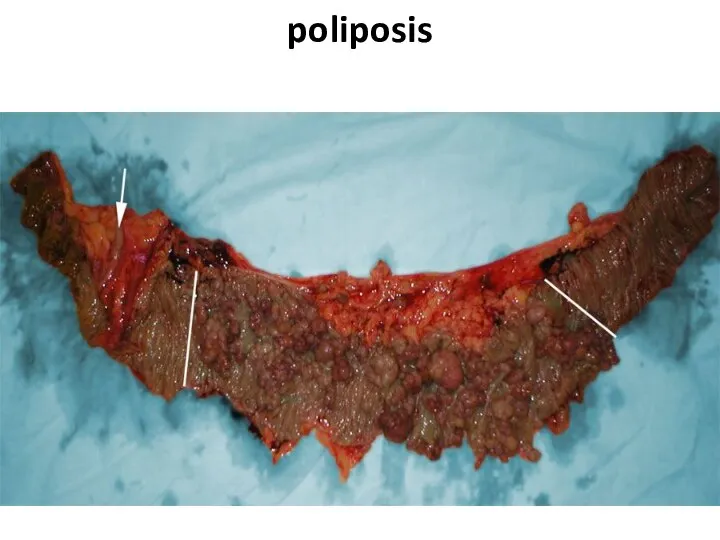
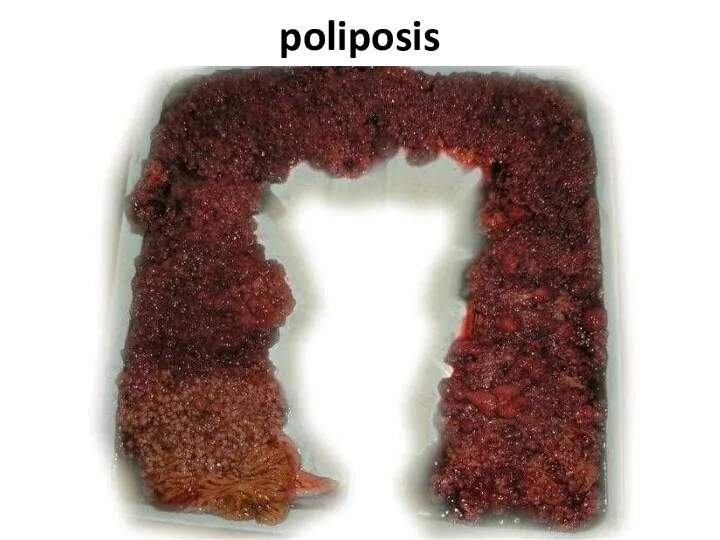
- 75. poliposis
- 76. poliposis
- 77. Congenital diseases 1. Hirshsprung disease 2. Megacolon 3. Dolichocolon
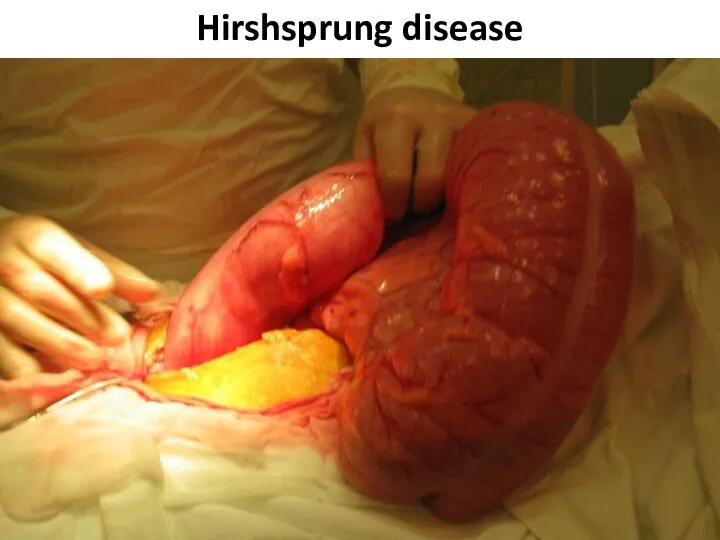
- 78. Hirshsprung disease
- 79. Differential diagnostics 1. Myxedema 2. Medicinal influences (morphinum and so forth) 5. Depressions 6. Schizophrenia 7.
- 80. diverticuls Diverticul Diverticulosis Diverticulitis
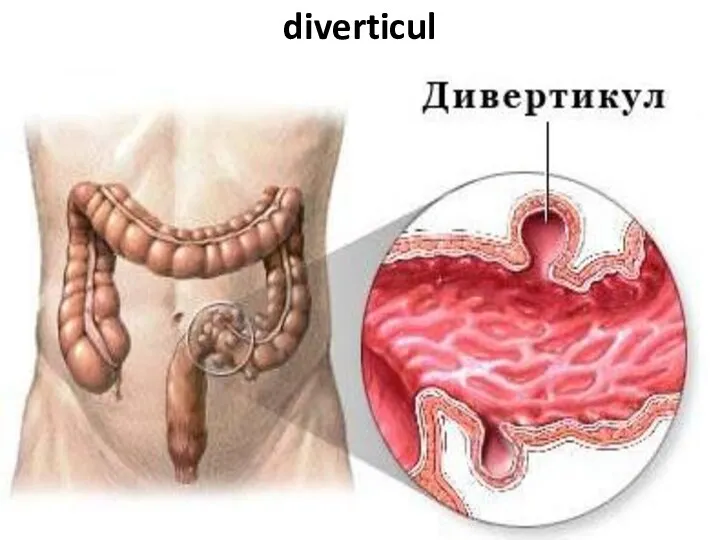
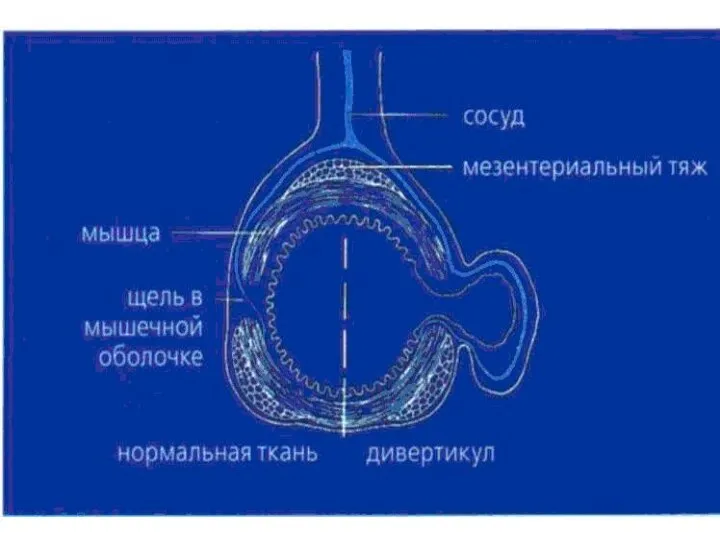
- 81. diverticul
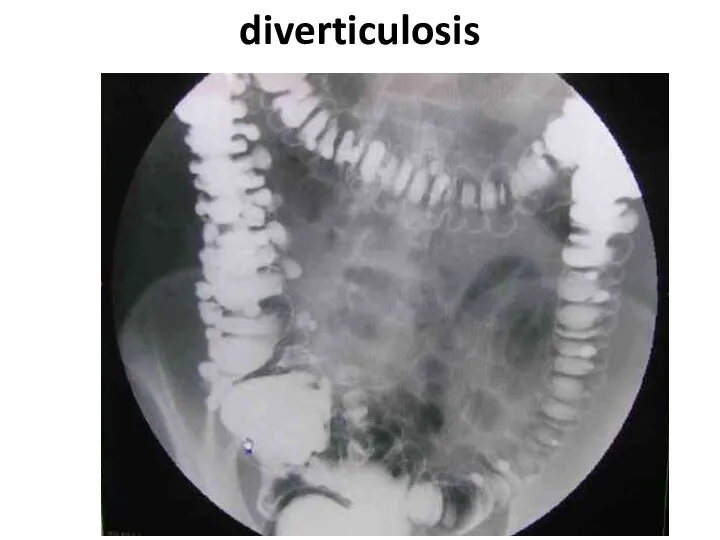
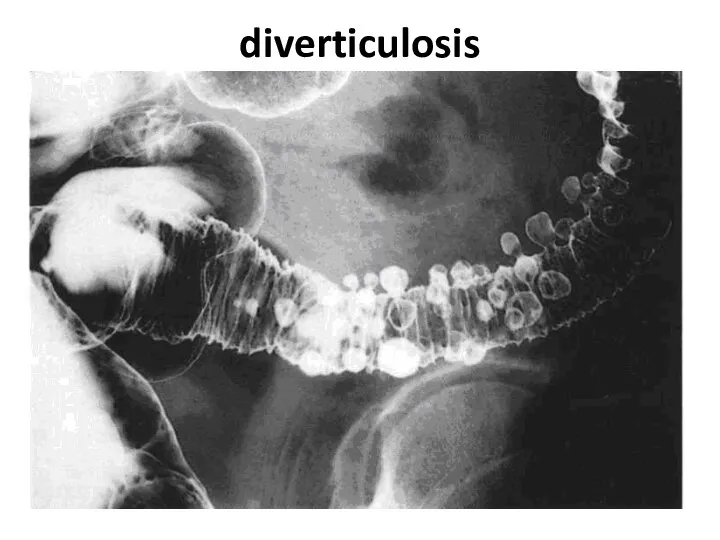
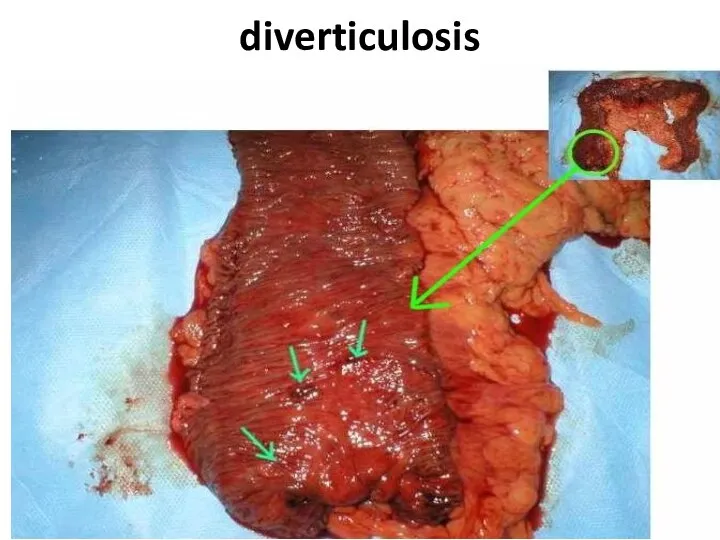
- 83. diverticulosis
- 84. diverticulosis
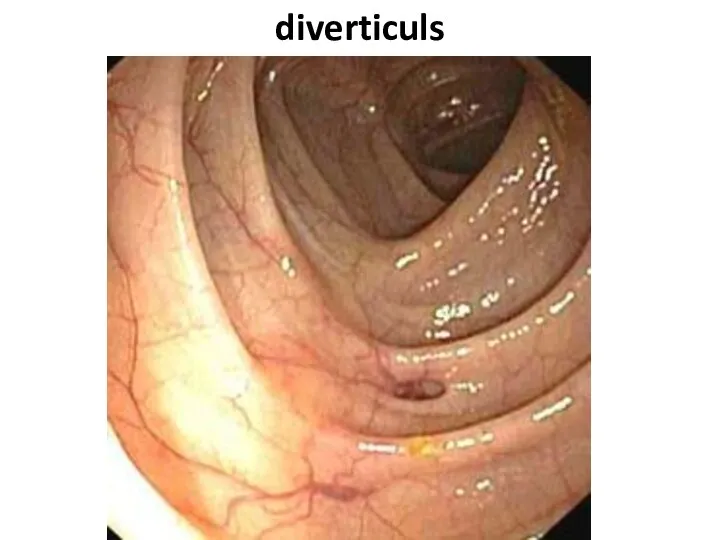
- 85. diverticuls
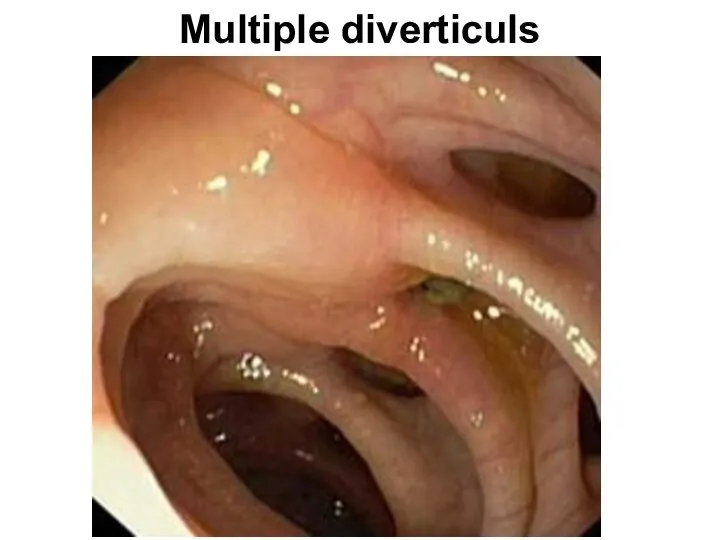
- 86. Multiple diverticuls
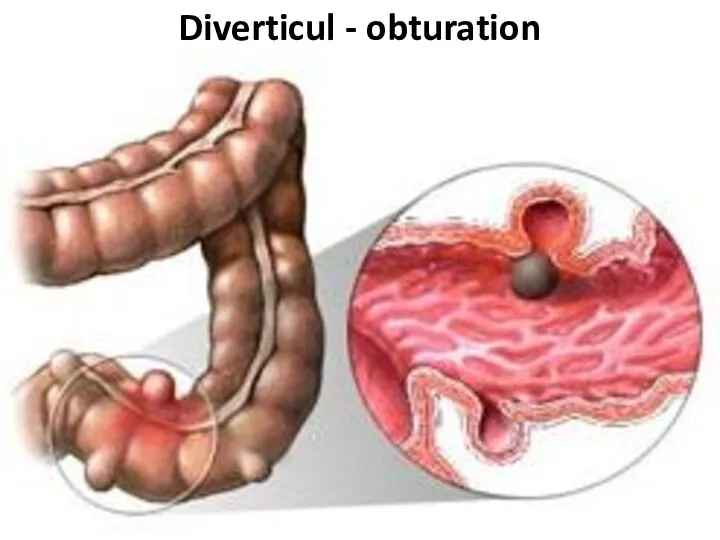
- 87. Diverticul - obturation
- 88. diverticulosis
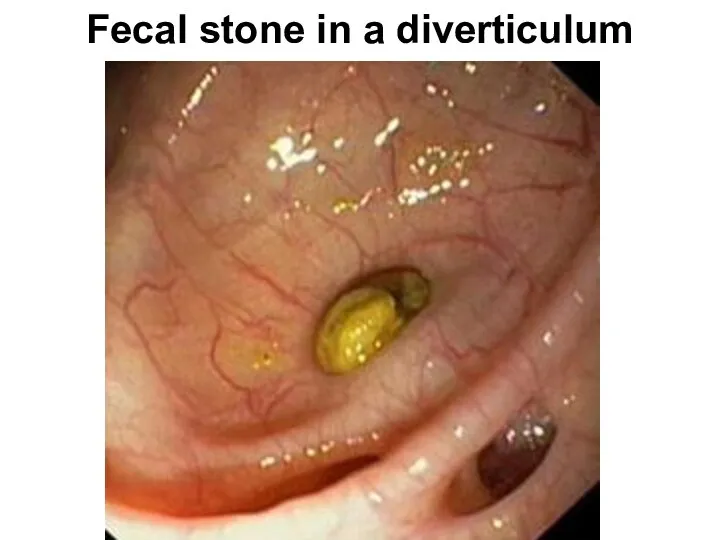
- 89. Fecal stone in a diverticulum
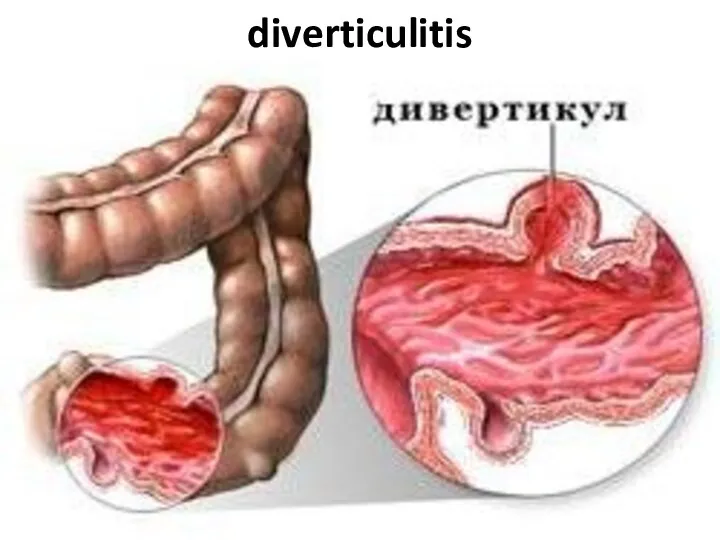
- 90. diverticulitis
- 91. Clinical features Acute diverticulitis is well nicknamed 'left-sided appendicitis'; an acute onset of central abdominal pain
- 92. Clinical features Chronic divertlcular disease exactly mimics the local clinical features of carcinoma of the colon;
- 93. Diverticulitis This results from infection of one or more divertlcula. An inflamed diverticulum may. 1. Perforate:
- 94. Diverticulitis The Hinchey classification - proposed by Hinchey et al. in 1978[1] classifies a colonic perforation
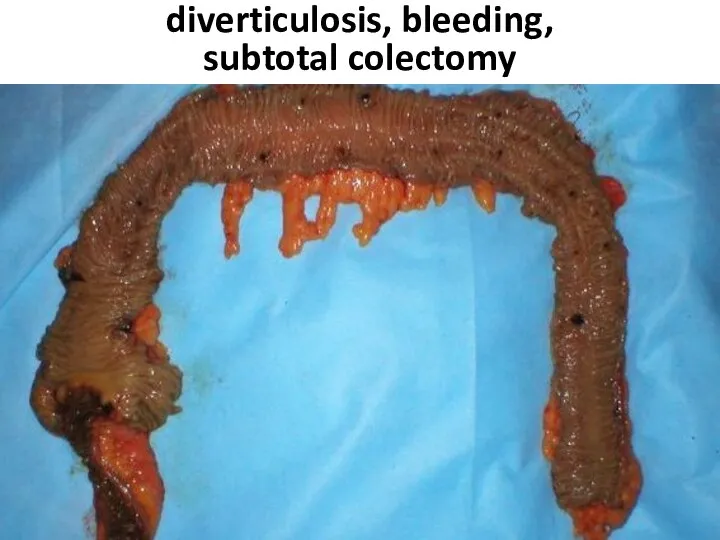
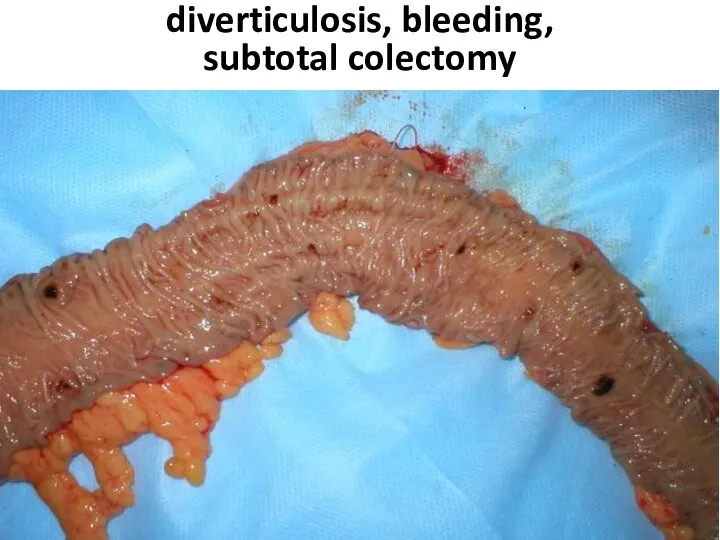
- 95. diverticulosis, bleeding, subtotal colectomy
- 96. diverticulosis, bleeding, subtotal colectomy
- 98. Скачать презентацию





























![Diverticulitis The Hinchey classification - proposed by Hinchey et al. in 1978[1]](/_ipx/f_webp&q_80&fit_contain&s_1440x1080/imagesDir/jpg/1165791/slide-93.jpg)
 Профилактика новой коронавирусной инфекции (COVID-19)
Профилактика новой коронавирусной инфекции (COVID-19) Роль гормонов в обмене веществ, росте и развитии организма
Роль гормонов в обмене веществ, росте и развитии организма Нормо- и гипотермическая машинная перфузия
Нормо- и гипотермическая машинная перфузия Слабительные препараты
Слабительные препараты Доброкачественные опухоли и опухолевидные образования челюстно-лицевой области
Доброкачественные опухоли и опухолевидные образования челюстно-лицевой области Mnogoplodnaya_beremennost
Mnogoplodnaya_beremennost Бредовые психозы позднего возраста
Бредовые психозы позднего возраста Основы рационального питания. Минеральные вещества
Основы рационального питания. Минеральные вещества Дети от матерей с токсикоманиями и наркоманиями
Дети от матерей с токсикоманиями и наркоманиями Лекарственные травы Алтая
Лекарственные травы Алтая Синдромна патологія анемій
Синдромна патологія анемій Операции на суставах
Операции на суставах ГОБ оконч
ГОБ оконч Эндодонтическое лечение
Эндодонтическое лечение Первая помощь при воздействии высоких и низких температур
Первая помощь при воздействии высоких и низких температур Биогенные стимуляторы
Биогенные стимуляторы Күмәнді мәліметтерді жариялау мәселесі
Күмәнді мәліметтерді жариялау мәселесі Поступление в организм, транспорт и распределение и выделение ядов. Кумуляция ядов в организме. Коэффициент кумуляции
Поступление в организм, транспорт и распределение и выделение ядов. Кумуляция ядов в организме. Коэффициент кумуляции Биоэтика и реализация соматических прав в странах Арабского мира
Биоэтика и реализация соматических прав в странах Арабского мира Кисты почек
Кисты почек Неотложные состояния
Неотложные состояния Травма живота
Травма живота СРС: Хламидиоз у детей
СРС: Хламидиоз у детей Расстройства настроения: биполярные аффективные расстройства
Расстройства настроения: биполярные аффективные расстройства Эшерихиозы. Эшерихии
Эшерихиозы. Эшерихии Тіс қақтары-әртүрлі факторлардың әсерінен тістердің бетінде пайда болатын шөгінділер
Тіс қақтары-әртүрлі факторлардың әсерінен тістердің бетінде пайда болатын шөгінділер Витамин Р
Витамин Р ВИЧ. Классификация
ВИЧ. Классификация